You feel it the moment your foot hits the first step. A dull ache. A sharp pinch around the kneecap. Maybe a grinding sensation that makes you grip the railing just to get through it. Stairs shouldn’t feel like a test of will. Yet for millions of people, they do.
Here’s what most people don’t know: that pain often has nothing to do with your knee.
The real trouble is hiding higher up. If stairs trigger pain around your kneecap, the true culprit is very likely your hips and core. These structures sit higher in your body’s movement chain, but they control everything below. When they’re weak or out of sync, your knee pays the price.
This is the part most treatment plans miss entirely.
The Common Misconception About Knee Pain
Think about how most people respond to knee pain. They ice it. They rest. They buy a brace. They do leg extensions at the gym to “strengthen the quad.” These steps aren’t wrong, but they’re incomplete.
The knee is a hinge. It bends and straightens. It doesn’t rotate, twist, or steer your leg on its own. The structures above and below it do that. So when the knee hurts, it’s often being pushed around by mechanics it can’t control.
Patellofemoral pain (PFP) is the formal name for knee pain that centers around the kneecap. It’s one of the most common complaints in active adults. It shows up during squats, running, and especially during stair climbing and descent. The kneecap glides in a groove at the end of the thigh bone. When everything lines up, this gliding is smooth. When it doesn’t, you feel it.
What determines that alignment? The muscles of your hip and core.
Treating the knee in isolation is like fixing a tire when the real problem is the alignment of the whole car. You can patch the tire, but it’ll keep wearing down until you fix the root cause.
The Science of Stair Descent: Why Going Down Is Harder Than Going Up
Most people assume going up stairs is harder than going down. Biomechanics tells a different story.
When you descend a staircase, your knee bears a load that can reach up to four times your body weight. That’s not a typo. Every step down is a controlled fall where your muscles work to slow and stabilize the drop. The forces involved are enormous, and they concentrate at the knee joint, specifically behind the kneecap.
Here’s where hip mechanics enter the picture in a big way.
A landmark 2010 biomechanics review by Powers examined how hip kinematics affect knee joint stress. The findings were clear: when the thigh bone rotates inward during movement, a pattern called femoral internal rotation, the kneecap is pulled outward and off-track. This misalignment dramatically multiplies the stress placed on the joint, especially during weight-bearing tasks like stair descent.
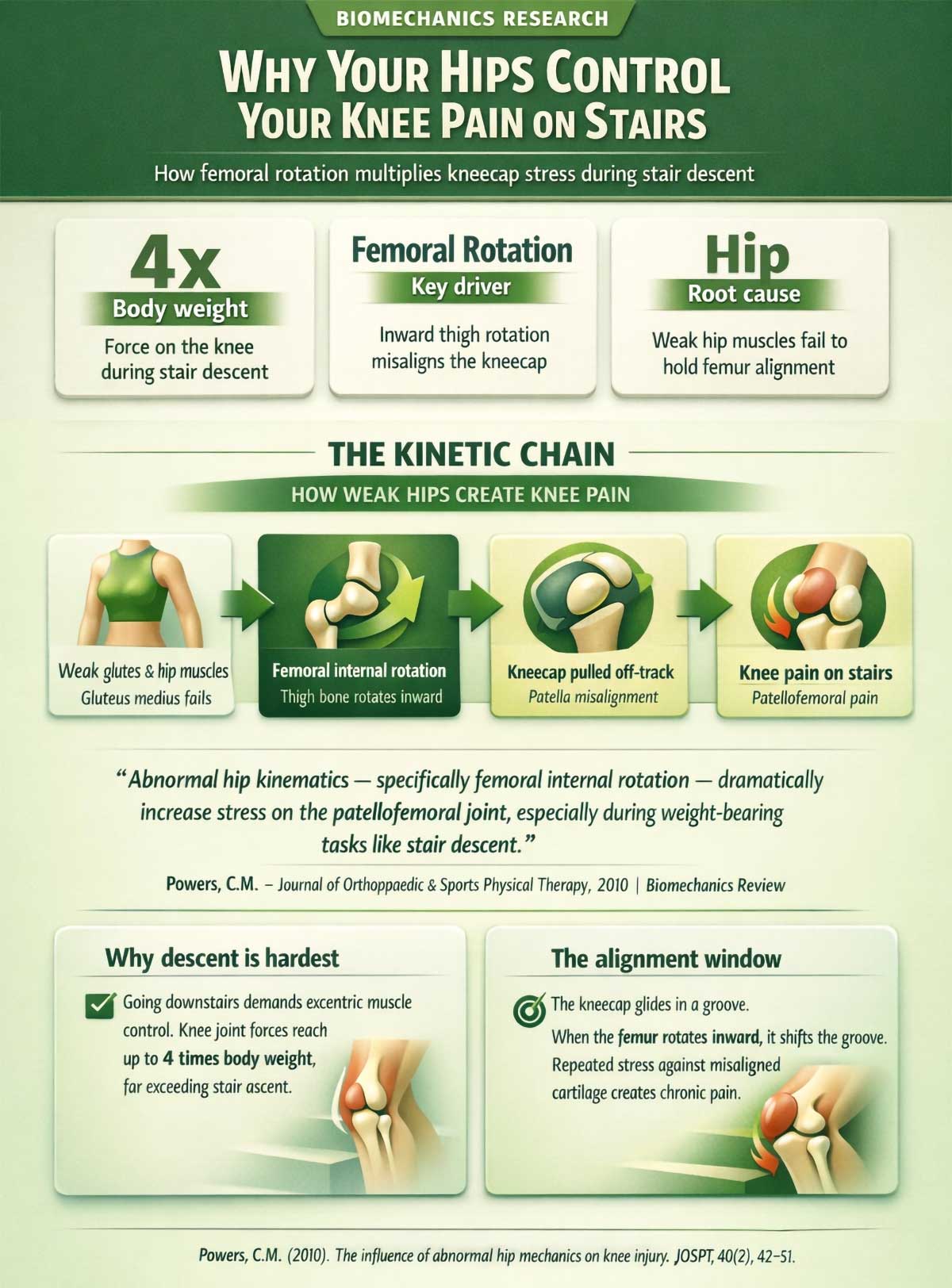
What causes femoral internal rotation? Weak hip muscles. Specifically, the gluteus medius and external rotators on the side and back of the hip. When these muscles can’t hold the thigh in proper alignment, the leg caves inward. The kneecap drags along with it.
This is the biomechanical domino effect. Weak hips cause the thigh to rotate inward. The inward rotation pulls the kneecap off its groove. The kneecap grinds. You feel pain on the stairs.
The knee isn’t failing you. It’s being failed by the structures above it.
The Glute Connection: Why Fixing the Hip Fixes the Knee
This brings us to one of the most important shifts in modern rehab thinking.
Traditional physical therapy for kneecap pain has long focused on the quadriceps, the large muscle group at the front of the thigh. And quads matter. But they’re not the whole picture. In many cases, they’re not even the main character.
A 2015 randomized controlled trial by Ferber and colleagues tested this idea directly. They compared a hip and core strengthening program against a traditional knee-focused program in people with patellofemoral pain over six weeks. The hip-focused group showed an earlier and faster reduction in pain. The improvement came sooner and was more consistent.
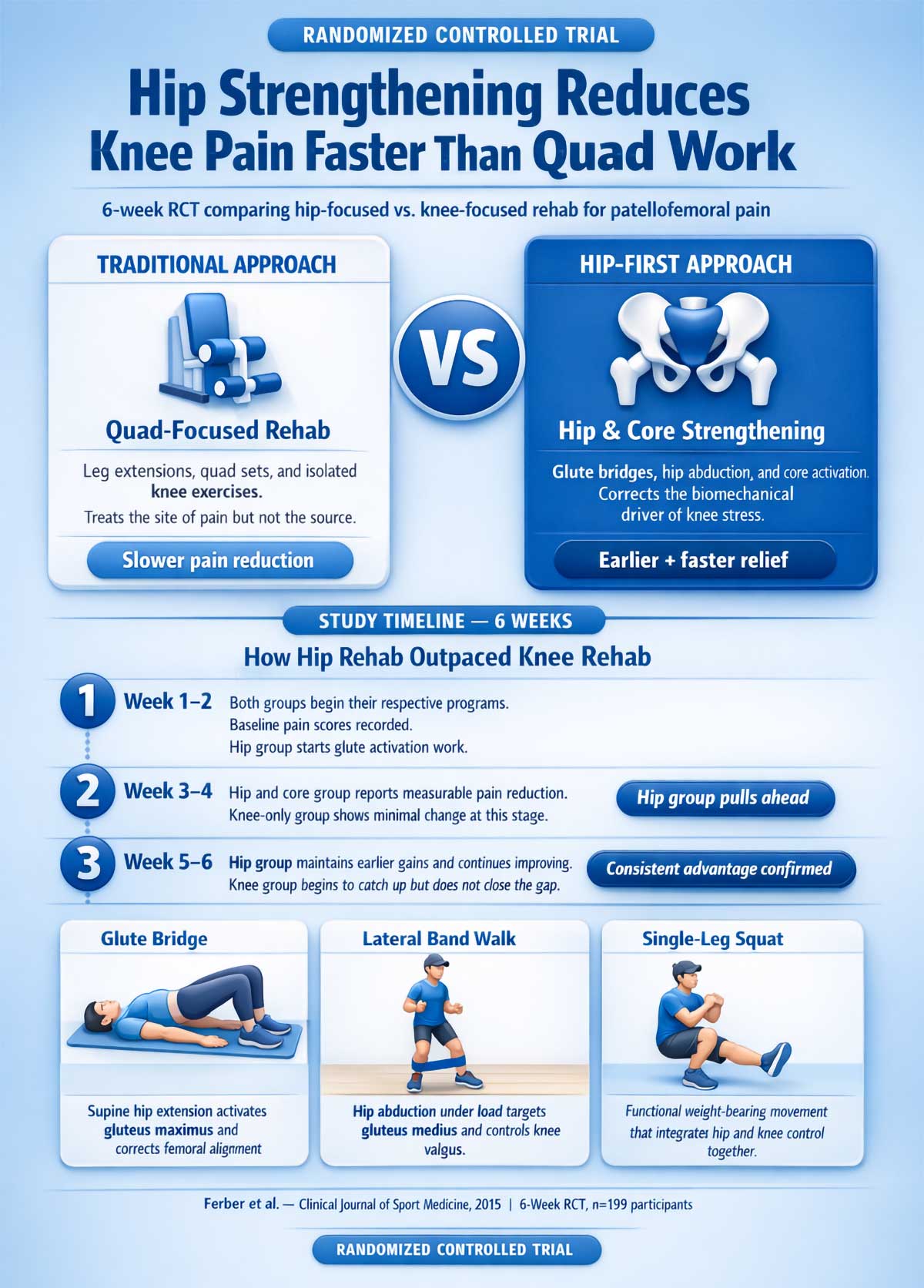
Why does this work? Because strengthening the glutes and hip muscles puts the femur back in its correct position. When the hip holds the thigh properly aligned, the kneecap glides smoothly. The grinding stops. The stress drops.
The two exercises with the strongest track record for this are glute bridges and lateral band walks. These movements target the gluteus medius and gluteus maximus in a way that directly improves how the femur tracks during movement. They aren’t glamorous. They don’t require a gym. But they work.
A glute bridge is performed lying on your back with knees bent. You push through your heels to lift your hips off the floor, squeezing the glutes at the top. A lateral band walk uses a resistance band looped around the ankles or just above the knees. You take slow, controlled steps sideways, keeping the knees from caving inward.
These movements teach the hip muscles to fire and hold. That’s exactly what they need to do on the stairs.
The Winning Combination: Hips and Knees Together
Here’s where the science gets very specific about what works best.
A 2016 consensus statement by Crossley and colleagues reviewed the available evidence on treating patellofemoral pain. Their conclusion was firm: combining hip and knee exercises is strictly recommended over knee exercises alone for people with weight-bearing pain. Neither approach alone produces the best results. Together, they do.
This was reinforced by a 2015 systematic review and meta-analysis by Lack and colleagues. After analyzing multiple clinical trials, the authors confirmed that combining hip strengthening with traditional quadriceps rehab produces the most solid short-term and long-term relief from kneecap pain.
The practical takeaway is this: don’t abandon quad work. The quads are part of the solution. A strong quad helps the kneecap track better and absorbs load at the knee. But the ratio needs to shift. If your program is 90% knee-focused, move it toward 50/50. Add glute bridges, hip abduction work, and lateral control exercises alongside your quad sets and step-downs.
Think of it as building a team rather than relying on a single player. The hip steers. The quad absorbs. Both need to be strong and working together.
The Chicken or the Egg: Did Weak Hips Cause the Pain?
Here’s a question that often comes up: did weak hips cause your knee pain in the first place? Or did the knee pain cause the hip weakness?
This matters more than it might seem, because the answer changes how you think about recovery.
A 2014 systematic review by Rathleff and colleagues looked at this question carefully. What they found was striking. Hip strength deficits are often a result of knee pain rather than a cause of it. When the knee hurts, the whole limb moves differently. The hip muscles are used less. They weaken over time from disuse and altered movement patterns.
So the hip weakness you have now may not be why your knee started hurting. It may be a consequence of the pain itself.
This reframes the goal. Whether weak hips came first or developed second, rebuilding hip capacity is non-negotiable. The hip muscles need to be restored to normal function before the movement pattern can correct itself. Waiting for the pain to go away before starting hip work is waiting for the wrong thing. The hip work is part of what makes the pain go away.
The good news is that this cycle can be broken. Restoring hip strength improves movement quality, which reduces stress on the knee, which reduces pain, which allows more normal movement, which further restores hip strength. It’s a positive loop once you get it started.
The Pace of Healing: Why Managing Load Matters
There’s one more piece that most rehab plans overlook, and it’s arguably just as important as the exercises themselves. It’s how much you do and how fast you ramp it up.
For years, the standard advice for any joint pain was RICE: Rest, Ice, Compression, Elevation. Rest was king. The idea was that reducing activity would reduce stress on the tissue and allow it to heal.
We now know this is incomplete. The tissue doesn’t just need rest. It needs the right amount of load at the right time.
A 2017 randomized controlled trial by Esculier and colleagues followed runners with patellofemoral pain over eight weeks. One of the key findings was that education on pacing and load management was just as critical to reducing symptoms as the strengthening work itself. When people understood how to modulate their activity, how to stay just below the pain threshold rather than pushing through it or avoiding movement entirely, they recovered faster and more completely.

This is called load management. It means your daily activity level, how many stairs you climb, how long you walk, how much you stand, affects the stress your kneecap experiences. Too much too soon and you inflame the tissue. Too little and the tissue never adapts.
The practical approach is simple. Track your pain on a zero to ten scale before and after activity. Aim to stay at a two or below during movement. If stairs cause a four, reduce the number of flights or the speed. Gradually increase exposure over days and weeks. A useful rule of thumb is to increase your daily stair load by no more than ten percent per week.
Your body adapts to load. It just needs time, consistency, and a pace it can handle.
Stepping Up to a Pain-Free Life
Knee pain on stairs is common. But “common” doesn’t mean you’re stuck with it.
The key insight from current research is this: the knee is often the victim, not the villain. The hip and core are where the real work needs to happen. Fix the mechanics above the knee, and the knee stops taking the hit.
Here’s the approach that the evidence supports, broken into three clear priorities.
Fix the mechanics. Femoral internal rotation is the main driver of kneecap stress on stairs. Hip strengthening directly corrects this pattern. Start with glute bridges and lateral band walks. Be consistent. Do them daily.
Strengthen both the hip and the knee. Don’t abandon quad work. The research from Crossley and Lack is clear: the combination outperforms either approach alone. Build a balanced program that targets glute strength, hip abduction, and quad control in equal measure.
Manage the load. Don’t rest completely, and don’t push through high pain. Find your threshold and stay just below it. Increase your activity gradually. Pacing is a skill, and it’s worth learning.
Start by testing your hip strength today. Can you do 20 glute bridges with both legs, then 10 single-leg glute bridges per side with your hips level throughout? Can you lateral band walk for 30 seconds in each direction without your knee caving inward?
If these feel hard or wobbly, you’ve found your starting point.
The stairs aren’t your enemy. They’re a test of whether your whole movement system is working together. Right now, it may not be. But with the right work in the right places, that changes.
Note: This article is for general educational purposes. If you have significant or persistent knee pain, consult a physiotherapist or sports medicine physician for an individualized assessment and treatment plan.



