Researchers found that a muscle that’s 1% of your body weight can double your metabolism while you sit. Most people over 50 have never used it correctly.
The standard story goes like this: you age, hormones shift, muscles shrink, and your body burns fewer calories. Eat less. Move more. Lift weights. It’s tired advice. And for a lot of people over 50, it just doesn’t work the way it used to. That’s not a personal failure. The biology has changed, and the advice hasn’t caught up.
There’s a specific physical state that most health content never talks about. It has nothing to do with how hard you train. It’s about what your body does during all the hours you spend completely still, and those hours are likely adding up to more metabolic harm than most people realize.
The “active couch potato” problem
You can work out four days a week and your body will still classify you as deeply inactive. That’s not a theory. It’s the conclusion of a growing body of research.
Scientists have identified a field called “inactivity physiology,” and it operates separately from exercise science. Exercise physiology studies what happens when you move. Inactivity physiology studies what happens when you don’t, and the two states don’t cancel each other out.
Research in Physiological Reviews confirms that prolonged sitting triggers harmful metabolic effects even in people who meet standard exercise guidelines. Sitting isn’t just the absence of movement. It’s a distinct biological state with its own consequences.
Think of it like a car. One that runs well for an hour a day but sits idle for 23 hours still develops rust. The driving doesn’t fix the problem. The stillness is the problem.
For someone over 50 who attends spin class three mornings a week but spends the rest of their time at a desk, this is not a minor point. The spin class is working. The desk is quietly undoing some of it in ways that don’t show up until blood sugar and triglycerides start climbing.
Why the usual advice stops working after 50
There’s a second problem layered on top of the sitting issue. It’s the reason so many people over 50 follow the classic prescription of “lift weights and eat more protein” and still feel like they’re fighting a losing battle.
Older muscle develops what scientists call “anabolic resistance.” In younger adults, protein and the strain of resistance training reliably trigger muscle repair and growth. After around 50, that response weakens. The muscle needs more protein to get the same signal. More stimulus to produce the same result. The workout that built muscle at 35 may barely maintain it at 55. This isn’t a discipline issue. It’s cellular.
Anabolic resistance drives sarcopenia, the steady loss of muscle mass that picks up speed after midlife and is one of the main engines behind a slowing metabolism. When people over 50 say their old methods have stopped working, they’re right. Their muscles have genuinely changed how they respond. That frustration is biologically valid.
The standard advice is not wrong. It’s just incomplete. It doesn’t account for changed muscle biology, and it says nothing at all about the damage sitting does between workouts.
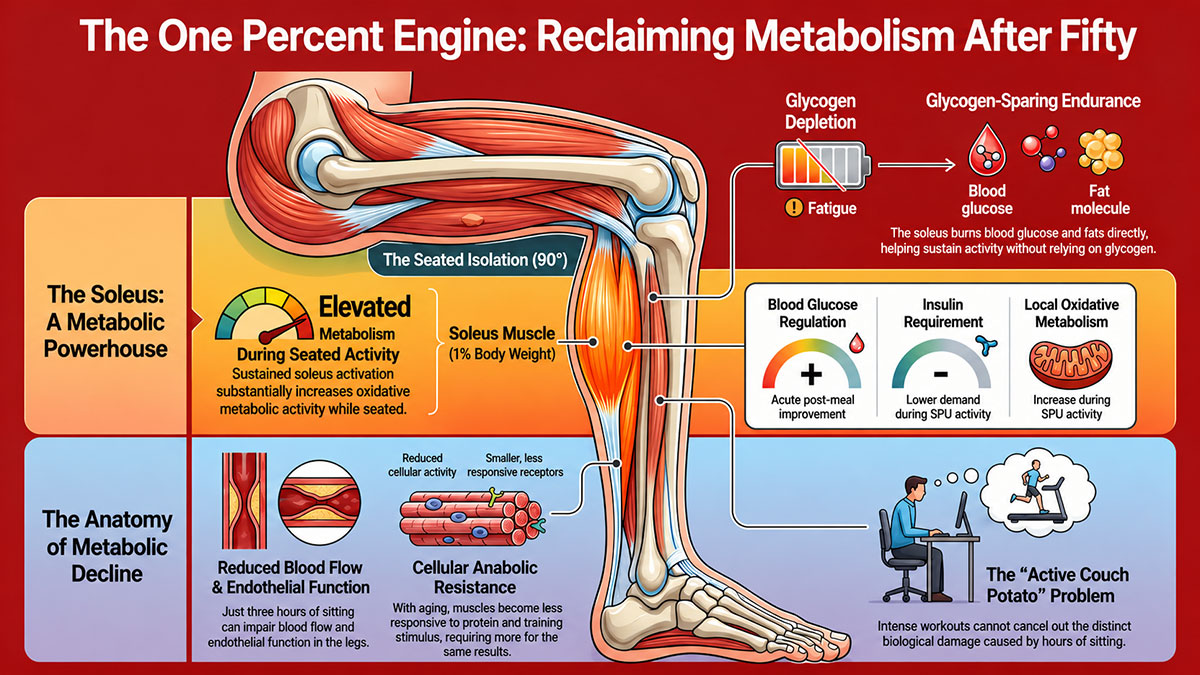
The one-percent engine
The soleus is a muscle almost nobody thinks about. It sits along the back of the lower leg, tucked beneath the gastrocnemius, and makes up about one percent of total body weight. Small. Overlooked. Left out of nearly every strength program ever written.
In 2022, University of Houston physiologist Dr. Marc Hamilton and colleagues published a study in the journal iScience that reframed what this small muscle can do. Their findings were built around a seated movement called the Soleus Pushup (SPU). The results stopped the research team in their tracks. Hamilton said his team was unaware of any drug that could produce a comparable effect.

The SPU roughly doubles whole-body resting metabolic rate while seated. The soleus raises its local oxidative metabolism two to three times above baseline and holds that level for hours, without tiring.
In a three-hour window after a meal, people who performed the SPU showed a 52% improvement in blood glucose regulation and needed 60% less insulin than those sitting still. The soleus does this by burning blood glucose and circulating fats rather than muscle glycogen. Glycogen depletion causes fatigue. This muscle sidesteps that process entirely.
A muscle at one percent of body weight doubles the metabolic output of the whole body. It’s a genuinely odd result.
Traditional training focuses on the large muscles: quads, glutes, back. It makes sense on paper. More mass, more metabolic impact. The SPU research suggests that logic misses something important about how the soleus works.
As the University of Houston press briefing on the research explained, the soleus is packed with slow-twitch, oxidative muscle fibers. These fibers run on oxygen and blood-borne fuel. They don’t tire easily. They’re built for endurance, not explosive power. That’s exactly why they’re useless to most gym programs and exactly why they’re so effective here. The soleus is already designed for sustained, low-level work. It just needs to be turned on.
Why it’s different from a calf raise
This is the part most people get wrong. A standard calf raise, standing, recruits the gastrocnemius first. That’s the large, visible muscle that makes up the rounded shape of the calf. It’s glycolytic. It fatigues. It’s not the target.
The SPU is performed seated, with knees bent at roughly 90 degrees. That position shortens the gastrocnemius. It takes that muscle largely out of the picture. What’s left is the soleus, working alone. That’s the whole point. The seated position isn’t a workaround or a modification for convenience. It’s what makes the exercise work at all.
Standing up and doing calf raises is fine exercise. It won’t produce the same metabolic result. The biology depends on isolating the oxidative soleus, and only the seated version does that reliably.
How to do it
Sit with your feet flat on the floor, hip-width apart, knees above your heels. Let your calf muscles fully relax. Then raise your heel off the floor while keeping the ball of your foot planted. Your calf contracts at the top. Lower your heel back down slowly. That’s one rep.
The pace should be controlled and deliberate. Not rushed. Not explosive. Think of it as a slow, continuous pump rather than a calf raise for reps. You should feel your calf working steadily, not burning out. You can do this while reading, in a meeting, or watching television.
Hamilton’s lab ran SPU sessions over multiple hours. That’s not a realistic daily target. The practical takeaway is regular activation throughout seated time, not a fixed number of minutes. Because the soleus doesn’t fatigue the way most muscles do, it handles repeated short sessions across the day without any real recovery cost.
What sitting does to your blood sugar and arteries
The SPU’s metabolic effect isn’t the whole story. Something else is happening in your blood vessels every hour you spend in a chair, and it runs in parallel to the blood sugar problem.
In a randomized crossover trial, Dunstan and colleagues (2012) published in Diabetes Care found that breaking up prolonged sitting with two-minute bouts of light walking every 20 minutes significantly reduced postprandial blood glucose and insulin levels in overweight and obese adults aged 45 to 65, compared to sitting without a break. The activity didn’t have to be intense. Just brief, consistent, and muscle-activating.

Thosar and colleagues, writing in Experimental Physiology, found that three hours of sitting was enough to significantly impair shear rate and endothelial function in the superficial femoral artery. Shear stress is the force that flowing blood exerts on artery walls. It keeps those walls flexible and signals the body to produce nitric oxide. When you sit, blood pools in the lower legs. Flow slows. Shear stress drops. Artery function starts to decline within hours. But when light activity breaks were introduced, the drop in endothelial function was prevented. The calf muscles, the soleus among them, are what keep that blood moving.
Sit still long enough and the damage is already building. Rising blood sugar. Stiffening arteries. A suppressed metabolism. None of it feels like anything in the moment.
The missing piece in the standard advice
The “eat less, move more, lift weights” framework isn’t wrong. It’s just missing something large.
It treats exercise as the primary variable and sitting as neutral. The research says sitting is not neutral. It’s an active metabolic suppressor with its own biology, separate from exercise. Addressing one without the other leaves a real gap.
Someone who adds three gym sessions a week but sits for nine hours a day is managing the edges of the problem. The gym session happens once. Sitting happens all day. The SPU doesn’t replace the gym. It fills the gap the gym can’t reach: the long sedentary stretch between sessions where metabolic damage actually builds.
The hours you spend sitting are not neutral time. Full stop. Blood sugar, insulin response, arterial health, metabolic rate: all of it is actively shaped by stillness. A slow, repetitive movement in the back of your calf, done in your chair, with no equipment, has measurable effects on every single one of those things.
One final thought
The fitness industry has spent decades focused on what happens during the workout. The more interesting question, it turns out, is what happens during everything else. A muscle that weighs next to nothing, buried under the more impressive calf muscle most people can name, has been quietly capable of changing whole-body metabolism all along. Nobody thought to ask the right question until now.



