Your blood work looks fine. Your doctor says you’re healthy. So why does your brain feel like it’s wrapped in wet cotton?
You’re not imagining it. That thick, foggy feeling in your head, the one where words slip away mid-sentence, where you read the same paragraph three times without retaining a single word, it’s real. It has a name: brain fog.
But here’s what’s frustrating. You go to the doctor. You describe it. You get a blood panel. Everything comes back “normal.” You leave with a pamphlet suggesting you sleep more and reduce stress.
Nothing changes.
This happens more often than it should. Standard medical check-ups aren’t designed to catch the subtle, slow-burning problems that quietly rob your mind of its sharpness. The causes are often hiding in plain sight, or buried deep inside systems your doctor may not even test during a routine visit.
This article breaks down nine scientifically supported triggers of brain fog that are frequently overlooked. These aren’t fringe theories. They’re backed by peer-reviewed research, and understanding them may finally give you the answers you’ve been searching for.
Cause 1: Subclinical Hypothyroidism (The “Normal” Range Illusion)
Your thyroid does a lot more than most people realize. It produces hormones that regulate nearly every cell in your body, including every neuron in your brain. When thyroid output drops even slightly below what your brain needs, you feel it.
The tricky part? “Normal” is a wide range.
Standard thyroid tests (TSH levels) flag a problem only when the numbers fall outside a broad window. But research by Bono and colleagues, published in the Journal of Clinical Endocrinology & Metabolism in 2004, found that even mild thyroid dysfunction below clinical thresholds was tied to cognitive slowing, memory complaints, and subjective brain fog. In other words, your results can look fine on paper while your brain is quietly struggling.
This is sometimes called subclinical hypothyroidism. “Subclinical” means the dysfunction is real, but not severe enough to trigger a clinical diagnosis using standard cut-offs.
If your brain fog is paired with fatigue, feeling cold, dry skin, or weight changes, it’s worth asking your doctor about a full thyroid panel. This goes beyond basic TSH and includes free T3, free T4, and thyroid antibodies. A standard TSH test alone doesn’t always tell the full story.
Cause 2: Ultra-Processed Diets (The Cognitive Cost of Convenience)
Food shapes the brain more directly than most people appreciate.
A landmark study by Felice Jacka and colleagues, published in 2010, followed a large group of Australian adults and found a clear pattern. Those who ate Western-style diets high in processed foods had worse cognitive function and a higher risk of depression. People who ate whole-food diets rich in vegetables, fruits, lean proteins, and healthy fats showed protective effects on brain health.
The mechanism isn’t mysterious. Ultra-processed foods are low in the nutrients your brain depends on: B vitamins, omega-3 fatty acids, antioxidants, and minerals like magnesium and zinc. They also tend to spike blood sugar sharply, followed by a crash that leaves you sluggish and unfocused.
Your brain is about 2% of your body weight but uses roughly 20% of its energy. Feed it junk, and it performs like a high-performance car running on low-grade fuel.
This isn’t about perfect eating. It’s about recognizing that convenience foods come at a cognitive cost, one that builds up over time without obvious symptoms until brain fog becomes your daily baseline.
Cause 3: Chronic Low-Grade Inflammation (A Smoldering Fire in Your Brain)
Inflammation has a well-known role in physical conditions like arthritis and heart disease. Its role in brain function is less commonly discussed, but the science is just as compelling.
In a detailed clinical review, Michael Maes and colleagues examined the link between inflammatory markers, fatigue, and cognitive symptoms. Their 2009 findings, published in Neuropharmacology, showed that elevated levels of cytokines such as IL-6, TNF-alpha, and CRP were directly tied to slowed psychomotor speed, fatigue, and cognitive complaints that look exactly like brain fog.

Here’s the key problem: this kind of inflammation doesn’t hurt. It doesn’t cause a fever. It doesn’t make you feel obviously sick. It just quietly interferes with brain function in the background.
Common drivers of low-grade inflammation include poor sleep, a diet high in processed foods, excess body fat around the abdomen, chronic stress, and gut imbalances. Many people carrying this kind of inflammation would have no idea from their last basic check-up because CRP and other inflammatory markers aren’t part of a standard blood panel.
Ask your doctor about testing for high-sensitivity CRP (hs-CRP) and other inflammatory markers if brain fog is a persistent issue for you.
Cause 4: Gut Microbiome Dysbiosis (When Your Second Brain Goes Wrong)
There’s a two-way communication highway between your gut and your brain. It’s called the gut-brain axis, and it’s far more involved in cognitive function than scientists once thought.
Your gut is home to trillions of bacteria, fungi, and other microorganisms that collectively make up your microbiome. These organisms produce neurotransmitters like serotonin and GABA, help regulate inflammation, and send signals directly to the brain via the vagus nerve.
A major review by John Cryan and colleagues, published in Nature Reviews Neuroscience in 2019, laid out the evidence for how gut bacteria influence brain function, mood, and cognition. When the microbiome gets out of balance, a state called dysbiosis, the resulting disruption to neurotransmitter production and inflammation pathways can show up as mood problems, poor focus, and cognitive impairment.
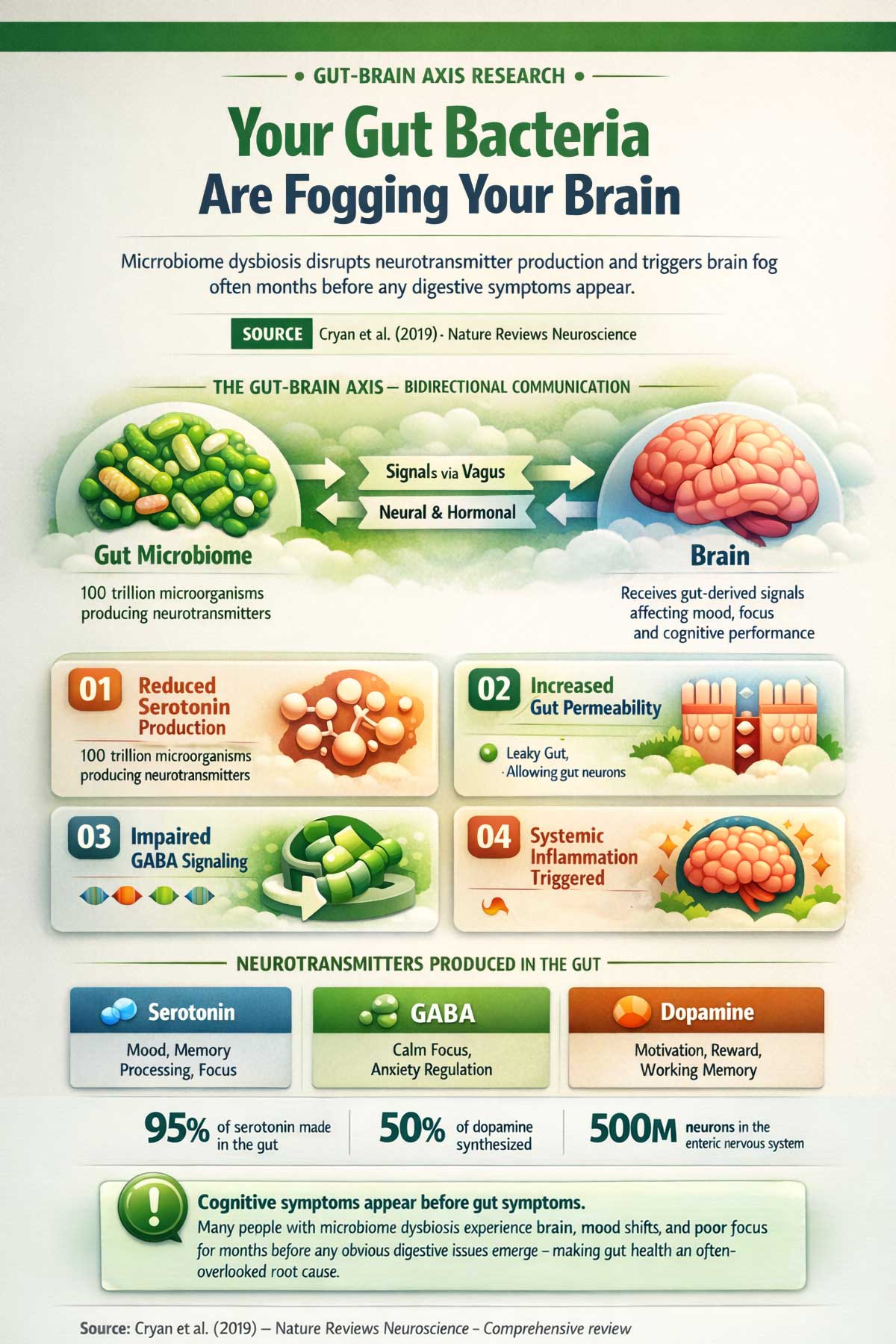
What makes this a hidden cause is timing. Cognitive symptoms from dysbiosis can appear long before any obvious digestive problems show up. Someone might have significant gut imbalances and feel mentally cloudy for months before they ever notice bloating or bowel changes.
The microbiome is heavily influenced by diet, antibiotic use, sleep quality, and stress. A diet rich in fiber and fermented foods supports a healthier microbial balance. Testing options like comprehensive stool analysis are available through functional medicine providers and can provide a clearer picture of gut health.
Cause 5: Sleep Fragmentation (Exhausted Even After 8 Hours)
Most people focus on how many hours they sleep. But the quality of those hours matters just as much, if not more.
Sleep fragmentation refers to repeated disruptions throughout the night. These are micro-awakenings, brief interruptions to sleep that the sleeper rarely remembers. You might spend eight hours in bed and still wake up unrefreshed, mentally slow, and unable to concentrate, because your brain never moved through the deeper stages of sleep it needed.
Kristine Yaffe and colleagues published findings in 2014 in the journal Neurology from a longitudinal study of older women. Objectively measured sleep fragmentation was strongly linked to impaired attention, poor memory consolidation, and accelerated cognitive decline over time. The researchers used actigraphy (wrist-worn sensors) to measure sleep objectively, not just what participants reported.

This matters because standard sleep questions in a medical visit rely on self-report. Patients say they “sleep fine” because they don’t remember the interruptions. Meanwhile, their brain is being starved of the restorative deep sleep cycles required for memory processing and cognitive repair.
Common causes of sleep fragmentation include sleep apnea, restless leg syndrome, chronic pain, anxiety, and alcohol use (which fragments sleep in the second half of the night). If you consistently wake up feeling unrefreshed, a sleep study is worth considering.
Cause 6: Vitamin B12 Deficiency (The Underdiagnosed Early Stage)
B12 is essential for the health of your nervous system. It plays a role in producing myelin, the protective coating around nerve fibers, and in synthesizing the neurotransmitters your brain uses to communicate.
A deficiency in B12 can produce neurological and cognitive symptoms well before a standard blood count shows anything abnormal. Stabler and Allen, in their widely cited 2004 review in the Annual Review of Medicine, described how early-stage B12 depletion can cause confusion, memory disturbance, and cognitive slowing, and that this is often missed because standard panels measure total B12 rather than the more sensitive markers of deficiency.
A better test is methylmalonic acid (MMA) and homocysteine levels. These are metabolic markers that rise before B12 levels in a standard blood test drop to the deficient range. Your blood count can look normal while your neurons are already being affected.
Groups at higher risk include older adults (because absorption decreases with age), vegetarians and vegans (animal products are the primary dietary source), people taking metformin for diabetes, and those who regularly use proton pump inhibitors for acid reflux, which interfere with B12 absorption.
This is one of the more treatable causes of brain fog. If you fall into a risk group, it’s worth asking specifically about MMA and homocysteine testing rather than a standard B12 check.
Cause 7: Immune Activation and “Sickness Behavior” (When Your Body Fogs Your Mind on Purpose)
Here’s a biological twist that surprises most people: brain fog can be an intentional product of your immune system.
When your body detects a threat, whether it’s an infection, an injury, or even chronic low-level stress, it releases proteins called cytokines. These cytokines travel to the brain and trigger a state called “sickness behavior.” You feel tired, unmotivated, mentally foggy, and socially withdrawn. This is your immune system forcing your body to rest and conserve energy for healing.
Robert Dantzer and colleagues described this mechanism in a foundational 2008 paper in Nature Reviews Neuroscience. They showed how cytokine-mediated immune activation produces this exact cluster of symptoms. Under normal circumstances, the state resolves when the threat passes.
The problem is that for many people, this pathway stays chronically activated without an obvious acute illness. Persistent low-grade infections, autoimmune conditions, gut dysbiosis, or even ongoing psychological stress can keep cytokine levels just high enough to maintain a low-level sickness behavior state. The result is a kind of permanent cognitive tax.
This is one reason why brain fog is reported across such a wide range of conditions, from autoimmune disorders to chronic fatigue syndrome to post-viral illness. The immune system is running a program that was designed to be temporary, but it never received the signal to stop.
Cause 8: Chronic Cortisol Overload (Stress That Physically Changes the Brain)
Stress is bad for the brain. You’ve heard that. But “reduce your stress” as medical advice is close to useless without understanding what stress is actually doing to your brain on a structural level.
Cortisol is the body’s primary stress hormone. In short bursts, it’s useful. It sharpens attention and mobilizes energy. But when cortisol stays elevated for weeks or months, it starts damaging the very brain structures responsible for memory and clear thinking.
Bruce McEwen and colleagues published research in 2007 showing that prolonged exposure to stress hormones physically impairs the hippocampus and the prefrontal cortex. The hippocampus is your brain’s memory hub. The prefrontal cortex handles focus, judgment, planning, and impulse control. When chronic stress degrades these areas, the effects are measurable: poorer memory, reduced concentration, difficulty making decisions, and emotional dysregulation.

This is not abstract. It’s structural. The good news is that the brain shows significant capacity for recovery when the stress load is reduced and supportive habits are put in place. Sleep, exercise, and mindfulness practices all show measurable effects on cortisol regulation and hippocampal health in the research literature.
The issue is that many people are living under a chronic stress load that they’ve normalized over years, so it no longer feels like “stress.” It’s just how life feels. But if that’s where you are, your brain is still paying the biological cost.
Cause 9: Long COVID Neurological Effects (The Post-Viral Brain)
Before 2020, post-viral cognitive symptoms were underappreciated outside of specialists treating conditions like post-Lyme syndrome or chronic fatigue syndrome. That changed dramatically when brain fog became one of the most widely reported symptoms of Long COVID.
Ziyad Al-Aly and colleagues published a landmark study in Nature Medicine in 2022, analyzing data from hundreds of thousands of COVID-19 survivors. They found that post-COVID patients showed significantly higher rates of persistent cognitive impairment, memory problems, and subjective brain fog compared to control groups, even months after the initial infection had resolved.
The mechanisms appear to involve neuroinflammation, micro-clotting in brain vasculature, disruptions to the blood-brain barrier, and reactivation of latent viruses like Epstein-Barr. In some patients, these effects are linked to the severity of the initial infection. In others, they occur after cases that were mild by standard measures.
What makes this relevant beyond COVID specifically is the broader lesson: viral infections can leave a neuro-inflammatory footprint long after the acute illness is gone. This isn’t a new phenomenon. It’s just one that has received much wider attention and research funding since 2020.
If your brain fog started or worsened following any viral illness, including flu, COVID-19, or a non-specific illness, this pathway deserves consideration. Post-viral specialists and clinics are increasingly available for evaluation and targeted support.
What to Do Next: A Practical Playbook for Your Doctor’s Visit
Brain fog is not a diagnosis. It’s a symptom, and symptoms have causes. The goal is to find yours.
Here’s a checklist of specific tests and topics worth discussing with your healthcare provider. Not all of these will be appropriate for every person, but this list gives you a starting point for a more informed conversation.
Thyroid: Request a full thyroid panel including TSH, free T3, free T4, and thyroid antibodies (TPO and TG antibodies), not just TSH alone.
Inflammation: Ask about high-sensitivity CRP (hs-CRP), IL-6, ESR (erythrocyte sedimentation rate), and if relevant, ANA (antinuclear antibodies) to screen for autoimmune activity.
Nutritional status: Beyond standard B12, ask about methylmalonic acid (MMA), homocysteine, vitamin D, magnesium (RBC magnesium, not serum), zinc, and ferritin.
Sleep: If you suspect fragmented sleep or snoring, ask for a referral for polysomnography (a formal sleep study) or a home sleep apnea test.
Gut health: A comprehensive stool analysis through a functional medicine provider can assess microbiome diversity, markers of dysbiosis, and intestinal permeability.
Stress markers: Ask your provider about salivary cortisol testing across the day (diurnal cortisol) to assess HPA axis function if chronic stress is a concern.
Post-viral workup: If symptoms began or worsened after an infection, mention this explicitly. Ask about referral to a Long COVID clinic or a provider familiar with post-viral syndromes.
Brain fog doesn’t have to be your normal. The nine causes covered here are each real, each measurable in some form, and each treatable once identified. Stop accepting a shrug as an answer. The right tests and the right questions can change everything.



