Millions are told their knee pain is arthritis and aging. The research says something else is usually driving it—and it’s fixable.
You’ve probably had the conversation. The doctor pulls up an X-ray, points to some shadowy patches, and says something like, “There’s quite a bit of wear here.” You leave with a diagnosis—arthritis, cartilage thinning, bone-on-bone—and the quiet sense that your knees are simply done.
But here’s what most people are never told: that X-ray is only part of the story. And it may not even be the most important part.
The Great X-Ray Deception: Why Your Scans Don’t Tell the Whole Story
This might sound strange. So let’s start with a real paradox.
Some people walk around with X-rays that look like a car crash. Bone spurs. Cartilage loss. Classic “severe arthritis.” And yet—they run. They hike. They feel fine. Others have scans that look nearly perfect, and they can barely get down the stairs.
This isn’t a medical mystery. It’s actually well-documented. A review by Dr. Tuhina Neogi published in Osteoarthritis and Cartilage (2013) laid it out clearly: the link between radiographic damage and how much pain a person feels is poor. Pain is shaped by many factors—muscle strength, nerve sensitivity, and even mental and emotional health. A scan shows structure. It doesn’t measure suffering.
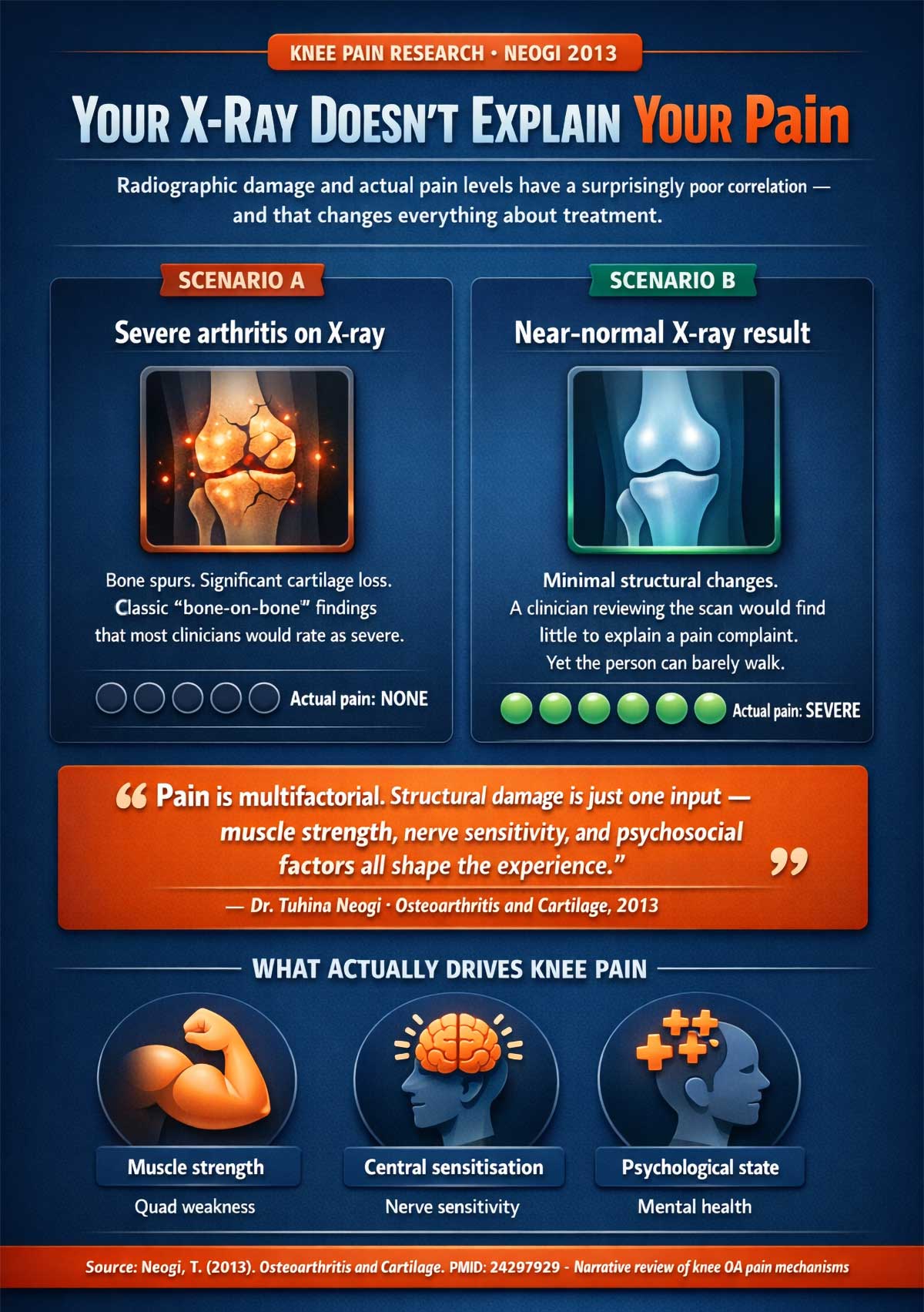
This single fact changes everything.
If structural damage doesn’t reliably predict pain, then chasing structural damage as the only explanation may be leaving you without real answers—and without a real path forward.
The Hidden Culprit: It’s Not the Joint, It’s the “Engine”
Think about the shock absorbers in a car. When they’re working well, the bumps in the road barely register. The chassis—the frame of the car—is protected. But when the shocks fail, every pothole rattles the entire structure. The chassis takes punishment it was never designed to absorb.
Your quadriceps—the muscles at the front of your thigh—work exactly like those shock absorbers. They’re the primary force-absorbers for the knee joint. When they’re strong, they take the load. When they’re weak, the joint itself takes the hit, every single step.
A major long-term study by Dr. Neil Segal and colleagues, published in Radiology (2010), tracked over 3,000 adults between the ages of 50 and 79 who did not have symptomatic knee arthritis at the start. The researchers found that people with greater quadriceps strength at baseline were significantly less likely to develop symptomatic knee pain over the following 30 months. Critically, strength didn’t prevent structural changes from appearing on X-rays—but it did protect against those changes becoming painful. That’s the key distinction. Structure and symptoms are not the same thing. You can have worn cartilage and no pain, provided the muscles doing the load-bearing work are strong enough.

The flip side is equally important. Weakness leads to a cycle that’s hard to break out of without the right approach. Pain causes people to move less. Moving less causes muscles to weaken. Weaker muscles put more pressure on the joint. More pressure means more pain. The cycle feeds itself quietly over months and years.
Why “Just Rest” Can Make Things Worse
For decades, rest was the go-to advice for sore knees. If it hurts, stop. Give it time. But this advice, well-intentioned as it is, can backfire badly in the long run.
Prolonged inactivity leads to muscle wasting. Less muscle means less shock absorption. Less shock absorption means more joint stress when you finally do move. What starts as temporary relief can harden into a long-term problem.
A major meta-analysis published in the Cochrane Database (2015) by Dr. Marlene Fransen and colleagues reviewed 44 clinical trials involving over 3,500 adults with knee arthritis. Land-based exercise produced meaningful reductions in pain and improvements in physical function. The effect sizes were comparable to those seen with anti-inflammatory medications—but without the stomach and cardiovascular side effects that come with long-term NSAID use.
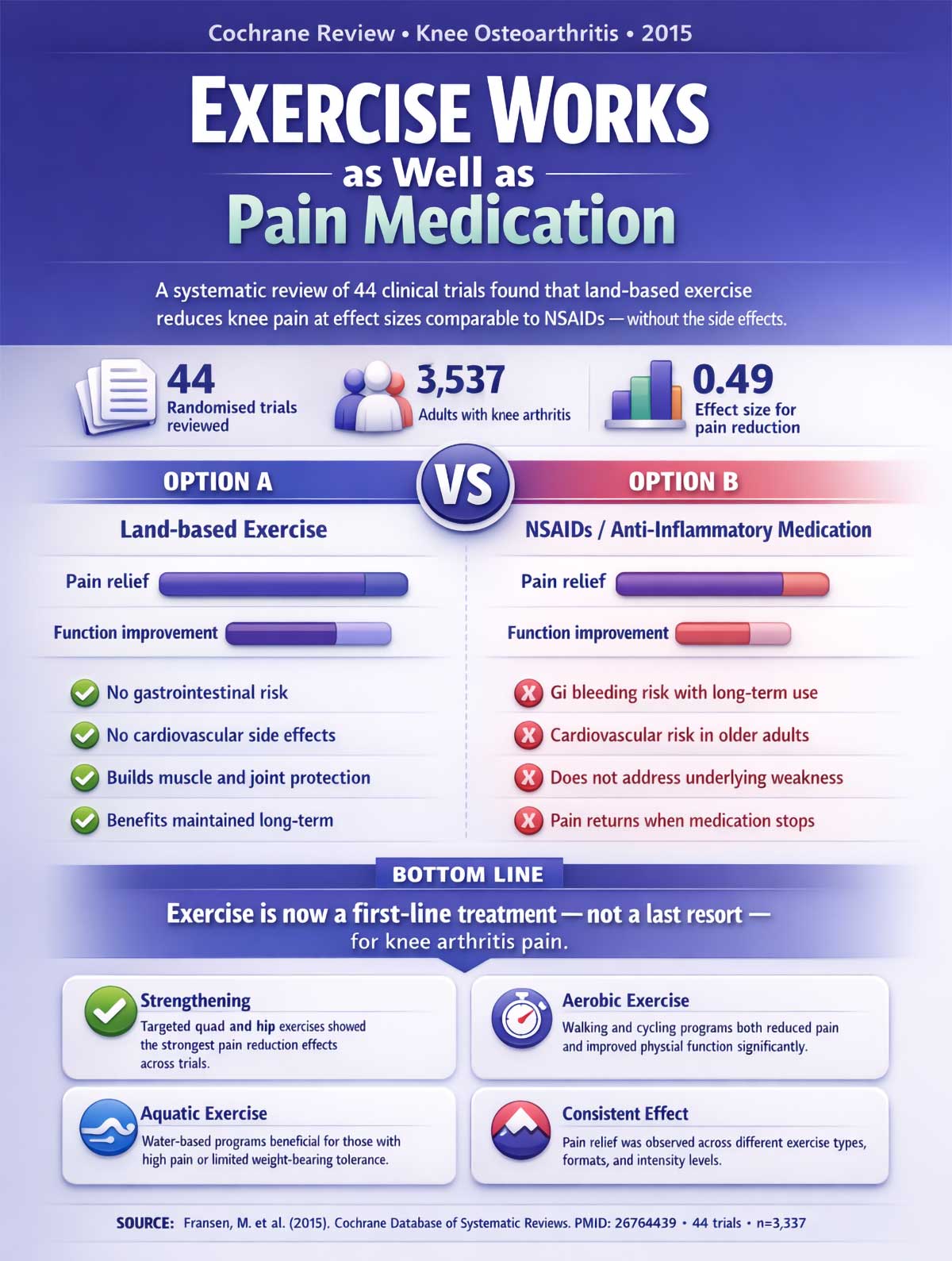

The takeaway isn’t that pain should be pushed through recklessly. It’s that movement, done right, is medicine. Sitting still for too long is often the worse choice.
The Brain-to-Muscle Disconnect: Why the “Engine” Sometimes Won’t Start
Here’s something almost nobody talks about: your brain may be actively switching off your quadriceps.
It’s called arthrogenic muscle inhibition. When a joint is injured, swollen, or under stress, the nervous system responds by dialing down activity in the surrounding muscles. The intent is protective—reducing force around a painful joint. But the result is weakness, even in people who are otherwise trying to stay active.
Research has consistently shown that arthrogenic muscle inhibition affects the vast majority of people with knee pain or arthritis. Dr. Riann Palmieri-Smith’s work has demonstrated that this inhibition persists even in people who remain physically active, meaning the quadriceps simply won’t fire at full capacity despite the person’s best efforts. You’re moving, but the engine isn’t fully engaged.
This is why simply “walking more” often isn’t enough to fix the problem. If the quads aren’t activating correctly, you’re loading a poorly supported joint. The movement isn’t building the strength it should. Targeted exercises—specifically designed to re-engage these muscles—are essential before progressing to heavier training.
The “Victim” Joint: Why Your Hips and Ankles Are Part of the Problem
Your knee doesn’t work in isolation. It’s sandwiched between the hip above it and the ankle below it. When either of those joints isn’t doing its job, the knee compensates. And compensation, over time, equals pain.
This concept is called the kinetic chain. Your body moves as a connected system. A breakdown anywhere in the chain creates stress at the weakest link—and for most people, that weak link is the knee.
The hip connection
The gluteus medius is a muscle on the outer part of your hip. Its job is to keep your pelvis stable when you take a step. When it’s weak, the hip drops on the swinging side, which causes the knee to cave inward. This inward collapse increases the load on the inner knee and the kneecap joint. Every step becomes a small insult to the joint.
A systematic review by Dr. Kay Crossley and colleagues, published in the British Journal of Sports Medicine (2016), confirmed that hip muscle weakness—particularly the gluteus medius—alters lower limb mechanics and increases stress on the knee. Strengthening the hip reduced knee pain significantly.
The ankle connection
Stiff ankles are an underappreciated contributor to knee trouble. The ankle needs to move freely—especially rotating inward as you walk or squat. When it can’t, the knee has to pick up the slack. It starts rotating and bending in ways it wasn’t built to, accelerating wear on the cartilage and stressing the supporting ligaments.
Research by Dr. Thomas Andriacchi and colleagues, published in Annals of Biomedical Engineering (2006), showed that altered movement patterns—specifically how the knee loads and rotates during walking—directly accelerate cartilage breakdown. The way you move matters, not just how much you move.
The Movement Prescription: 4 Steps to Rebuild Your Knees
This isn’t about running a marathon or getting back into the gym five days a week. It’s about restoring the function that protects your joint, step by step.
Step 1: Wake Up the Quadriceps
Before you can strengthen the quads, you need to get them firing again. Isometric exercises are the starting point. These involve contracting the muscle without moving the joint—so there’s no aggravation, no impact, no pain.
A simple quad set involves sitting with your leg straight, pressing the back of your knee gently into the floor, and holding for five to ten seconds. This might feel too easy. That’s fine. The goal at this stage isn’t effort—it’s neuromuscular reconnection. Think of it as sending a signal to a muscle that’s been on standby.
Dr. Kim Bennell and colleagues have published several high-quality clinical trials showing that structured neuromuscular exercise programs for adults with knee arthritis lead to meaningful reductions in pain and improvements in function—with changes large enough to be considered clinically significant. The emphasis on neuromuscular retraining, not just general exercise, was key.
Step 2: Strengthen the Hip
Once the quads are activating more reliably, it’s time to address the hip. Side-lying leg raises, clamshells, and resistance band walks target the gluteus medius directly. None of these exercises require standing or putting load through the knee. They’re accessible, and they work.
Clinical trials led by researchers like Dr. Michael Rathleff have found that programs built around hip strengthening can outperform knee-only exercise plans, especially for kneecap-related pain. The mechanism is straightforward—a stable hip reduces the sideways forces that drive the knee inward with each step.
Even five to ten minutes of daily hip work can shift the mechanical forces acting on your knee. The effect builds over weeks. It’s not exciting, but it’s reliable.
Step 3: Manage Your Load Wisely
One of the most useful ideas in modern physical therapy is the concept of “optimal loading.” The idea is simple: tissue heals and strengthens when it’s exposed to the right amount of stress—not too much, not too little.
Complete rest leads to tissue weakening. Excessive loading leads to flare-ups. The goal is to find the window in between. That might mean walking 15 minutes instead of sitting all day, or adding light resistance rather than heavy weights. It means listening to how the knee responds in the 24 hours after activity, and adjusting accordingly.
A systematic review by Dr. Bjørnar Øiestad and colleagues, published in Osteoarthritis and Cartilage (2015), confirmed that quadriceps weakness is a risk factor not just for pain, but for the progression of knee arthritis over time. This means that building strength isn’t just about feeling better now—it’s about protecting the joint for the long term.
Step 4: Show Up Every Day
One hour at the gym once a week is far less effective than ten minutes of targeted movement every single day. Muscles respond to frequency. The nervous system adapts through repetition. Daily activation, even brief, sends a consistent signal to the muscles that they’re needed.
Consistency also prevents the cycle of deconditioning. Each day without movement is a small step backward. Each day with even modest activity is a small step forward. Over months, that difference compounds significantly.
Research by Dr. Adam Culvenor and colleagues, published in the British Journal of Sports Medicine (2017), found that quadriceps strengthening programs reduced pain and improved function—and importantly, those benefits were maintained six to twelve months after the intervention ended. That’s not just short-term relief. That’s lasting change built through consistent effort.
Rethinking the “Inevitable”
There’s a narrative that many people absorb over time. It goes something like this: knees wear out as you age. It’s just part of getting older. You have to manage it.
This narrative isn’t entirely wrong, but it’s dangerously incomplete. It frames the knee as a mechanical hinge—like a door hinge that eventually rusts. But a door hinge doesn’t heal. A knee does.
Biological tissue adapts. Cartilage health can be maintained or degraded depending on how the joint is loaded—and while cartilage itself has limited self-repair capacity in adults, the surrounding tissues respond continuously to use. Muscles grow or atrophy. Bone density rises or falls. Tendons strengthen or weaken. The human body is not static machinery. It responds to input.
Replacing “wear and tear” with “wear and repair” isn’t just motivational language. It reflects the actual biology. Given the right stimulus—progressive loading, consistent movement, proper mechanics—the body improves. At any age.
The American College of Rheumatology guidelines (Kolasinski et al., 2020) now give a strong recommendation for exercise—including strengthening, aerobic, and water-based training—as a first-line treatment for knee arthritis. Not a second option after medications. Not a “nice to have.” First line. That’s where the evidence has landed.
“But I’ve Tried Exercise Before…”
This is one of the most common responses—and it’s fair. Many people have genuinely tried exercise for knee pain and felt no real improvement. That’s not a sign that exercise doesn’t work. It’s usually a sign that the approach was missing something.
The most common gaps are these: arthrogenic muscle inhibition wasn’t addressed before loading started, the wrong muscles were targeted, or the progression moved too fast and kept flaring the joint. Generic “leg strengthening”—like pushing heavy weight on a leg press machine—isn’t the same as neuromuscular retraining that specifically wakes up inhibited quadriceps. In fact, loading a muscle that’s neurologically switched off can shift the work to compensating muscles, making the pattern worse.
The sequence matters just as much as the exercises themselves. Activation comes before loading. Hips get attention alongside the quads. Ankle mobility is part of the picture. When all of those pieces are in place, exercise works reliably—because the research behind it is robust.
When Strengthening Isn’t Enough
This article is not an argument against medical care. It’s an argument for a more complete picture.
Strengthening addresses the most common and modifiable drivers of knee pain. But there are situations where medical input becomes more important. If you experience a sudden, sharp increase in pain with significant swelling, a feeling that the knee is locking or giving way, or pain at night that disrupts sleep consistently—those are signals worth investigating with a doctor.
Similarly, if you follow a properly structured, well-progressed strengthening program consistently for eight to twelve weeks and see no improvement at all, that’s also a reason to get a more thorough assessment. For most people with gradual-onset knee pain driven by muscle weakness and poor joint mechanics, exercise is highly effective. But “most people” isn’t “everyone.” Know when to escalate.
What to Expect: A Realistic Timeline
Rebuilding strength around a painful joint takes time. Here’s a rough guide to what the process typically looks like:
Weeks 1–2: You’ll likely feel more body awareness around the knee. Muscle activation may feel unfamiliar. Pain levels may not shift much yet—and that’s normal.
Weeks 3–4: Daily activities start to feel slightly easier. Stairs may feel less difficult. The first signs of progress often show up in function before they show up in pain scores.
Weeks 8–12: Meaningful, stable improvements in both pain and strength. This is when most people feel confident that something real is changing.
Months 4–6: Gains consolidate. The new movement patterns start to feel automatic. Maintenance becomes easier than building.
Progress is rarely linear. Some weeks feel like a step back. That’s normal in any rehabilitation process. The overall direction—measured across weeks, not days—is what matters.
A Quick Self-Assessment: Two Tests You Can Do Right Now
You don’t need a clinic to get a rough sense of whether muscle weakness is contributing to your knee pain. These two simple tests are used by physical therapists as quick functional screens.
The Chair-Stand Test
Sit in an upright chair with your arms crossed over your chest. Without using your hands for support, stand up fully and sit back down. Try to complete as many repetitions as you can in 30 seconds.
For adults aged 60 to 64, a rough benchmark is 14 to 17 repetitions for women and 14 to 19 for men. If you fall well below this range—or find yourself relying heavily on your arms—quadriceps weakness is likely a significant factor in your knee pain. The test isn’t diagnostic, but it gives you a starting point.
The Single-Leg Balance Check
Stand near a wall or counter in case you need support. Lift one foot off the floor and see how long you can hold the position with your eyes open. Then try it with your eyes closed.
Most healthy adults can hold a single-leg balance for 30 seconds or more with eyes open. Struggling to hold ten seconds, or noticing that your knee wobbles and caves inward, points to neuromuscular control deficits. This is the “firing” problem in action—not the strength itself, but the coordination and timing of the muscles around the joint.
If either of these tests highlights a weakness, that’s actually useful information. It means there’s something concrete to work on. Something that can change.
Your Knee Is Not a Car Part
This is the hardest shift to make—but also the most important one.
A worn-out car part gets replaced. It doesn’t grow back stronger. Your knee is not a car part.
It’s living tissue surrounded by muscles, tendons, and nerves that all communicate, adapt, and respond. When the supporting system is strong, even a structurally imperfect joint can function well and feel fine. When the supporting system breaks down, even a “normal” joint can cause significant pain.
The X-ray tells you about structure. It doesn’t tell you about what the muscles are doing, whether the hips are stable, whether the brain is activating the quads properly, or whether movement has become so restricted that the whole system is stiffening up around the joint.
Most patients get a scan. What they actually need is a strength assessment.
The good news is this: muscle weakness is modifiable. Neuromuscular dysfunction can be retrained. Hip stability can be rebuilt. Stiff ankles can be improved with consistent work. None of this requires surgery. None of it requires strong medications. It requires consistent, targeted effort—and the understanding that your knee has not given up on you, even if the X-ray makes it look that way.



