It went head-to-head with a prescription ACE inhibitor. The results surprised researchers — and most doctors still aren’t talking about it.
There’s a deep-red tea that’s been used for centuries across West Africa, Latin America, and Southeast Asia. People drank it for its tart flavor and cooling effect. Today, scientists are taking a much closer look at what it does to blood pressure — and the results are hard to ignore.
Hibiscus tea, made from the dried calyces of Hibiscus sabdariffa, is now one of the most studied herbal teas in heart health research. It’s not a miracle cure. But for people managing mild to moderate high blood pressure, the science behind it is genuinely worth knowing.
What 26 Clinical Trials Actually Found
Most articles about hibiscus tea cite one or two older studies and call it a day. This one won’t.
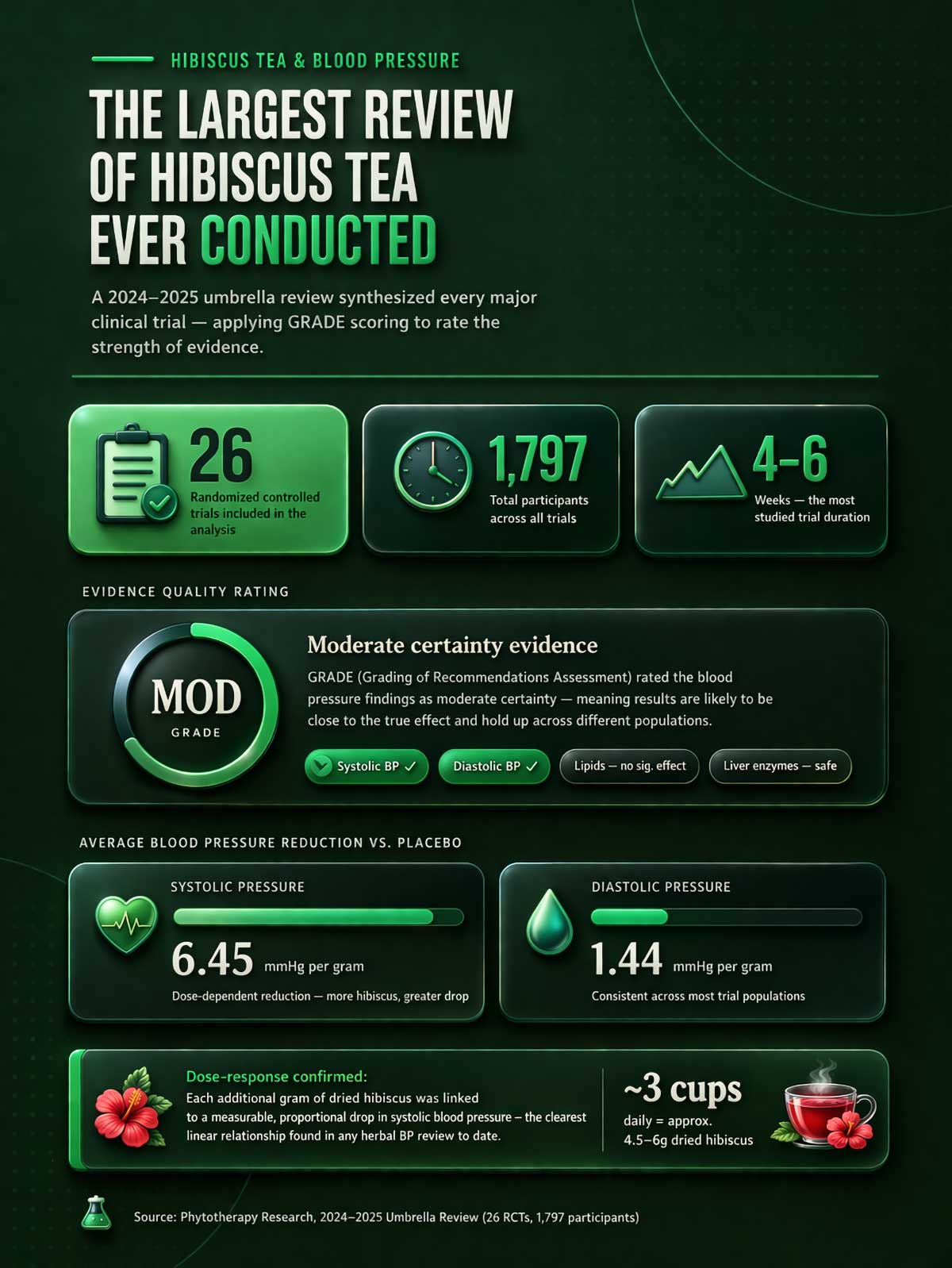
A 2024–2025 umbrella review published in Phytotherapy Research pulled together data from 26 randomized controlled trials, covering 1,797 participants. That’s the largest and most thorough analysis of hibiscus and blood pressure to date. The researchers used GRADE certainty scoring — a rigorous system for rating evidence quality.
The conclusion? Hibiscus tea produces a real, measurable reduction in both systolic and diastolic blood pressure compared to placebo. The certainty of evidence was rated as moderate — meaning it holds up under scrutiny, not just in one population or one lab.
This is the kind of data that changes how we think about a plant-based remedy.
The Dose-Response Link: Why Every Gram Counts
One of the most useful findings from the umbrella review is what researchers call a dose-response relationship. This means the more hibiscus you consume (within reason), the greater the drop in blood pressure.
Specifically, each gram of hibiscus corresponded to an average systolic blood pressure reduction of 6.45 mmHg. Diastolic blood pressure dropped by an average of 1.44 mmHg per gram.
That’s a meaningful number. For context, a 5 mmHg drop in systolic blood pressure is associated with a significantly reduced risk of stroke and heart disease in long-term studies. The reductions seen in hibiscus trials — averaging 6–7 mmHg, and reaching 10+ mmHg in people starting with higher readings — place the herb in the range of clinically meaningful benefit, comparable to modest blood pressure medication.
Most of the trials in the review used between 2g and 10g of dried hibiscus daily. The most commonly studied dose — and the most practical for everyday use — translates to about three 8-ounce cups of hibiscus tea per day. That’s the amount used in many of the positive trials, including one widely referenced study from 2010.
Why 6 Weeks Is the Sweet Spot
Researchers at Tufts University conducted a rigorous randomized controlled trial in 2010, published in the Journal of Nutrition. Sixty-five adults with pre-hypertension or mild hypertension — none of them on blood pressure medication — drank three 240mL servings of hibiscus tea daily for six weeks.
The result: their systolic blood pressure dropped by 7.2 mmHg compared to just 1.3 mmHg in the placebo group. That difference was statistically significant. People who started the trial with higher baseline readings saw even greater reductions. It’s worth noting that individual responses varied widely — some participants saw much larger drops, others smaller ones. The trend strongly favored hibiscus, but the variation reflects real biological differences between people.

Six weeks is the window that appears most consistently in the positive trials. It’s long enough for the active compounds in hibiscus to produce measurable vascular changes. It’s short enough to be a realistic commitment. Think of it as a loading period — the first two weeks you’re building up consistent levels of anthocyanins in your system. By weeks five and six, the effects tend to peak.
The Compound Doing the Heavy Lifting
The deep crimson color of hibiscus tea isn’t just beautiful — it’s a sign of the compounds responsible for most of its effects. Anthocyanins, the pigments that give hibiscus calyces their rich red hue, are the primary active compounds identified in the research.
These molecules work through several established pathways. They reduce oxidative stress in blood vessel walls, improving vascular function and flexibility. They also produce a mild diuretic effect and appear to reduce sodium retention — a process researchers call a natriuretic effect. Less sodium in circulation means less fluid volume, which directly reduces pressure on arterial walls. Some research suggests anthocyanins may have weak ACE-inhibitory properties, though their primary cardiovascular benefit appears to come from antioxidant and anti-inflammatory actions rather than direct enzyme inhibition.
A 2013 comprehensive review published in Fitoterapia analyzed both animal and human studies, confirming anthocyanins as the key active fraction. The same review found that hibiscus also improved lipid profiles in the majority of studies reviewed — a bonus for overall cardiovascular health.
Hibiscus vs. Prescription Medication: A Straight Comparison
This is where the evidence becomes especially clear — and it’s information that doesn’t get enough attention in popular health coverage.
Against Captopril
A 2004 clinical trial published in Phytomedicine directly compared hibiscus extract (10g of dried calyces daily, providing 9.6mg of anthocyanins) against 50mg of captopril per day — a standard ACE inhibitor used to treat hypertension.
Seventy-five adults with mild to moderate hypertension were divided into two groups for four weeks. In the hibiscus group, systolic blood pressure dropped from 139.05 to 123.73 mmHg. Diastolic fell from 90.81 to 79.52 mmHg. The therapeutic effectiveness was 78.95% for hibiscus, compared to 84.38% for captopril. Statistically, that difference was not significant. Both treatments were 100% tolerable with no reported adverse effects. This is a seminal finding, and it’s worth stating clearly: at that dose, hibiscus performed comparably to an ACE inhibitor in a clinical setting.

Against Hydrochlorothiazide (HCTZ)
A 2015 randomized controlled trial published in the Nigerian Journal of Clinical Practice tested hibiscus against hydrochlorothiazide — one of the most commonly prescribed diuretics for hypertension — in 80 newly diagnosed patients over four weeks.
Hibiscus significantly reduced systolic blood pressure, diastolic blood pressure, and mean arterial pressure. But here’s what set it apart: hibiscus caused less disruption to electrolyte balance than HCTZ. That’s a meaningful advantage. Diuretics like HCTZ can deplete potassium and sodium to problematic levels in some patients. Hibiscus produced its diuretic-like effect without that tradeoff.
There’s another finding from this study worth highlighting. One week after stopping treatment, the hibiscus group maintained lower blood pressure readings. The HCTZ group had already returned to near-baseline. That persistence suggests a sustained vascular adaptation — not just a temporary diuretic flush.
One important note: a comprehensive 2013 review of the evidence found that while hibiscus matched captopril’s effectiveness, it appeared less potent than lisinopril, a more powerful ACE inhibitor. This conclusion came from comparing different studies rather than a direct clinical trial, so it’s a relative assessment rather than a definitive head-to-head result. Hibiscus is not a replacement for all medications, and no one should stop taking prescribed drugs without talking to their doctor. But as a complement to lifestyle changes, or for those managing pre-hypertension, the evidence is genuinely strong.
A 6-Week Plan: What to Drink and When
Turning the research into a practical routine isn’t complicated.
Weeks 1–2: Building the Habit
Start with three cups of hibiscus tea daily. Space them through the day — morning, afternoon, and evening works well. Use about 1.5–2g of dried hibiscus calyces per cup. A standard commercial hibiscus tea bag typically contains 1.5–2g. This phase is about consistency more than anything else.
Weeks 3–4: Staying Consistent
Weeks 3 and 4 may be when the body’s sodium-reducing effects become more noticeable, though the research doesn’t track week-by-week changes in all participants — most trials report their results at the full 6-week mark. You may notice slightly increased urination during this phase, which is consistent with the natriuretic effect researchers observed when studying hibiscus. Some people notice mild changes in how their body feels after salty meals. Consistency with your three cups daily matters more than watching for specific timeline markers.
Weeks 5–6: Peak Response
Based on the trial data, systolic reductions in the 5–8 mmHg range are most commonly reported at this stage, particularly in those who started with elevated baseline readings. The McKay trial found that people with higher initial blood pressure responded more strongly. If your readings were in the 140–160 mmHg range before starting, you’re likely to see the most noticeable change here.
Keep a log. Track your readings at the same time each day — ideally in the morning before eating. That consistency gives you the clearest picture of what’s happening.
Is It Safe? What the Evidence Actually Says
The short answer: yes, for most healthy adults, hibiscus tea at typical doses is well-tolerated.
The 2024–2025 umbrella review found no significant effects on liver enzymes, blood glucose, or lipid levels compared to placebo — which directly addresses concerns some people have seen circulating online about liver toxicity. At normal doses (2–10g daily), hibiscus does not appear to harm the liver. The liver enzyme concern likely stems from very high-dose animal studies, not from human clinical trials at standard tea-drinking amounts.
Mild gastrointestinal side effects — nausea, stomach discomfort — were reported in some participants consuming more than 15g of hibiscus per day. At three cups a day (roughly 4.5–6g), this is not a concern for most people.
Who should be cautious:
Pregnant women should avoid hibiscus tea. Some research suggests it may stimulate uterine contractions. This is a consistent recommendation across multiple safety reviews.
People taking chloroquine (used for malaria and some autoimmune conditions) should avoid hibiscus. A study found it may reduce the absorption and effectiveness of chloroquine.
Anyone already on blood pressure medication should talk to their doctor before adding hibiscus regularly. The combined effect could lower blood pressure further than intended, especially with ACE inhibitors or diuretics.
Choosing the Right Tea
Not all hibiscus teas are equal, and the distinction matters.
Calyx, not leaf. Make sure the product uses Hibiscus sabdariffa calyces — the fleshy outer parts of the flower that surround the seed pod. These are the parts consistently used in the research and where the anthocyanin concentration is highest. Some products use hibiscus leaves or flowers, which have a different compound profile. Check the label or the product description carefully.
Check for anthocyanin content. Quality products often list anthocyanin content on the label — typically 50–100mg per serving. The clinical trials used doses providing roughly 9–250mg of anthocyanins daily, with the wide range reflecting different study protocols. If a product doesn’t list anthocyanin content, the 1.5–2g per cup guideline is a reasonable starting point, though actual potency varies depending on growing conditions, harvest timing, and drying methods. Only 15 of the 26 trials in the umbrella review independently verified the purity and strength of their hibiscus preparations — a reminder that sourcing quality material matters.
Organic where possible. Hibiscus is often grown in regions with variable pesticide regulations. For a tea you’re drinking three times a day for six weeks, choosing organic reduces unnecessary chemical exposure.
Water temperature and steeping time. There’s been concern that boiling water destroys heat-sensitive anthocyanins. Current evidence suggests that hibiscus anthocyanins are relatively stable at typical steeping temperatures. Bringing water to a boil (100°C) and then letting it cool for 30–60 seconds before pouring over dried calyces is a reasonable approach. Steep for 5–10 minutes for a stronger, more concentrated brew. Cold brewing overnight in the refrigerator is also effective and may preserve slightly more of the more delicate compounds.
Avoid adding large amounts of sugar. The tartness of hibiscus is part of what makes it distinct, and excess sugar works against the cardiovascular benefits you’re drinking it for. A small amount of honey or a squeeze of lime is a better fit.
What Happens After 6 Weeks?
It’s a fair question: do the benefits keep going, plateau, or fade if you stop?
The honest answer is that most trials end at four to six weeks, so long-term data is limited. The 2015 Nwachukwu trial showed that blood pressure reductions persisted for at least one week after stopping hibiscus — unlike HCTZ, which saw readings bounce back quickly. But what happens at week ten, or month six, isn’t yet well-documented in the research.
A sensible approach: take your blood pressure readings consistently throughout the six weeks. At the end of the protocol, check your numbers against your baseline. If readings have improved meaningfully, continuing the habit while monitoring results monthly is reasonable. If there’s minimal change after a full six weeks, talk to your doctor about other options. Hibiscus is one tool — not the only one.
Conclusion
Managing blood pressure isn’t a single-intervention problem. Diet, exercise, sleep, and stress all play significant roles. Hibiscus tea doesn’t replace any of that. What it does is add a well-studied, low-risk, pleasantly tart daily habit that the research consistently links to real reductions in blood pressure readings.
A meta-analysis published in the Journal of Hypertension in 2015 confirmed these findings across five randomized controlled trials in 390 participants. Systolic blood pressure dropped by an average of 7.58 mmHg and diastolic by 3.53 mmHg compared to control. Importantly, the effects were strongest in people with the highest baseline readings — exactly the population most likely to benefit.
Three cups a day. Six weeks. Consistent timing. Use the right product. Track your numbers. That’s the protocol that maps most closely to what the research actually tested.
If your blood pressure is mildly elevated and you’re looking for something evidence-backed to add to your daily routine, hibiscus tea is one of the more credible options available. The data behind it is no longer thin. Twenty-six trials and nearly 1,800 participants later, this is a conversation worth having with your doctor — with the research in hand.



