The muscle loss seen in active adults over 50 has a biological explanation unrelated to how hard they train.
A particular frustration is rarely discussed. It affects those who’ve consistently stayed physically active for years, lifted weights three times a week, walked, and prioritized protein.
Despite this, the body still changes: softer arms, weaker legs on stairs, and a body that no longer responds as before. The gym and effort are the same, but results differ.
Most people in this position assume they’re losing the battle against aging. And in a narrow biological sense, they’re right: muscle mass does decline with age, a process called sarcopenia. But the assumption that “aging” is the full explanation is incorrect.
Researchers have spent the last decade arriving at a more uncomfortable conclusion. For adults over 50 who exercise regularly, the hours outside the gym may matter as much as, or more than, the hours inside it.
What happens in the nine or ten hours a day that most people spend sitting is a separate biological event from exercise. And it has consequences that exercise alone can’t fully reverse.
The Active Couch Potato Problem
There’s a label researchers have started using: “active couch potato.” It describes someone who meets the standard physical activity guidelines, gets their workouts in, but spends the rest of the day almost entirely sedentary. The label implies that the workout isn’t enough.
A landmark 2015 meta-analysis by Biswas and colleagues, published in the Annals of Internal Medicine, found that sedentary time is independently associated with higher rates of disease and death, regardless of how much exercise a person does. This wasn’t a minor effect buried in an adjustment table.
Across a range of health outcomes, including cardiovascular disease, diabetes, and cancer, the harm from prolonged daily sitting persisted even after accounting for physical activity levels. The morning run, in other words, does not create a biological shield that lasts all day.
This is the core problem, and it’s worth taking note of, because most of us have built our health identity around what we do during exercise. We count the sets, the steps, the miles. We’re measuring one hour. But the other fifteen waking hours have a biological life of their own, and when those hours are spent seated, the body registers that fact at a cellular level.
Science has since moved well past this general observation. Researchers are now asking more specific questions, not just whether sitting is harmful, but exactly how it harms specific tissues, and which populations are most vulnerable.
The Sarcopenia Trigger
For physically active adults over 50, the risk data on sitting and muscle loss is startling.
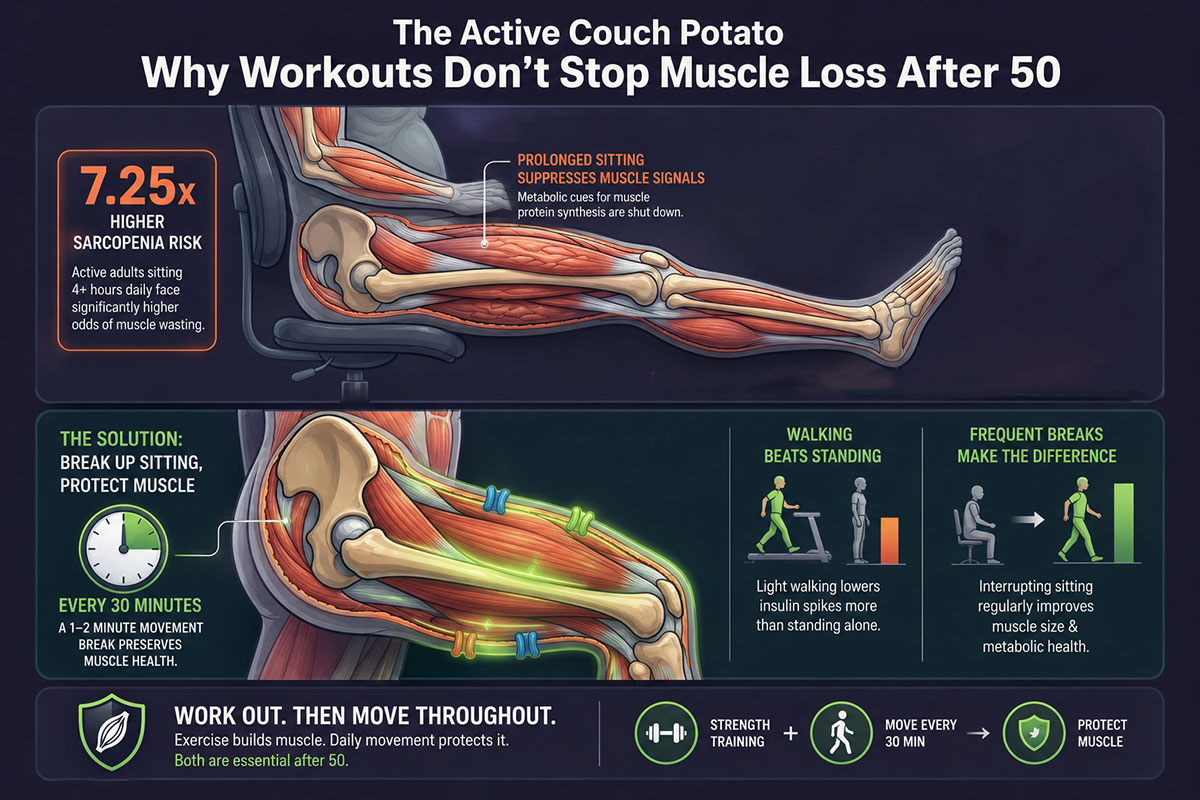
A 2023 systematic review and meta-analysis by Zhu and colleagues, published in BMC Geriatrics, examined the relationship between sedentary behavior and sarcopenia in older adults across multiple studies. The pooled analysis found that sitting for more than four hours per day was associated with odds of sarcopenia roughly 7.25 times higher in physically active older adults compared to those with lower sedentary time.

That figure represents a pooled association across the studies reviewed, not a direct causal measurement from a single trial, and it should be read with that caveat in mind. But even with appropriate statistical humility, the size of that association is not easy to dismiss. Active older adults who sit for long, unbroken stretches are not protected by their workouts. The workouts and the sitting appear to operate on separate tracks.
→ See why shorter workouts may be more effective after 50
The biological explanation for this is not simple, but the general outline is clear enough. Sarcopenia is not purely a matter of “not using” a muscle during exercise. It also depends on what the muscle is signaling between workouts, whether it’s receiving the metabolic cues that keep synthesis running, or whether those signals are being suppressed by chronic inactivity.
Prolonged sitting appears to suppress those cues in ways that a single daily workout cannot fully compensate for. The muscle that gets trained for sixty minutes then sits for nine hours is receiving contradictory information, and the sitting appears to win more often than we’d like to admit.
The Fit But Wasting Phenomenon
Here’s where the research takes a turn that is genuinely surprising.
A 2025 paper published in Nutrients examined anabolic resistance in what researchers call “master athletes,” meaning adults who have maintained lifelong exercise habits well into their 50s, 60s, and beyond. Anabolic resistance refers to a blunted muscle-building response, where the muscle doesn’t respond as efficiently to protein and exercise stimulus as it once did. This is known to increase with age in the general population. What the paper addressed is whether dedicated, lifelong exercisers escape it.
They don’t. Even in older adults who have exercised consistently for decades, the muscle’s ability to synthesize new protein in response to the usual signals is diminished compared to that of their younger counterparts. The relevant point for this discussion is that inactivity during non-exercise hours compounds this resistance.
When prolonged sitting reduces the metabolic signals that muscle tissue depends on to stay anabolic, the already-blunted response in older adults takes another hit. The fittest, most committed people in this demographic are not immune to the mechanism. They’re just better at offsetting it during their training windows, and those windows are not long enough to carry the whole day.
The conversation about muscle loss after 50 gets framed as a protein or exercise problem, and protein and exercise are genuinely important. But neither addresses what the muscle is doing, and not doing, during the other 85% of the day.
The Architecture of Sitting
Not all sedentary time is created equal, and this distinction matters in ways that should change how the problem is approached.
A 2024 PLOS ONE study by Wullems and colleagues measured sedentary behaviour and skeletal muscle architecture directly in community-dwelling older adults using accelerometers and ultrasound imaging.
Their key finding was that the pattern of sitting, specifically how it accumulates in long, unbroken bouts, had an independent negative effect on muscle size and architecture beyond what was explained by total sedentary time alone. In other words, ten hours of sitting broken up by regular movement produced less muscle damage than ten hours of sitting in one or two long stretches.
This reframes the question completely. The issue isn’t purely “how long do you sit each day.” It’s whether that sitting is fragmented or continuous. A person who sits for eight hours with regular brief breaks may be in a meaningfully different biological position than a person who sits for the same total time in uninterrupted four-hour blocks. The muscle is registering the gaps, or registering the absence of them.
The Metabolic Interruption
The mechanism connecting sitting patterns to muscle health runs through glucose and insulin signaling, and the foundational work here is surprisingly clear.
A 2012 study by Dunstan and colleagues, published in Diabetes Care, was among the first to show directly that breaking up prolonged sitting reduced post-meal glucose and insulin spikes compared to uninterrupted sitting. The practical implication was significant: brief, regular movement breaks after meals were doing measurable metabolic work that a single earlier workout was not doing.
Gillen and colleagues extended this in 2021, demonstrating that activity snacks as brief as one minute of chair stands every 30 minutes were as effective as two-minute treadmill walks for lowering post-meal insulin levels in healthy adults. No gym. No equipment. Just brief, repeated interruptions of sitting.
These interruptions matter for muscle specifically because insulin signaling is one of the mechanisms that keep muscle tissue anabolic. When post-meal insulin responses are dysregulated by prolonged unbroken sitting, the signal for muscle protein synthesis is weakened. Older adults, who already have reduced anabolic sensitivity as a baseline, take a compounded hit when their insulin signaling is further disrupted by sitting patterns that never let the glucose response settle.
The Standing Desk Trap
A popular response to the sitting problem has been the standing desk, which does not solve the problem.
Buffey and colleagues published a systematic review and meta-analysis in Sports Medicine in 2022 comparing the effects of standing versus light-intensity walking breaks on cardiometabolic markers. Light walking produced significantly greater reductions in post-meal glucose and insulin spikes than standing alone. Standing, despite feeling active and virtuous, falls short of the metabolic threshold needed to shift glucose regulation in any meaningful way.

Standing desks may reduce lower back discomfort, but they don’t replicate the metabolic effect of movement. The threshold for meaningful metabolic interruption appears to require actual locomotion, even at extremely low intensity.
The good news is that the movement required is genuinely minimal. A short walk. Repeated chair stands. A brief circuit of whatever room you’re in. The effort level is near zero. The consistency requirement is not.
Re-Engineering the Day
Repairing the daily pattern is not the same problem as improving a workout.
The workout problem is about overload, recovery, and progression. It responds to discipline applied in concentrated doses. The sitting problem is a design problem: it’s about how a day is structured, where the friction exists, and who is responsible for creating the interruptions.
Most environments are optimized for unbroken sitting. Meetings, screens, commutes, meals. Nothing in the average day automatically breaks the pattern, which means the interruptions have to be deliberately engineered.
What the research collectively points toward is not a single solution but a different way of measuring success. For adults over 50 who are already exercising, the question worth asking isn’t “did I hit my workout today?” It’s “how often did I interrupt my sitting, and did those interruptions happen every thirty minutes or so?”
The metabolic evidence suggests that frequency matters more than the intensity of each break. A ninety-second walk every half hour, repeated throughout the day, does biological work that an extra thirty minutes on the treadmill cannot replicate.
People who exercise consistently have built their health self-image around the session. The session is visible, trackable, and feels like an effort. Interrupting sitting feels like nothing because it is, physically, almost nothing.
And yet that almost-nothing, done repeatedly and consistently across the hours between workouts, is exactly what the muscle is waiting for.



