You didn’t wake up one day and suddenly fall apart. It happened slowly. A little more tired each week. A little less excited about work. A growing sense that you’re running on empty — but somehow still expected to perform.
That’s burnout. And by the time most people recognize it, they’ve been sliding toward it for months.
Burnout isn’t a dramatic collapse. It’s a slow erosion of your internal resources. Think of it like a battery that never fully charges. Each day drains a little more. Eventually, even the smallest task feels enormous.
Understanding where you are on that spectrum — before you hit zero — is what this article is about.
What Burnout Actually Is
Burnout isn’t just being “really stressed.” It has a specific, three-part definition that researchers have studied since the early 1980s.
Psychologists Christina Maslach and Susan Jackson developed the gold-standard measurement tool for burnout — the Maslach Burnout Inventory (MBI) — after studying burnout across a wide range of professions involving care and service. Their 1981 research confirmed that burnout is made up of three distinct dimensions: emotional exhaustion, depersonalization, and a reduced sense of personal accomplishment. This three-part model is still the foundation of burnout research today.
These three dimensions work together. They feed each other. And they tend to show up in patterns that are easy to miss until they’ve already taken root.
The stakes are higher than most people realize. A large-scale review by Salvagioni and colleagues (2017), which analyzed dozens of studies across multiple industries, found that chronic burnout is linked to a significantly increased risk of heart disease, depression, insomnia, and long-term absence from work. The longer someone stays in a burned-out state, the harder recovery becomes.
This is why catching the early warning patterns matters.

Pattern 1: You’ve Stopped Caring About People
One of the first signs of burnout isn’t exhaustion. It’s a quiet shift in how you see the people around you.
You used to care. You were patient with clients, engaged with colleagues, present in meetings. Now, people feel like problems. Their needs feel like interruptions. You find yourself getting irritated by things that never used to bother you.
This is depersonalization — a psychological defense mechanism. When your internal resources are depleted, your brain starts protecting itself by creating emotional distance. It’s not that you’ve become a bad person. It’s that your system is overwhelmed and trying to cope.
The tricky part? This shift feels justified. You tell yourself the people around you really are more demanding, or that your cynicism is just “being realistic.” That’s the defense mechanism talking.
The early check: Ask yourself whether you’ve started thinking about people at work in cold or dismissive ways. Are you rolling your eyes more? Dreading interactions you once looked forward to? Have people or activities that used to energize you started to feel like obligations? These small shifts are worth paying attention to.
The difference between a bad day and a pattern is repetition. One rough afternoon doesn’t mean much. Three weeks of dreading every meeting does.
Pattern 2: Your Body Is Sending Signals You’re Ignoring
Burnout isn’t only mental. It has a clear physical footprint — and your body often picks up on it before your mind is ready to admit something is wrong.
The most telling physical symptom is what researchers call “tired but wired.” You’re exhausted during the day, struggling to focus, dragging yourself through tasks. But at night, you can’t shut your brain off. You lie awake running through tomorrow’s to-do list, replaying conversations, bracing for what’s coming next.
This is a sign of HPA axis dysregulation — a disruption in the hormonal system that manages your stress response. Under normal conditions, cortisol rises in the morning to get you going and drops at night to let you rest. Chronic stress scrambles that rhythm.
Melamed and colleagues (2006) tracked workers over several years and found that chronic burnout was associated with elevated cortisol levels and measurable changes in how the body manages cardiovascular stress — independent of other known risk factors for heart disease. This means burnout can affect your heart health even when everything else looks fine on paper.
Other physical warning signs include getting sick more often than usual, frequent tension headaches, and heart palpitations that your doctor can’t easily explain. These aren’t random. They’re your immune and cardiovascular systems responding to sustained overload.
The early check: Have you been catching every cold that goes around? Are you waking up between 3 and 5 a.m. with your mind already racing? Are you noticing chest tightness or pounding heartbeats during moments that shouldn’t be stressful? These physical signals are worth taking seriously.
Pattern 3: You’re Working More and Getting Less Done
There’s a painful irony at the core of burnout: the harder you push, the less you produce.
You might be putting in longer hours than ever. But somehow, the work isn’t getting done. Decisions that used to be easy now feel enormous. Simple emails sit in your drafts folder for days. You read the same paragraph four times and still can’t focus.
This is the productivity paradox of burnout. And it’s not a motivation problem. It’s a cognitive one.
Burnout impairs executive function — the brain’s ability to plan, prioritize, and follow through. The prefrontal cortex, which handles complex thinking and decision-making, is highly sensitive to chronic stress. When it’s overloaded, even straightforward tasks require a level of mental effort that feels exhausting.
At the same time, a growing sense of “imposter syndrome” often creeps in. You start to believe your work doesn’t matter, or that you’re not capable of doing it well — even when people around you say otherwise. External praise starts to feel hollow. You can’t trust it.
This was captured clearly in Maslach and Jackson’s research: reduced personal accomplishment — the sense that your efforts no longer translate into meaningful results — is one of the three core dimensions of burnout, and it tends to deepen the more the other two dimensions take hold.
The early check: Are you taking much longer than usual to complete tasks? Do compliments from your manager feel empty or even annoying? Is your to-do list growing even on days when you worked non-stop? These are signs that burnout may already be affecting your cognitive performance.
Pattern 4: You’ve Pulled Back From the People You Like
Burnout makes you want to disappear.
Not in a dramatic way. You’re not picking fights or announcing that you need space. You’re just quietly declining invitations. Skipping the group chat. Going home and closing the door.
And here’s the key distinction: it’s not that you’re too busy. It’s that the thought of engaging with other people — even people you genuinely like — feels like too much effort. Your social battery isn’t just low. It feels broken.
This withdrawal is often followed by a specific kind of coping: numbing out with low-effort, high-stimulation activities. Scrolling social media for an hour. Watching three episodes of something you’re not even that interested in. Not because it’s enjoyable, but because it requires nothing from you.
There’s a reason for this. These activities offer a quick dopamine signal with almost no cognitive cost. For a brain running on fumes, that trade-off feels like relief. But it’s not recovery. It’s avoidance. And the next morning, you feel just as depleted — sometimes more so.
The early check: Think about the last few weeks. Have you been turning down plans not because of scheduling, but because you just couldn’t face the energy it would take? Have social activities that once recharged you started to feel like obligations? Are your evenings mostly spent in passive consumption rather than anything that actually restores you? This pattern is worth noticing.
Pattern 5: You Can’t Turn Your Brain Off
Even when you leave the office — physically — work comes with you.
You’re at dinner, but you’re mentally drafting a reply to that email. You’re trying to fall asleep, but you’re running through the meeting you have tomorrow. You’re on a walk, but you’re calculating how you’re going to get everything done this week.
This is one of the most insidious patterns of burnout. The inability to mentally disconnect from work — even during time that’s supposed to be off — is both a symptom and a cause of continued deterioration.
It’s directly tied to sleep. Burnout-related insomnia has a specific profile that differs from ordinary sleep trouble. The most common sign isn’t difficulty falling asleep. It’s early morning awakening — waking up at 3 or 4 a.m. with your mind already full of work-related thoughts, unable to get back to sleep.
This matters because sleep is the primary window during which the brain processes stress and restores cognitive resources. When rumination cuts that window short, you start the next day already behind. It’s a cycle that compounds over time.
The Salvagioni (2017) meta-analysis found sleep disturbance to be one of the most consistent outcomes linked to burnout across studies — appearing in workers across industries and job types. It’s not a coincidence. It’s a mechanism.
The early check: Can you genuinely “leave work” when you leave work? If you’re spending your evenings and early mornings mentally at the office, that cognitive anchor is a clear warning sign.
Why “Just Do Self-Care” Isn’t the Answer
Here’s something most burnout articles won’t tell you: a 10-minute meditation app won’t fix a 60-hour workweek.
That’s not to say individual practices don’t matter. They do. But placing the full burden of recovery on the individual ignores a significant part of what the research actually shows.
A 2017 meta-analysis by Panagioti and colleagues looked at controlled trials comparing individual-focused interventions — like mindfulness and resilience training — against organizational-level changes like reducing workload, increasing autonomy, and improving support systems. The organizational interventions had significantly larger effect sizes. They also produced more lasting results.
West and colleagues (2016), in a large analysis published in The Lancet, found similar results: both mindfulness-based and structural changes reduced burnout, but changes to workload, autonomy, and team support outperformed personal resilience training alone.
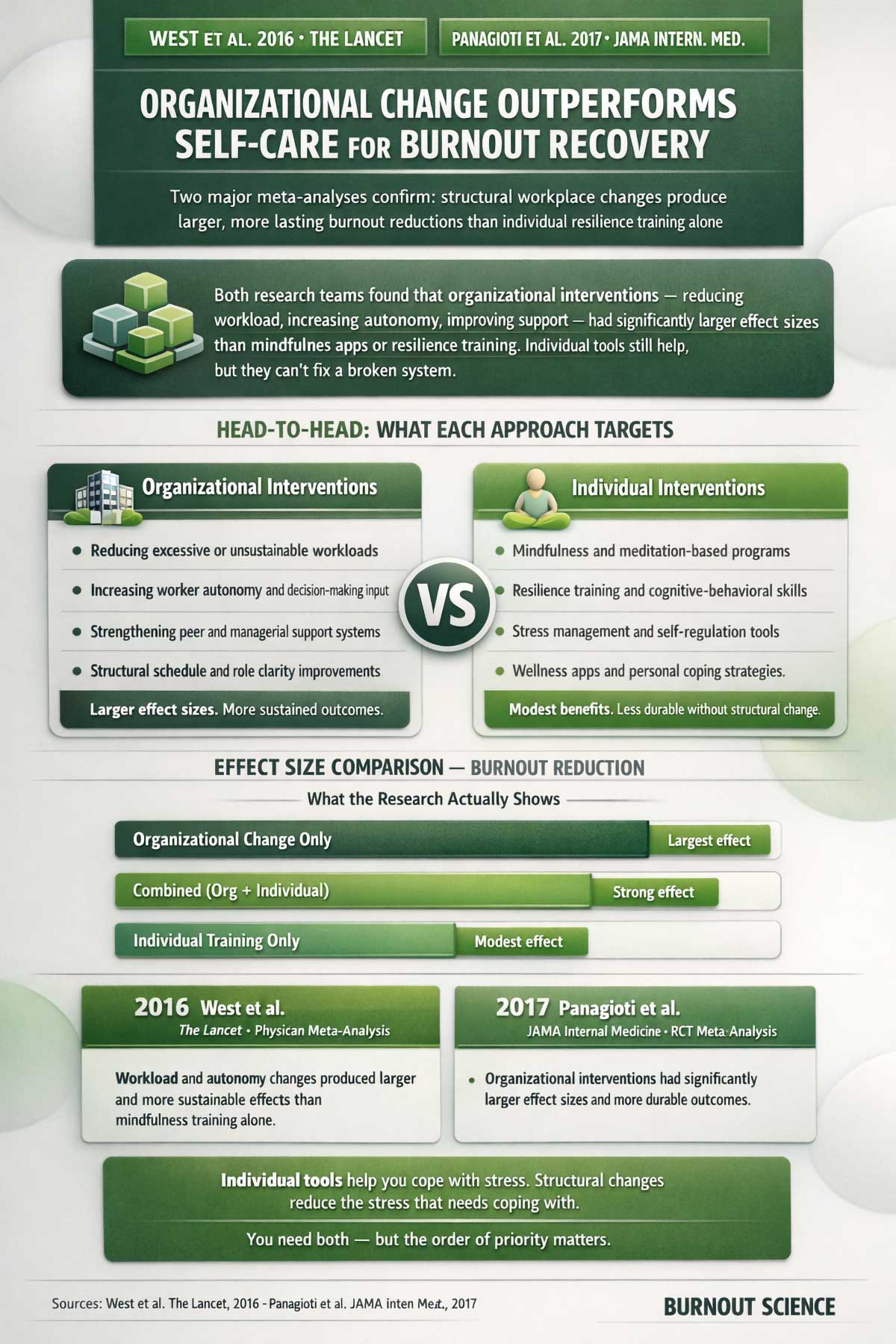

This isn’t an argument against self-care. Mindfulness, sleep hygiene, and stress-reduction practices do help. A review by Luken and Sammons (2016) found that mindfulness-based interventions consistently reduced emotional exhaustion and stress-related symptoms. But those practices work best as part of a larger strategy — not as a substitute for addressing the conditions that caused burnout in the first place.
The honest framework is this: individual tools help you cope with stress. Structural changes reduce the stress that needs to be coped with. You need both.
A Structured Path Back
For those looking for more than ad hoc coping strategies, structured interventions offer a more reliable path.
A pilot study by Sood and colleagues (2011) tested a 12-week program called Stress Management and Resilience Training (SMART) with healthcare professionals — a group with notoriously high burnout rates. Participants showed measurable improvements in burnout scores, reduced anxiety, and better stress resilience. Those gains held up at follow-up. The key wasn’t willpower or motivation — it was structure and consistency over time.
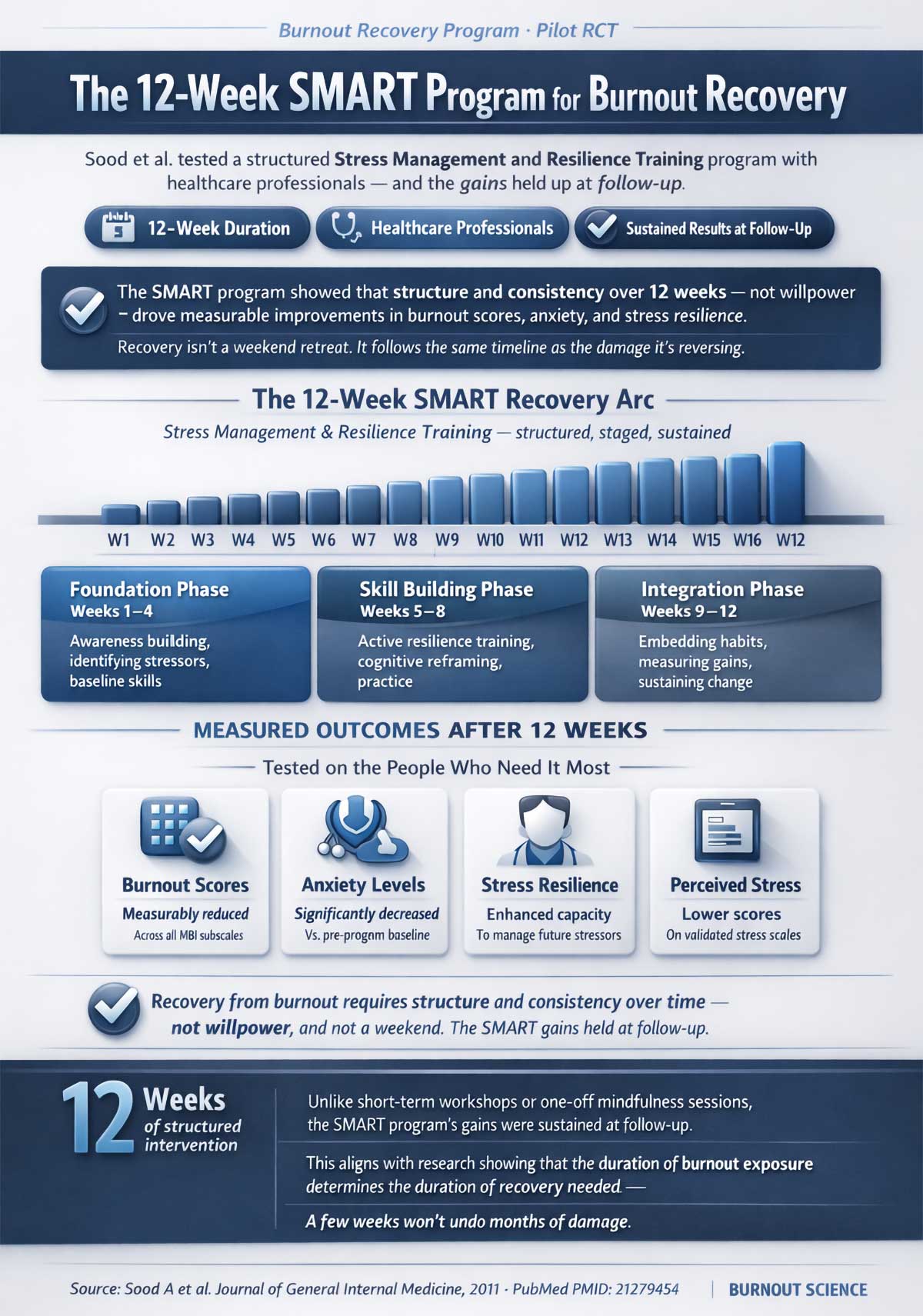
The takeaway: recovery from burnout isn’t something that happens in a weekend. It follows a timeline proportional to how long you’ve been running on empty.
A review by Awa and colleagues (2010), which looked at burnout prevention across multiple healthcare settings, found that both individual and organizational interventions reduced burnout — but that sustained improvement required follow-through over months, not days. The longer the pattern has been in place, the longer meaningful recovery takes.
This is the dose-response relationship that the research points to: the more cumulative exposure to burnout conditions, the more time and effort recovery requires. Recognizing early warning patterns isn’t just useful — it’s how you keep a manageable problem from becoming a long-term health consequence.
Your Next Steps: A Practical Checklist
If you recognized yourself in three or more of the patterns above, it’s worth taking action now — not later.
For immediate action on your own: Work-related rumination at night can often be reduced with simple “cognitive offloading” — writing down everything on your mind before bed rather than carrying it mentally. This isn’t a cure, but it can break the sleep disruption cycle enough to start recovering.
Try to carve out at least one hour of genuine offline time before sleep. Even modest consistency here makes a difference over time. And start identifying which parts of your workload are the biggest sources of depletion — and which ones are within your ability to push back on. If enforcing that boundary feels impossible on your own, that’s exactly when talking to your manager or seeking professional support becomes important.
When to seek professional support: If you’ve been experiencing these patterns consistently for more than a few weeks — especially the physical symptoms and the inability to disengage from work — it’s worth speaking to a doctor or mental health professional. The physiological changes that Melamed and colleagues documented don’t resolve on their own without some form of intervention.
If your burnout is tied to your workplace, a structured conversation with your manager about workload, boundaries, or support isn’t a sign of weakness. According to the research, it’s actually the higher-leverage move.
When to reassess the bigger picture: Some workplaces have persistent, systemic problems — chronic understaffing, impossible expectations, or a culture that treats burnout as a badge of honor. In those environments, the most important step isn’t better coping. It’s an honest reassessment of whether the role itself is sustainable for you. Recovery requires conditions that allow for recovery. If those conditions don’t exist where you are, that’s worth facing directly.
The bottom line: Burnout is not a personal failure. It’s a predictable response to sustained, unmanaged demands. The patterns are identifiable. The research is clear. And the earlier you catch it, the more options you have.



