Most people who eat lentils for cholesterol see zero change on their lab results. The fix isn’t eating more. It’s understanding what to eat less of.
Clinical research has moved lentils well beyond pantry-staple status. A growing body of evidence shows they can lower LDL (“bad” cholesterol) in a measurable, predictable way. But there’s an overlooked factor that decides whether you’ll actually see that result on your next blood test. Most articles never mention it.
Here’s what really happens inside your body over six weeks of daily lentil eating, and the one thing that determines whether it works.
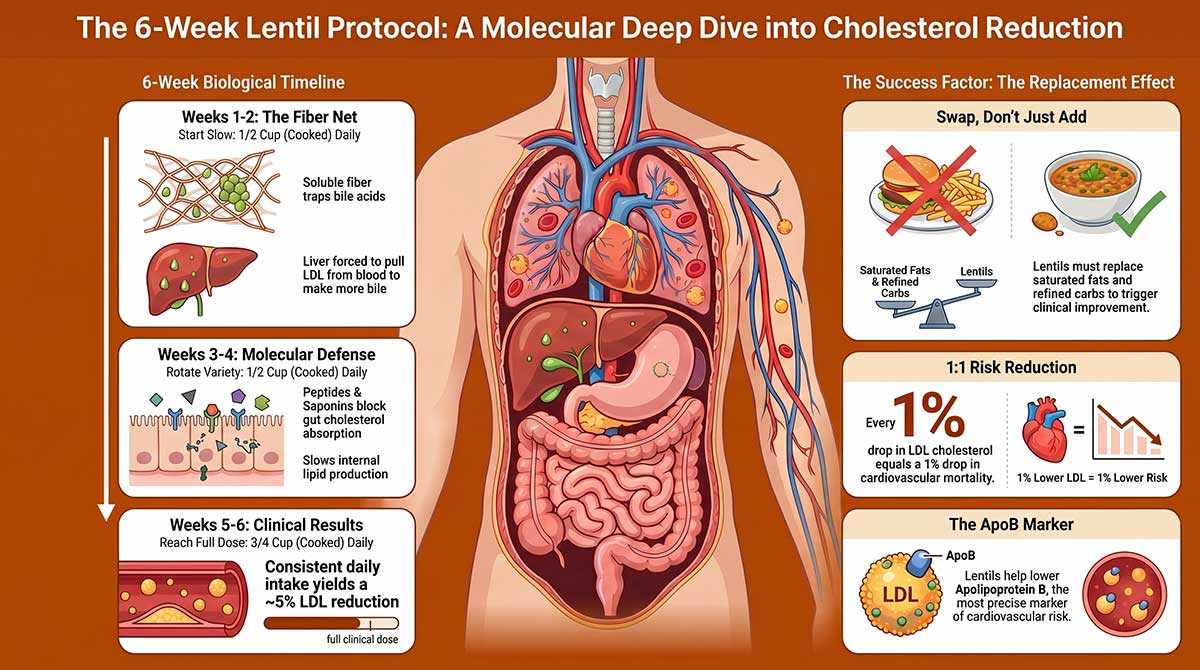
Week 1 to 2: Your Gut Gets to Work
The first thing lentils do has nothing to do with your liver. It starts in your digestive tract.
Lentils are packed with soluble fiber. Picture a slow-moving net being dragged through your intestines. As it travels, it catches bile acids, the compounds your digestive system makes from cholesterol to break down fats. Normally, your body recycles about 95% of those bile acids, looping them back to the liver to be used again. Soluble fiber breaks that loop. It traps the bile acids inside the net and carries them out through your stool.
Here’s where your LDL enters the picture. Your liver needs a fresh supply of bile acids to keep digesting your next meal. With its recycled stock gone, it has only one place to get the raw material: circulating LDL in your bloodstream. It pulls LDL out of the blood and converts it into new bile. Your LDL level drops as a direct result. That’s the mechanism. It’s well-documented and it kicks in within the first two weeks.
A 2011 meta-analysis by Bazzano and colleagues, published in Nutrition, Metabolism and Cardiovascular Diseases, pooled data from 10 clinical trials and confirmed this effect. Non-soy legume diets produced a measurable drop in both total cholesterol and LDL compared to control diets. The soluble fiber pathway was central to those results.

Practical tip: In the first two weeks, start with about 1/2 cup of cooked lentils per day. Your gut microbiome needs time to adjust to the extra fiber. Starting slow keeps bloating in check.
Week 3 to 4: Something Deeper Is Happening
By weeks three and four, lentils are doing more than sweeping out bile acids.
Digestion breaks lentil proteins down into smaller fragments called bioactive peptides. These aren’t just nutrition; they’re active compounds that interact with your cells. Research published in Nutrients in 2025 analyzed the molecular pathways involved and found that legume-derived peptides can interfere with fatty acid synthesis at the cellular level. This means they may slow the liver’s own production of lipids from the inside out.
Lentils also contain compounds called saponins. These plant chemicals can form insoluble complexes with cholesterol molecules inside the gut, blocking some of that cholesterol from being absorbed into the bloodstream in the first place. A peer-reviewed overview published in Pharmaceuticals (2022) confirmed that lentil saponins have a measurable plasma cholesterol-lowering effect in humans through this direct cholesterol-binding route, adding yet another layer to what fiber alone provides.
The fiber story, the peptide story, and the saponin story work together. Older articles on lentils for cholesterol typically only tell the first one. That’s why the real benefit is larger than most people expect.
The 2024 Nutrients scoping review by Zhao, Jiao, Chiu, and Wallace mapped evidence from 30 studies, including 17 randomized controlled trials, and confirmed that pulses including lentils produce consistent, favorable changes in LDL cholesterol and blood glucose markers across diverse populations. The benefits were seen across different global diets, different pulse varieties, and different preparation methods.
Practical tip: Try eating different types of lentils across the week: red, green, and black beluga. Each variety has a slightly different protein and saponin composition. More variety may mean broader benefit.
Week 5 to 6: The Numbers Move
By the end of six weeks, the compounding effect of daily lentil eating becomes visible on a lipid panel.
The landmark meta-analysis by Ha and colleagues, published in the Canadian Medical Association Journal, reviewed 26 randomized controlled trials with 1,037 participants. The median intake was about 3/4 cup of cooked pulses daily. The result: a roughly 5% reduction in LDL cholesterol. That may sound modest, but the same paper notes that a 1% drop in LDL is associated with a 1% drop in cardiovascular mortality. A 5% LDL reduction translates to a meaningful real-world risk reduction.
Research from the Portfolio Diet program, led by Jenkins and colleagues and published in JAMA (2011), extended this further. The Portfolio Diet study tracked adults with high cholesterol over six months and found that legumes, as part of a targeted dietary approach, produced significant reductions in LDL and Apolipoprotein B (ApoB). ApoB is the protein that wraps around LDL particles. High ApoB is one of the most precise markers of cardiovascular risk, arguably more telling than LDL alone.

A related finding from Jenkins et al. published in the Journal of Nutrition (2012) showed ApoB reductions in adults with existing high cholesterol who followed a legume-rich dietary pattern for one month, suggesting these effects can begin even before the six-week mark.
By weeks five and six, most people who’ve followed the daily habit consistently will also notice that their blood sugar response to meals has smoothed out. Glycemic control and cholesterol management are closely linked, and lentils appear to support both at once.
Practical tip: This is the time to ramp up to the full clinical dose: about 3/4 cup of cooked lentils per day. To be clear, that means cooked. Three-quarters of a cup of dry lentils would more than double that volume once boiled, which is far beyond what the trials used. Measure after cooking.
The Overlooked Factor: Why Most People Fail
Here’s the part that nearly every article on lentils for cholesterol skips entirely.
Lentils do not work in a vacuum.
If you add lentils to an existing diet built around white rice, pasta, processed snacks, and fatty meats, your cholesterol panel will barely change. The research is clear about this. Clinical success depends on what’s called the “Replacement Effect”: the act of swapping lentils in place of refined carbohydrates or high-saturated-fat foods, not just piling them alongside.
Saturated fat is the specific dietary villain here. It’s found in fatty cuts of red meat, butter, full-fat dairy, and processed meats. It directly signals the liver to produce more LDL. Refined carbohydrates, the other key offender, do the same through a different pathway. Both keep your liver in LDL-making mode regardless of how much soluble fiber you eat.
A 2021 review in Nutrients, which analyzed multiple studies across a 4-to-12-week window, identified the Replacement Effect as the primary driver of cardiovascular improvement. Simply adding legumes on top of a poor diet produced weak results. Replacing refined carbs and high-saturated-fat foods with legumes produced consistent, measurable ones.

The JAMA Portfolio Diet study supports this directly. Its success came not from addition, but from substitution. Legumes took the place of foods that were actively raising LDL. The fiber bound bile acids, yes. The peptides and saponins slowed cholesterol absorption, yes. But all of that was amplified because the saturated fat and refined carb competition was removed.
Think of it this way: lentils are excellent at pulling LDL out of your blood. But if you’re simultaneously flooding your system with saturated fat, the liver just makes more. Lentils can’t outrun a diet that keeps filling the pipeline.
What this looks like in practice:
Swap your white rice at lunch for a lentil salad. Use lentil pasta instead of wheat pasta. Replace a meat-heavy dinner twice a week with a lentil-based main dish. These aren’t small tweaks; they’re the actual mechanism behind the clinical results.
Your 6-Week Challenge
Here’s the simplified timeline:
Weeks 1 to 2: Your soluble fiber intake rises. Your liver starts pulling LDL out of your blood to replenish the bile acids your body is now excreting. Start at 1/2 cup of cooked lentils per day.
Weeks 3 to 4: Bioactive peptides and saponins from lentils begin working at the cellular level. Lipid production slows at the source and cholesterol absorption drops in the gut. Keep the habit going and vary your lentil types.
Weeks 5 to 6: The compounding effect becomes measurable. LDL and ApoB drop. Blood sugar response improves. Ramp up to about 3/4 cup of cooked lentils daily. This is when your lipid panel should start telling a different story.
The golden rule throughout: lentils replace, not just accompany. Make them the main event.
Three easy batch-cooking ideas to get you started:
- No-soak red lentil soup: Red lentils need no soaking. Simmer them with canned tomatoes, garlic, and cumin for 20 minutes. Cook a large pot on Sunday and eat it through the week.
- Green lentil salad base: Cook green lentils in about 25 minutes. Toss cold with olive oil, lemon, parsley, and whatever vegetables are in the fridge. Use it as the base where you’d normally use rice or pasta.
- Black beluga lentils as a side-to-main swap: These hold their shape after cooking. Dress them warm with mustard vinaigrette and serve them as the centerpiece of a meal instead of a starchy side.
Cook them in bulk. Keep them in the fridge for up to five days. The habit part is easy once the lentils are already made.
Six weeks from now, test your bloodwork. If you replaced saturated fat, refined carbs, and high-fat proteins with daily lentils at the right dose, the science says you’re likely to see a real change. Not because lentils are special in some vague sense, but because the biology, done right, actually works.
A note on the research: Some studies in this area used mixed pulses (beans, chickpeas, peas) rather than lentils alone. Effects specific to lentils may vary. If you have existing cardiovascular disease or take cholesterol-lowering medications, speak with your doctor before making significant dietary changes.



