Age-related macular degeneration (AMD) affects more than 11 million Americans and remains the leading cause of blindness in adults over 50. Meanwhile, the average person spends seven hours daily staring at screens. Your eyes weren’t built for this. The economic burden of vision loss exceeds $139 billion annually in the United States alone—not counting the immeasurable impact on quality of life.
Scientists have spent decades testing which supplements actually protect your eyes. We’ve sorted through the evidence—from massive government-funded trials to smaller studies—to show you what works, what doesn’t, and what might surprise you. In the next 10 minutes, you’ll know exactly which supplements your eyes actually need. Let’s separate the science from the marketing hype.
Understanding the Evidence: What Makes a Study Trustworthy?
Before we get into specific supplements, you need to know how we evaluated the evidence. Not all studies carry equal weight.
Gold standard studies are randomized controlled trials (RCTs) with thousands of participants followed for years. These studies use hard endpoints—actual vision loss or disease progression—not just lab measurements.
Strong evidence comes from multiple RCTs showing consistent results in targeted populations. These might have smaller sample sizes but still use rigorous methods.
Emerging evidence includes smaller trials or newer research that shows promise but needs confirmation from larger, independent studies.
Weak evidence comes from inconsistent results, very small sample sizes, or studies that only measure indirect markers without proving actual clinical benefit.
We’ve ranked every supplement in this article using these criteria. No guessing. No marketing hype. Just science.
1. The AREDS2 Formula
What the Research Actually Shows
The Age-Related Eye Disease Study (AREDS) represents the gold standard in supplement research. Published in 2001, this National Eye Institute trial followed 4,757 people aged 55-80 for an average of 6.3 years. The results were clear: a specific combination of nutrients slowed AMD progression by 25% over five years.
But here’s the catch that most articles miss: this formula only works if you already have intermediate or advanced AMD. If your eyes are healthy, taking these supplements will most likely not prevent AMD from starting. The study specifically excluded people with early AMD or no AMD, so we have no evidence it helps prevent the disease from developing.
Why AREDS2 Fixed What AREDS Got Wrong
The original formula contained beta-carotene. Bad idea. Post-hoc analysis revealed that beta-carotene increased lung cancer risk by 18% in current and former smokers. The follow-up study (AREDS2), published in 2013 with 4,203 participants, replaced beta-carotene with lutein (10mg) and zeaxanthin (2mg). The new version worked just as well without the danger.
The formula also originally packed 80mg of zinc—enough to cause stomach upset, copper deficiency, and immune problems. AREDS2 tested a lower dose of 25mg and found it equally effective with fewer side effects. About 40% of participants in the original study reported stomach problems with the high-dose zinc.
| Nutrient | AREDS (2001) | AREDS2 (2013) | Reason for Change |
|---|---|---|---|
| Vitamin C | 500mg | 500mg | No change needed |
| Vitamin E | 400 IU | 400 IU | No change needed |
| Beta-Carotene | 15mg | REMOVED | 18% increased lung cancer risk in smokers |
| Lutein | None | 10mg | Safer replacement for beta-carotene |
| Zeaxanthin | None | 2mg | Safer replacement for beta-carotene |
| Zinc | 80mg | 25mg | Equal efficacy, fewer side effects |
| Copper | 2mg | 2mg | Prevents zinc-induced anemia |
What “Intermediate AMD” Actually Means
You can’t self-diagnose this. Your eye doctor needs to examine your retina and look for drusen—yellow deposits under the retina. Intermediate AMD means you have medium-sized drusen (63-125 micrometers) or at least one large drusen (over 125 micrometers). Advanced AMD in one eye also qualifies you for this formula.
If you have AMD, you’ll likely notice:
- Blurred central vision
- Difficulty recognizing faces
- Straight lines appearing wavy
- Dark or empty spots in central vision
- Colors appearing less vivid
The Updated Formula That Actually Works
If you have intermediate AMD or advanced AMD in one eye, here’s what you need:
- Vitamin C: 500mg
- Vitamin E: 400 IU
- Zinc: 25mg
- Copper: 2mg (only there to prevent zinc-induced anemia)
- Lutein: 10mg
- Zeaxanthin: 2mg
Your ophthalmologist needs to diagnose AMD before you start this regimen. Taking high-dose zinc and vitamin E without medical reason can cause more harm than good. Some meta-analyses have linked 400 IU of vitamin E to slightly increased all-cause mortality and hemorrhagic stroke risk, though the data remains debated.
The omega-3 fatty acids that many companies add to “AREDS-type” formulas? They showed no additional benefit when tested in AREDS2. Don’t pay extra for them in this context.
Brand Shopping: Formula vs. Marketing
Many brands claim “AREDS2 formula” but don’t match the studied doses. When shopping, look for:
- Exact ingredient amounts matching the table above
- USP verification or third-party testing (ConsumerLab, NSF)
- No “proprietary blends” hiding actual doses
- Zinc as zinc oxide (the form studied)
- Lutein free from synthetic sources when possible
Buying ingredients separately might save $5-10 monthly, but combination formulas ensure you get the right ratios. Generic store brands often match name brands for half the price—just verify the doses match exactly.
Bottom line: This formula works, but only for people with diagnosed intermediate or advanced AMD. Taking it “just in case” wastes money and exposes you to unnecessary risks from high-dose zinc and vitamin E.
2. Lutein and Zeaxanthin
Think of these as internal sunglasses. They’re the only nutrients that concentrate specifically in your macula—the tiny spot in your eye responsible for sharp, central vision.
How They Actually Work
Lutein and zeaxanthin filter harmful blue light before it reaches your retina’s light-sensitive cells. They also act as antioxidants, neutralizing free radicals that damage eye tissue over time.
Scientists measure their effect by checking macular pigment optical density (MPOD). This test uses flickering lights to determine how much protective pigment you have in your macula. Higher density means more protection. Studies consistently show that taking 10-20mg of lutein daily increases MPOD and improves visual function.
Blue light isn’t just from screens. The sun produces far more blue light than any device. However, we spend less time outdoors than our ancestors did, and we eat fewer leafy greens—the main dietary source of these protective pigments. This double deficit leaves modern maculas more vulnerable.
The Evidence That Changed Everything
A 2012 meta-analysis published in the British Journal of Nutrition examined six prospective studies involving 41,999 participants. People with higher dietary intake of lutein and zeaxanthin had a 26% lower risk of developing late-stage AMD. The relationship showed a dose-response pattern: more intake meant more protection.

The LUTEGA study, conducted in Germany with 108 participants over 12 months, found that 12mg lutein plus vitamins improved visual acuity and contrast sensitivity in people with early AMD. Macular pigment density increased significantly in the supplement group but not in controls.
Real-World Benefits You’ll Notice
After 6-12 months of supplementation, many people report:
- Better contrast sensitivity (easier to see in low light)
- Faster recovery from bright glare
- Improved night driving
- Sharper vision overall
- Less difficulty reading in dim conditions
These aren’t dramatic overnight changes. But for people who don’t eat leafy greens regularly, supplementation makes sense. Your body can’t make these nutrients on its own. You must get them from food or supplements.
How Much Do You Need?
Most effective studies used 10mg lutein plus 2mg zeaxanthin daily. Some newer formulas include meso-zeaxanthin—the third carotenoid found in the macula. This compound sits at the very center of the macula, while lutein and zeaxanthin distribute more around the edges. The evidence for adding it is promising but not yet definitive.
Can you get too much? Probably not from supplements at typical doses. No upper limit has been established because no toxicity has been observed even at 20mg daily for years. The only documented side effect is carotenodermia—a harmless yellowing of the skin that reverses when you stop supplementation.
One caution: High-dose beta-carotene supplements can compete with lutein and zeaxanthin for absorption. If you take a multivitamin, check that it uses mixed carotenoids or excludes beta-carotene entirely.
Do You Need MPOD Testing?
Some optometry practices offer macular pigment density testing. Is it worth the cost?
For most people, no. If you’re taking lutein and zeaxanthin consistently, your MPOD will increase regardless of whether you measure it. The test costs $50-150 and isn’t covered by insurance.
Testing makes sense if:
- You have early AMD and want to track response to supplementation
- You have a strong family history of AMD
- You want objective motivation to maintain supplementation
Otherwise, save the money and put it toward higher-quality supplements or more leafy greens.
Food Sources: Can You Eat Your Way There?
| Food Source | Serving Size | Lutein (mg) | Zeaxanthin (mg) | Additional Benefits |
|---|---|---|---|---|
| Kale (cooked) | 1 cup | 23.7 | 0.5 | Vitamins A, C, K, calcium |
| Spinach (cooked) | 1 cup | 20.4 | 0.3 | Iron, folate, magnesium |
| Collard greens | 1 cup | 14.6 | 0.4 | Calcium, vitamin K |
| Turnip greens | 1 cup | 12.2 | 0.2 | Vitamin C, calcium |
| Swiss chard | 1 cup | 10.0 | 0.2 | Magnesium, potassium |
| Egg yolks | 2 large | 0.3 | 0.2 | Highly bioavailable form |
| Corn (cooked) | 1 cup | 1.8 | 1.3 | Higher zeaxanthin than most foods |
| Orange peppers | 1 cup raw | 0.3 | 2.8 | Highest zeaxanthin vegetable source |
| Zucchini | 1 cup cooked | 2.5 | 0.3 | Low calorie, high fiber |
Notice that egg yolks provide relatively small amounts but in a highly absorbable form. The fat in egg yolks helps your body absorb the carotenoids. This matters because lutein and zeaxanthin are fat-soluble.
To hit 10mg lutein from food alone, you’d need about half a cup of cooked kale or spinach daily. Zeaxanthin is harder—you’d need 10 cups of orange peppers to get 2mg. This is why supplementation often makes more practical sense than food alone, especially for zeaxanthin.
When Supplements Make More Sense Than Food
Consider supplements if you:
- Don’t eat leafy greens at least 4-5 times weekly
- Have digestive issues that limit vegetable intake
- Take medications that interfere with fat absorption
- Have genetic variants affecting carotenoid metabolism
- Want insurance against dietary gaps
Unlike the AREDS formula, this combination is safe for everyone. No copper deficiency risk. No stomach issues. Just consistent daily intake.
Quick takeaway: Lutein and zeaxanthin have the strongest evidence of any single-ingredient eye supplements. They work for prevention in healthy eyes, unlike AREDS2, which only helps existing AMD. If you take just one supplement for eye health, this should be it.
3. Astaxanthin
Your eyes aren’t designed for eight-hour screen marathons. That tight, tired feeling by afternoon? That’s your ciliary muscles—the tiny muscles that change your lens shape for focusing—crying for help.
What Makes This Different
Most eye supplements target the retina. Astaxanthin works differently. It’s a carotenoid like lutein and zeaxanthin, but it doesn’t accumulate in the macula. Instead, it concentrates in the ciliary body and improves the muscle’s ability to contract and relax through the day.
A 2012 Japanese study with 49 participants compared 6mg daily astaxanthin to placebo in people with eye strain. After four weeks, the astaxanthin group showed significant improvements in accommodation amplitude—the eye’s ability to shift focus from near to far. Accommodation time also decreased, meaning eyes could refocus faster. The placebo group showed no changes.
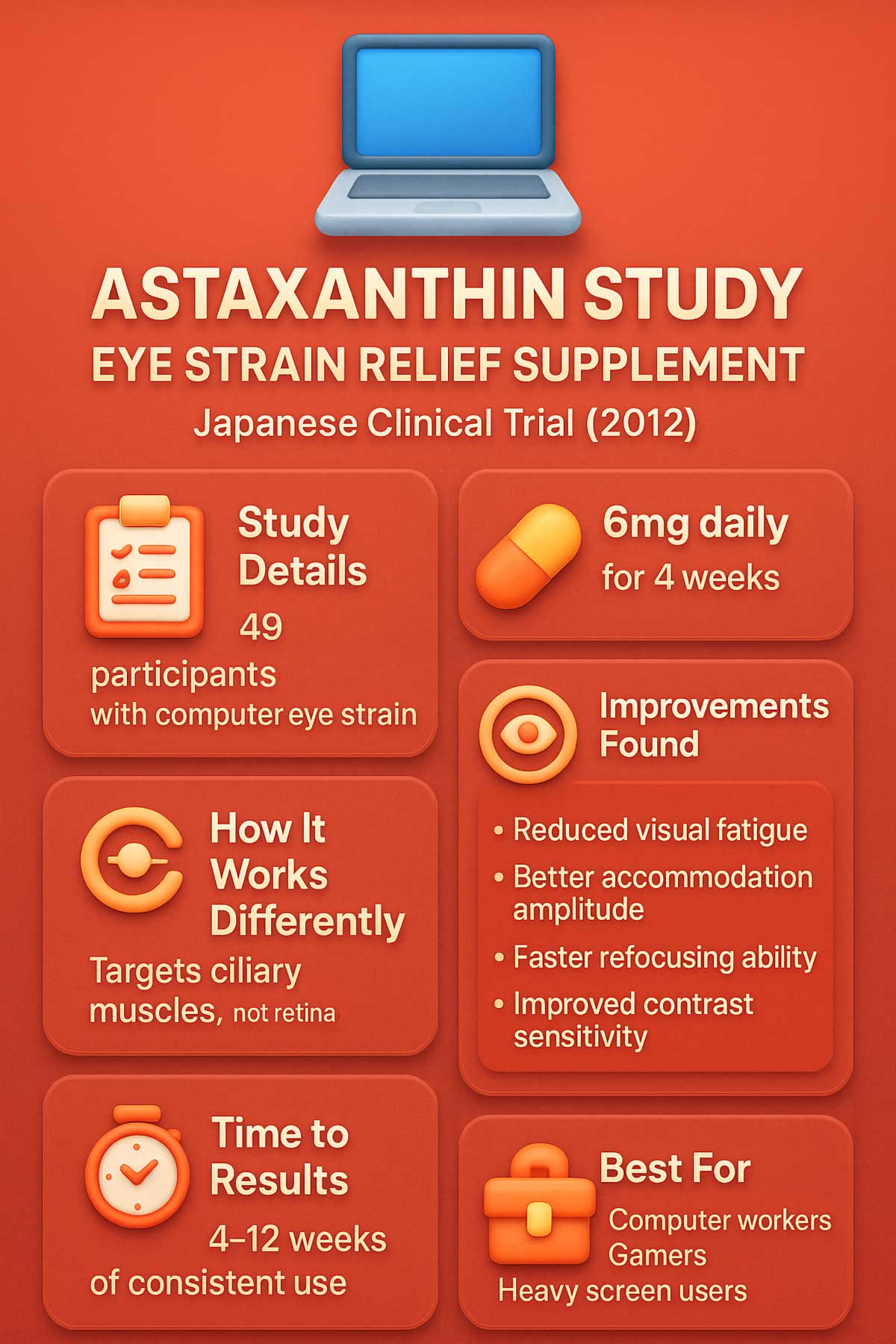
The Science Behind Screen Fatigue
When you look at a screen, your ciliary muscles contract to thicken your lens for near focus. They stay contracted for hours. This causes:
- Muscle fatigue (the tired, heavy feeling)
- Reduced accommodation range (blurry vision when looking up)
- Slower refocusing ability (takes longer to see clearly after changing distance)
- Tension headaches from sustained muscle contraction
Astaxanthin appears to improve mitochondrial function in these muscles, giving them more energy for sustained contraction. It also reduces oxidative stress that accumulates during prolonged near work.
Real Results in Real Users
Multiple clinical trials show astaxanthin (6-12mg daily) improves:
- Visual fatigue scores after computer work (reduction of 30-50% in most studies)
- Accommodation amplitude (increased focusing range)
- Contrast sensitivity (ability to distinguish objects from background)
- Recovery time between near and far vision (faster refocusing)
- Subjective eye strain symptoms (less heaviness, discomfort)
A 2018 systematic review analyzed data from multiple astaxanthin studies involving over 300 participants. The consistent finding: people who spend more than four hours daily on digital devices benefit most. Effects typically appear after 4-12 weeks of consistent use.
Who Should Consider It
Computer workers, gamers, and anyone spending hours on screens see the clearest benefits. This isn’t about preventing blindness decades from now. It’s about feeling better today.
You’re a good candidate if you experience:
- Blurry vision when looking up from your screen
- Eyes that feel tired or heavy by afternoon
- Difficulty focusing after extended reading
- Headaches centered around or behind your eyes
- The need to blink hard or rub your eyes frequently
Natural Sources vs. Supplements
Unlike lutein and zeaxanthin, which you can get from eating greens, astaxanthin comes mainly from seafood—particularly wild salmon, shrimp, krill, and lobster. These animals get astaxanthin from eating algae.
To get 6mg from food, you’d need about 6 ounces of wild sockeye salmon daily. That’s not practical for most people. Farmed salmon contains far less astaxanthin because the fish don’t eat natural algae.
Supplements typically use astaxanthin extracted from Haematococcus pluvialis algae. This is the same source wild salmon get it from, just without the middleman fish.
Combining with Lutein and Zeaxanthin
These carotenoids work through different mechanisms and target different eye structures. Lutein and zeaxanthin protect the retina from light damage. Astaxanthin helps the focusing muscles work better.
You can safely take both. In fact, some newer “digital eye health” formulas combine all three. Just make sure you’re getting therapeutic doses of each:
- Lutein: at least 10mg
- Zeaxanthin: at least 2mg
- Astaxanthin: at least 6mg
Bottom line: If screen time leaves your eyes exhausted, astaxanthin directly addresses the problem. It’s not a retina protector—it’s a muscle supporter. Different problem, different solution.
Blue Light Blocking Glasses: Supplement Alternative or Complementary Tool?
You’ve seen them advertised everywhere. But do blue light blocking glasses actually work? And how do they compare to taking lutein and zeaxanthin?
What the Science Says
A 2017 systematic review examined evidence for blue light blocking glasses. The conclusion: minimal evidence for benefit. Most studies were small, poorly designed, or showed inconsistent results.
A 2021 Cochrane review analyzed data from six trials involving 156 participants. Blue light filtering lenses showed no significant benefit for reducing eye strain, improving sleep, or protecting macular health compared to clear lenses.
That doesn’t mean they’re useless—just that the evidence isn’t strong. Some people report subjective improvements in comfort, even if objective measurements don’t show differences.
How They Compare to Lutein and Zeaxanthin
Blue light glasses:
- Block some blue light before it enters your eye
- Work immediately (no waiting period)
- Cost $20-150 one-time
- No biological benefit beyond light filtering
- Don’t increase macular pigment density
- Can add visual distortion or color shift
- Must remember to wear them
Lutein and zeaxanthin supplements:
- Filter blue light at the retina level
- Take 6-12 months to reach full effect
- Cost $15-25 monthly ongoing
- Provide antioxidant protection
- Increase protective macular pigment
- No visual distortion
- Work 24/7 once levels build up
Can You Do Both?
Sure. They work through different mechanisms and don’t interfere with each other. But honestly, the better approach is:
The 20-20-20 rule: Every 20 minutes, look at something 20 feet away for 20 seconds. This gives your ciliary muscles a break. Studies show this simple habit reduces eye strain more effectively than blue light glasses.
Screen positioning: Keep screens 20-26 inches from your eyes, slightly below eye level. This reduces strain on focusing muscles and decreases tear evaporation.
Blink deliberately: People blink 66% less when using screens. Incomplete blinks are even more common. Make a conscious effort to blink completely every few seconds.
Adjust screen settings: Reduce blue light through software (Night Shift on Apple, Night Light on Windows) rather than buying special glasses. It’s free and adjustable.
If you work at a computer all day, invest in astaxanthin supplements rather than blue light glasses. The evidence is stronger, and you’re addressing the root cause—muscle fatigue—rather than just filtering light.
Bottom line: Blue light blocking glasses have weak evidence despite heavy marketing. Lutein, zeaxanthin, and astaxanthin have stronger evidence and work from the inside out. Good screen habits beat both.
4. Omega-3
Walk into any health store and you’ll find omega-3s promoted for eye health. The reality is more complicated.
The AMD Evidence Is Disappointing
AREDS2 tested omega-3 supplements in thousands of people at risk for AMD. The study design was rigorous: participants received 1g daily of EPA plus DHA or placebo, added to the AREDS formula. After five years, adding omega-3s to the AREDS formula provided no additional benefit. None.
That said, observational studies consistently show that people who eat fatty fish 2-3 times weekly have 30-40% lower AMD risk compared to people who rarely eat fish. The Blue Mountains Eye Study in Australia followed 2,895 people for five years and found that eating fish just once weekly reduced late AMD risk by 31%.
Why the disconnect? Several possibilities:
The form matters: Whole fish contains omega-3s in triglyceride form along with other nutrients (vitamin D, selenium, astaxanthin in wild salmon). Most supplements use ethyl ester form, which absorbs poorly.
The timing matters: You need decades of adequate omega-3 intake for AMD prevention, not just five years during AREDS2.
The dose might matter: Observational studies track total dietary omega-3s, which might exceed 1g daily in high fish consumers.
Understanding EPA vs. DHA
These are the two main omega-3 fatty acids. DHA concentrates heavily in the retina—it makes up about 60% of the fatty acids in photoreceptor outer segments. EPA doesn’t accumulate in the retina but has strong anti-inflammatory effects.
For eye health, DHA appears more important than EPA. A 2009 study in the American Journal of Clinical Nutrition found that women in the highest quintile of DHA intake had 38% reduced risk of AMD, while EPA showed no association.
When choosing supplements, look for:
- At least 500mg DHA per dose
- Re-esterified triglyceride (rTG) form for better absorption
- Third-party testing for mercury and PCBs (especially important with fish oil)
- Enteric coating to prevent fishy burps
The Dry Eye Story Is Mixed Too
The DREAM study, published in 2018 in the New England Journal of Medicine, tested omega-3s for dry eye disease. This large trial with 535 participants found that 3g daily of EPA/DHA worked no better than olive oil placebo over 12 months.

Critics argue the olive oil itself had beneficial anti-inflammatory effects, making the comparison unfair. The study also used people with relatively mild dry eye—maybe omega-3s help more severe cases.
Some earlier studies showed benefits. A 2013 trial found that 1g daily omega-3s improved tear osmolarity and reduced inflammatory markers in dry eye patients after three months. But results across studies remain inconsistent.
The Triglyceride Form Advantage
Not all omega-3 supplements are created equal. Fish oil naturally contains triglycerides, but processing often converts these to ethyl esters. Some manufacturers then re-convert to triglycerides.
A 2015 study compared absorption of different forms. The re-esterified triglyceride form showed 124% better bioavailability than ethyl ester form. That means you absorb more than twice as much.
Check your supplement label:
- “Triglyceride form” or “rTG form” = good
- “Ethyl ester” or no specification = poor absorption
- “Phospholipid form” (from krill) = also well absorbed but expensive
What About Vegetarian Sources?
If you don’t eat fish, algae-based DHA supplements work well. Algae is where fish get their omega-3s anyway. Studies show algae-based DHA raises blood levels of DHA just as effectively as fish oil.
Flaxseed and chia seeds contain ALA (alpha-linolenic acid), which your body converts to EPA and DHA. But conversion rates are low—typically under 10%. Don’t rely on plant sources alone for eye health.
Mercury Concerns: Real or Overblown?
Fish contains mercury, which accumulates in larger, longer-lived fish like shark, swordfish, and king mackerel. But smaller fish like salmon, sardines, and anchovies have minimal mercury.
High-quality fish oil supplements are molecularly distilled to remove mercury and other contaminants. Look for products that show third-party testing results for heavy metals. USP verification, NSF certification, or ConsumerLab approval all indicate the product has been tested.
For most people, the benefits of eating fish or taking fish oil far outweigh the minimal mercury risk, especially if choosing smaller fish or tested supplements.
The Practical Recommendation
For AMD prevention, skip the pills. Eat salmon, mackerel, sardines, or trout 2-3 times weekly. You’ll get omega-3s plus vitamin D, selenium, and other beneficial nutrients that supplements don’t provide.
For dry eye symptoms, you can try rTG omega-3 supplements (2-3g EPA/DHA daily) for three months. If you see no improvement, stop. The evidence is too mixed to justify indefinite supplementation.
Quick takeaway: Omega-3s from whole fish show strong observational evidence for AMD prevention. Supplements show disappointing results in clinical trials. For dry eye, they might help some people but certainly don’t help everyone.
5. Maqui Berry Extract
This might be the most interesting development in years for people with gritty, uncomfortable eyes.
Better Than Bilberry
Maqui berry comes from Chilean Patagonia. It contains powerful anthocyanins called delphinidins—compounds that support tear production through a different mechanism than artificial tears or omega-3s.
A 2014 study published in Panminerva Medica tested 60mg daily of standardized maqui berry extract (MaquiBright) in 13 dry eye patients. After 30 days, tear fluid production increased by 50% on average. By 60 days, the increase reached nearly 100% compared to baseline. The control group showed no change.
Head-to-head studies suggest maqui berry outperforms bilberry for dry eye symptoms. That matters because bilberry has dominated the supplement market for decades based on much weaker evidence.
How It Works Differently
Most dry eye treatments focus on reducing inflammation or supplementing the tear film. Maqui berry appears to stimulate the lacrimal glands to produce more tears naturally.
The delphinidins in maqui berry activate specific cellular pathways related to tear secretion. This addresses the root problem: inadequate tear production. It’s not about soothing symptoms temporarily—it’s about making more tears.
Who Benefits Most
If you have dry, scratchy eyes that feel worse by afternoon, this addresses your actual problem. You’re a good candidate if you experience:
- Gritty or sandy sensation in eyes
- Burning or stinging
- Eyes that feel worse in air conditioning or wind
- Intermittent blurry vision that improves with blinking
- Excessive tearing (paradoxical response to dryness)
- Contact lens discomfort
The typical dose in studies was 60mg of standardized extract daily. Look for products specifying MaquiBright or similar standardized forms with defined delphinidin content (usually 25-35%).
Timeline for Results
Unlike artificial tears, which work immediately, maqui berry takes time. Most studies show:
- Week 1-2: Minimal change
- Week 3-4: First noticeable improvements in tear production
- Week 6-8: Peak benefits for most people
- After 8 weeks: Effects plateau
If you see no improvement after 60 days, it’s probably not going to work for you. That’s the right time to reassess and try a different approach.
Combination with Other Treatments
You can use maqui berry alongside:
- Artificial tears (use less as natural tears increase)
- Omega-3 supplements (different mechanisms)
- Prescription dry eye medications
- Warm compresses for meibomian gland dysfunction
Don’t stop prescription treatments without asking your eye doctor. Think of maqui berry as an add-on that might eventually allow you to reduce other interventions.
Cost Considerations
Maqui berry supplements typically cost $25-40 monthly, making them pricier than basic omega-3s or lutein. The standardized extracts required for efficacy cost more to produce than generic berry powders.
Is it worth the cost? If omega-3s haven’t worked for your dry eyes, yes. The evidence is stronger and more consistent than for omega-3s in dry eye disease. For many people, increased comfort and reduced need for artificial tears justifies the expense.
Standardization Issues
Not all maqui berry products are equal. Generic “maqui berry powder” won’t deliver the same results as standardized extracts tested in clinical trials.
Look for:
- Standardized delphinidin content (usually expressed as percentage)
- MaquiBright or equivalent branded extract
- Capsules or tablets (powders degrade faster)
- 60mg daily dose of standardized extract
- Third-party testing certification
Bottom line: Maqui berry represents a genuinely new approach to dry eye. It doesn’t just reduce inflammation or supplement tears—it helps you make more of your own tears. If artificial tears and omega-3s haven’t solved your dry eye, this deserves a two-month trial.
The “Watch and Wait” List: Promising but Limited
Some supplements show real potential but need larger studies before we can make strong recommendations.
6. Saffron
Saffron is expensive—sometimes costing more than gold per ounce. But multiple small trials suggest it might improve visual function in early AMD.
A 2018 systematic review published in Nutrients analyzed eight studies involving 370 participants. Across these trials, saffron (20-30mg daily) consistently improved visual acuity, contrast sensitivity, and retinal function in people with early-to-moderate AMD over 3-12 months. The supplement also showed benefits in Stargardt disease, a rare genetic condition causing juvenile macular degeneration.

The Australian Saffron study, published in 2016, found that 20mg daily saffron improved macular function in participants with early AMD. After three months, electroretinogram measurements showed significant improvements in retinal response. Visual acuity also improved slightly but not enough to read better on an eye chart.
How Saffron Might Work
The active compounds are crocin and crocetin—carotenoids that provide saffron’s distinctive color. These compounds appear to:
- Protect photoreceptor cells from oxidative damage
- Reduce inflammation in the retina
- Improve blood flow to the macula
- Modulate genes involved in cell survival
The mechanism differs from lutein and zeaxanthin, which mainly filter light. Saffron appears to work at the cellular level.
The Limitation Problem
Here’s the catch: all saffron studies have been relatively small (20-60 participants each). Most come from Italian and Australian research groups. We need large-scale, independent trials to confirm these promising signals.
Also, not all saffron supplements contain adequate active compounds. Look for:
- Standardized extracts with defined crocin content
- Products specifying “saffron stigma” (not cheaper substitutes)
- Doses matching studied amounts (20-30mg daily)
- Reputable brands with third-party testing
At $30-50 monthly, saffron is pricey. But if you have early AMD and want to try something beyond AREDS2, saffron has the best safety profile of the experimental options. Just understand you’re taking a calculated risk on emerging evidence.
7. Alpha-Lipoic Acid
If you have diabetes, alpha-lipoic acid (ALA) deserves attention. This antioxidant is unique because it’s both water-soluble and fat-soluble, allowing it to work throughout your cells.
A four-year German study published in Diabetes Care in 2004 followed 73 people with diabetic macular edema. Those taking 600mg daily ALA showed significantly reduced progression compared to placebo. Retinal thickness measurements remained more stable in the ALA group.
Several other trials show that ALA (300-600mg daily) may:
- Slow diabetic retinopathy progression
- Improve retinal nerve fiber layer thickness
- Reduce oxidative stress markers in the eye
- Improve contrast sensitivity in diabetic patients
Why ALA Is Special
Alpha-lipoic acid regenerates other antioxidants after they neutralize free radicals. It recycles vitamins C and E, plus glutathione—your body’s master antioxidant. This amplifies the antioxidant capacity of your entire system.
The retina has high metabolic activity and generates lots of oxidative stress, especially with high blood sugar. ALA’s ability to work in both watery and fatty environments makes it particularly suited to protecting diverse eye tissues.
Who Should Consider ALA
If you have:
- Type 1 or type 2 diabetes
- Early signs of diabetic retinopathy
- Diabetic macular edema
- Pre-diabetes with family history of diabetic eye disease
Talk with your doctor about ALA. The evidence isn’t strong enough yet to call this a must-have, but for people with diabetic eye disease, it’s worth discussing. The typical dose studied is 300-600mg daily, taken with meals.
ALA can lower blood sugar, so monitor your glucose levels carefully if you try it alongside diabetes medications. Dosage adjustments might be needed.
Quick takeaway: Saffron and ALA show consistent positive signals in small studies. They’re worth considering for specific conditions—early AMD and diabetic eye disease—but understand you’re acting on promising rather than proven evidence.
Save Your Money on These: The Myth-Busting Section
Some supplements have great marketing but terrible evidence.
9. Bilberry
Remember those British pilots and their supposed carrot-based night vision? The bilberry story follows the same pattern. RAF pilots allegedly ate bilberry jam to see better at night. More propaganda.
A 2013 systematic review published in the Journal of Evidence-Based Complementary Medicine analyzed all available bilberry studies. The conclusion: disappointing results for vision improvement. Some small studies reported modest improvements in visual fatigue, but larger, better-designed trials failed to confirm benefits.
A specific study testing bilberry for night vision found no improvement in healthy volunteers. Participants took 12-36mg of anthocyanins (the active compounds in bilberry) for three weeks. Night vision measurements showed no difference from placebo.
Despite potent antioxidant properties in lab dishes, bilberry hasn’t lived up to its reputation in human eyes. Maqui berry has now surpassed it for dry eye symptoms. Lutein and zeaxanthin beat it for macular protection. There’s little reason to choose bilberry anymore, especially at premium prices.
10. Vitamin A
Competitors love listing vitamin A as a top eye supplement. Here’s the truth: unless you’re severely malnourished, you don’t need it.
Vitamin A deficiency causes night blindness, dry eyes, and eventually corneal damage. But in developed countries, deficiency is extremely rare. The National Health and Nutrition Examination Survey found that less than 1% of Americans have vitamin A deficiency.
Taking high doses of preformed vitamin A (retinol) is toxic. Chronic intake above 10,000 IU daily can cause:
- Liver damage
- Bone fractures
- Birth defects if pregnant
- Intracranial pressure (pseudotumor cerebri)
- Dry, itchy skin
Your body converts beta-carotene from vegetables into vitamin A as needed. That’s the safe way to get it. You can’t overdose on beta-carotene from food—your body simply stops converting it when stores are adequate.
The only exception: people with rare genetic variants affecting beta-carotene conversion might need preformed vitamin A. But this affects less than 5% of the population and requires genetic testing to identify.
Isolated vitamin A supplements for eye health? Skip them. You’re either already getting enough or you have a medical condition requiring doctor supervision.
11. Ginkgo Biloba
Ginkgo biloba has been studied for multiple eye conditions, particularly glaucoma. The results are all over the map.
Some small trials report improved ocular blood flow in normal-tension glaucoma. A 2013 study found improved visual field measurements after six months of ginkgo supplementation. But other studies show no benefit, and a 2020 systematic review concluded the evidence was too inconsistent to recommend it.
More concerning: ginkgo interacts with blood thinners and may increase bleeding risk. If you take warfarin, clopidogrel, or even aspirin regularly, ginkgo can potentiate their effects. Several case reports describe serious bleeding events—including eye hemorrhages—in people combining ginkgo with anticoagulants.
Given the inconsistent benefits and real risks, ginkgo doesn’t make the cut for eye health recommendations.
12. CoQ10
Coenzyme Q10 supports cellular energy production. Since retinal cells have high energy demands, CoQ10 supplementation makes theoretical sense.
Small trials suggest CoQ10 (100-400mg daily) might protect retinal ganglion cells in glaucoma. A 2017 study found reduced intraocular pressure and improved visual function in glaucoma patients taking 300mg daily CoQ10 for 12 months.
Topical CoQ10 combined with vitamin E shows more promise than oral supplements. A 2019 study using topical CoQ10 eye drops found improved symptoms and corneal health in dry eye patients.
But large-scale trials are lacking. The studies we have involve small sample sizes and short durations. For now, this remains experimental. If you have glaucoma, discuss CoQ10 with your ophthalmologist, but don’t start it on your own as a replacement for proven treatments.
Why These Supplements Persist Despite Weak Evidence
Marketing drives sales more than science. Bilberry has the World War II story. Vitamin A has decades of “carrots for night vision” cultural momentum. Ginkgo benefits from being a traditional Chinese medicine. CoQ10 rides the wave of general energy and aging concerns.
Supplement companies aren’t required to prove efficacy before selling products. They just need to avoid making specific disease claims. This creates a market flooded with supplements that sound science-based but lack clinical proof.
When evaluating any eye supplement, ask:
- Are there multiple large RCTs showing benefit?
- Do the studies measure actual vision outcomes or just lab markers?
- Has the research been replicated by independent groups?
- Does the benefit outweigh potential risks and costs?
Most products fail these tests. The supplements in our “top tier” pass them. That’s the difference between evidence-based recommendations and marketing hype.
Quick takeaway: Just because a supplement is popular doesn’t mean it works. Bilberry, isolated vitamin A, ginkgo, and CoQ10 all have weak or inconsistent evidence for eye health. Save your money for supplements with proven benefits.
How Long Until You See Results? Setting Realistic Expectations
One of the biggest reasons people quit supplements is unrealistic expectations. Here’s what to actually expect and when.
Week 1-4: The Invisible Phase
For most eye supplements, you’ll notice nothing during the first month. This doesn’t mean they’re not working—it means you’re building up tissue levels of nutrients.
Lutein and zeaxanthin: These accumulate slowly in your macula. Blood levels peak within a few days, but macular levels take months to plateau.
AREDS formula: Working at the cellular level to slow oxidative damage you can’t feel.
Omega-3s: Building into cell membranes throughout your body, including eye tissues.
Astaxanthin: Beginning to accumulate in ciliary muscles and reduce inflammation.
Maqui berry: Starting to influence tear gland function, but production increases take time.
Saffron: Early cellular changes happening that won’t show up in vision yet.
Don’t give up during this phase. The lack of immediate results frustrates people, but that’s how prevention works. You’re investing in future eye health, not fixing acute problems.
Month 2-3: First Noticeable Changes
This is when some supplements start showing subjective benefits.
Astaxanthin: Many people notice less eye fatigue after work by week 6-8. Eyes feel “fresher” at the end of the day. Focusing between near and far tasks becomes easier.
Maqui berry: Dry eye symptoms begin improving around week 4-6. You might use artificial tears less frequently. The gritty sensation decreases.
Lutein and zeaxanthin: Subtle improvements in night driving or glare recovery might appear. Most people don’t notice dramatic changes yet, but objective measurements would show increased MPOD.
Omega-3s (if they work for you): Dry eye comfort might improve slightly. Tear quality changes before tear quantity increases.
This phase is critical. You’re starting to see benefits, which motivates continued use. Track your symptoms weekly to notice gradual improvements that might otherwise go unrecognized.
Month 6-12: Full Benefits Emerge
Maximum effects typically require 6-12 months of consistent supplementation.
Lutein and zeaxanthin: MPOD reaches plateau. Visual function improvements peak. Contrast sensitivity and glare recovery maximize. Long-term protective effects are established.
AREDS formula: In people with AMD, this is when progression rates diverge most clearly from non-supplementers. You can’t “feel” this, but ophthalmologist measurements show slower disease advancement.
Astaxanthin: Full improvement in accommodation and reduced fatigue. Ciliary muscle function optimizes.
Saffron: Studies showing vision improvements typically measured outcomes at 3-12 months. Earlier changes are minimal.
A 2013 study tracking lutein supplementation used MPOD measurements at baseline, 3 months, 6 months, and 12 months. MPOD increased linearly through 6 months, then plateaued. Functional vision improvements paralleled MPOD increases but lagged slightly behind.
Why Patience Matters with Supplements
Unlike medications that produce immediate effects, nutritional supplements work by:
Building tissue stores: Your body must accumulate nutrients in target tissues. This takes time.
Cellular-level changes: Reducing oxidative damage, improving mitochondrial function, and decreasing inflammation happen gradually.
Structural improvements: Increasing macular pigment density or improving meibomian gland function requires weeks to months.
Think of supplements like exercise. You don’t get fit from one workout. Consistent daily action over months produces results. Same principle applies to eye nutrients.
When to Reassess
Give supplements an adequate trial before deciding they don’t work:
- Astaxanthin: 12 weeks minimum
- Maqui berry: 60 days minimum
- Lutein/zeaxanthin: 6 months for subjective benefits, 12 months for full effect
- Omega-3s: 3 months minimum
- Saffron: 3-6 months
- AREDS formula: Must continue indefinitely; benefits only persist with ongoing use
If you see no improvement after an adequate trial, the supplement either doesn’t work for your particular situation, or the condition you’re trying to address doesn’t respond to that supplement.
Condition-Specific Timelines
Slowing AMD progression (AREDS2): Benefits accumulate over years. You won’t notice slower progression—your doctor will document it through exams. This requires indefinite continuation.
Preventing AMD (lutein/zeaxanthin): A 20-30 year investment. You’re reducing risk decades from now. Impossible to know if it “worked” for you individually, but population studies show clear benefits.
Reducing eye strain (astaxanthin): 4-12 weeks for noticeable improvement. If your eyes still feel exhausted after work by week 12, it’s not working.
Improving dry eye (maqui berry, omega-3s): 30-90 days for meaningful improvement. If symptoms haven’t improved by day 90, try something else.
Early AMD vision support (saffron): 3-12 months. Requires objective measurements (visual acuity tests, contrast sensitivity) to detect small improvements.
Bottom line: Supplements require patience. Expect nothing for the first month. Look for subtle improvements by month 2-3. Give most supplements 3-6 months before deciding they don’t work. Prevention benefits accumulate over years or decades.
Reading Supplement Labels: Red Flags and Green Flags
The supplement aisle is full of misleading labels. Here’s how to evaluate products and avoid wasting money.
Red Flags That Should Make You Walk Away
“Proprietary blend”: This means the manufacturer lists a group of ingredients with a total weight but doesn’t tell you how much of each ingredient is included. They could include 99% cheap filler and 1% active ingredient.
Example label:
“Eye Health Blend (500mg): Lutein, Zeaxanthin, Bilberry, Grape Seed Extract, Turmeric”
You have no idea if this contains 10mg lutein or 0.5mg. Skip these products entirely.
Insufficient dosing: Many “eye health” supplements contain far less than effective doses studied in clinical trials.
Real example from a major brand:
“Lutein: 250mcg”
That’s 0.25mg—40 times less than the 10mg dose proven effective. You’d need to take 40 pills daily to get a therapeutic dose. This is intentional—it lets them put lutein on the label while keeping costs low.
Multiple unrelated ingredients: Some products throw in 20+ ingredients at minimal doses. The thinking: if one ingredient becomes popular, they can market that feature.
Example:
“Contains lutein, zeaxanthin, bilberry, ginkgo, CoQ10, vitamin A, vitamin C, vitamin E, zinc, copper, selenium, alpha-lipoic acid, taurine, quercetin, resveratrol, beta-carotene, lycopene, astaxanthin…”
Each ingredient is probably underdosed. You’re paying for a little bit of everything rather than effective amounts of anything.
Vague language: Watch for terms like “supports,” “promotes,” or “maintains” without specific claims. These are legal weasel words that imply benefits without promising them.
Celebrity endorsements: If the main selling point is a famous person’s name rather than clinical evidence, walk away.
“Clinically proven” without specifics: This phrase is meaningless without citing actual studies. Proven for what? In whom? Over what timeframe?
Green Flags That Indicate Quality
Specific ingredient amounts: Every active ingredient should list its exact dose in mg or mcg.
Good example:
“Lutein (from marigold extract): 10mg
Zeaxanthin: 2mg
Vitamin C: 500mg”
You can compare this directly to studied doses.
USP verification: The U.S. Pharmacopeia is an independent testing organization. USP-verified supplements have been tested for:
- Ingredient accuracy (contains what the label claims)
- Purity (free from harmful contaminants)
- Dissolution (breaks down properly for absorption)
- Manufacturing quality
Look for the USP seal on the label.
Third-party testing: NSF International and ConsumerLab also provide independent verification. These organizations test products randomly and publish results.
Standardized extracts: For herbal supplements like maqui berry or saffron, look for standardization to specific active compounds.
Good example:
“Maqui Berry Extract (standardized to 25% delphinidins): 60mg”
This ensures consistent potency batch to batch.
Form matters for some nutrients: Labels should specify the chemical form of minerals and vitamins.
For zinc: “Zinc (as zinc oxide)” matches AREDS2 studies
For omega-3s: “Re-esterified triglyceride form” absorbs better than ethyl ester
Expiration dates: Quality supplements include expiration or “best by” dates. Nutrients degrade over time.
Contact information: Reputable companies provide phone numbers, email addresses, and physical addresses for questions or concerns.
How to Compare Products
When choosing between brands, create a simple comparison:
| Brand A | Brand B | Studied Dose | |
|---|---|---|---|
| Lutein | 5mg | 10mg | 10mg |
| Zeaxanthin | 1mg | 2mg | 2mg |
| Cost | $15/month | $20/month | — |
| Testing | No third-party testing | USP verified | — |
Brand B costs more but delivers effective doses with quality assurance. Brand A is cheaper but underdosed—you’d need to double or triple the serving size, making it more expensive and less convenient.
Store Brand vs. Name Brand
Generic store brands often match name brands for a fraction of the price—if they contain the same ingredients at the same doses. Compare labels carefully.
Major pharmacy chains (CVS, Walgreens, Costco) often produce quality store-brand supplements. Check for:
- Exact dose matching of proven formulas
- Similar or identical ingredient forms
- Third-party testing when possible
Save the extra $10-15 monthly on name-brand marketing and put it toward higher-quality whole foods.
What About “Preservative-Free” and “All-Natural”?
These marketing terms don’t indicate higher quality or efficacy.
“Natural”: Arsenic is natural. Snake venom is natural. Natural doesn’t mean safe or effective.
“Preservative-free”: Some supplements need preservatives to prevent bacterial growth or oxidation. Without them, products might degrade faster.
Focus on evidence, not marketing feelings. Would you rather have an all-natural supplement with 1mg of lutein or a “synthetic” one with the 10mg proven to work? The dose matters more than the origin.
Bottom line: Read ingredient amounts, not marketing claims. Verify doses match clinical studies. Look for third-party testing. Avoid proprietary blends and underdosed products. Generic brands often work just as well as expensive name brands if the formulation matches.
The Genetic Factor: Why Some People Need Supplements More
Your genes influence how well you absorb, transport, and use nutrients. This explains why some people benefit more from supplements than others.
CFH Gene Variants and AMD Risk
The complement factor H (CFH) gene regulates inflammation in your immune system. Certain variants dramatically increase AMD risk.
People with two copies of the high-risk Y402H variant have 5-7 times higher AMD risk than people with low-risk versions. About 50% of AMD cases involve CFH gene variants.
A 2013 study published in Ophthalmology examined whether genetics influenced AREDS supplement response. The findings were striking: people with high-risk CFH variants benefited more from zinc supplementation than those with low-risk variants. The genetic makeup determined who responded best.
This suggests personalized supplementation based on genetics might optimize outcomes. Someone with high-risk CFH variants might need earlier and more aggressive supplementation.
APOE4 and Nutrient Metabolism
The APOE gene helps regulate cholesterol and fat metabolism. The APOE4 variant increases Alzheimer’s risk but also affects how your body handles fat-soluble nutrients like lutein and zeaxanthin.
Research shows APOE4 carriers might need higher doses of these carotenoids to achieve the same macular pigment density as non-carriers. Their bodies appear to transport or metabolize these nutrients differently.
If you carry APOE4 and have family history of AMD, you might benefit from higher lutein doses (15-20mg vs. standard 10mg).
BCO1 Gene and Carotenoid Conversion
The BCO1 gene controls how efficiently you convert beta-carotene to vitamin A. About 45% of people carry variants that reduce conversion efficiency by up to 69%.
For these individuals:
- Eating carrots and sweet potatoes produces less vitamin A
- They might need more dietary vitamin A from animal sources
- Beta-carotene supplements work poorly
But this doesn’t affect lutein and zeaxanthin, which your body doesn’t convert to vitamin A. People with BCO1 variants still absorb and use these carotenoids normally for eye health.
Why Family History Matters More Than You Think
If your parents or siblings developed AMD, your risk increases 3-6 fold compared to people with no family history. This isn’t just about CFH—dozens of genes contribute to AMD risk.
Strong family history should trigger earlier supplementation conversations with your eye doctor. Don’t wait for symptoms. Start protective supplementation with lutein and zeaxanthin in your 40s or 50s rather than waiting until AMD develops.
Genetic Testing: Is It Worth It?
Several companies offer genetic testing for AMD risk genes. Costs range from $150-400. You submit a saliva sample, and they test for CFH, ARMS2, and other AMD-related variants.
Potential benefits:
- Identifies high-risk individuals who need earlier screening
- Might guide supplement choices (higher zinc for CFH variants)
- Motivates lifestyle changes when you see concrete risk numbers
Limitations:
- Testing only identifies risk, not destiny. You might have high-risk genes but never develop AMD
- Doesn’t change the basic recommendation (comprehensive eye exams, lutein/zeaxanthin)
- Insurance rarely covers testing for this purpose
- Results might cause anxiety without changing management much
For most people, genetic testing isn’t necessary. If you have multiple family members with AMD, especially early-onset cases, testing might provide useful information. Discuss with your ophthalmologist.
Nutrigenomics: The Future of Personalized Supplements
Research is moving toward personalized supplement recommendations based on your genetic profile. Imagine getting a report that says:
“Based on your CFH rs1061170 CT genotype, we recommend:
- Zinc: 40mg daily (you’re a strong zinc responder)
- Lutein: 15mg daily (you need higher doses for adequate MPOD)
- Omega-3s: Standard benefit (no genetic variants affecting response)”
We’re not quite there yet, but studies are actively investigating these approaches. Within the next decade, genetic-guided supplementation might become standard care for AMD prevention.
What You Can Do Now
Even without genetic testing, you can act on family history:
Strong AMD family history (parent or sibling affected):
- Start lutein/zeaxanthin supplementation by age 45-50
- Get comprehensive dilated eye exams every 1-2 years starting at 40
- Consider genetic counseling if multiple family members affected young
- Avoid smoking absolutely—it multiplies genetic risk
No family history but other risk factors (smoking, light eyes, high sun exposure):
- Consider lutein/zeaxanthin supplementation by age 55-60
- Regular eye exams every 2 years after age 60
- Prioritize lifestyle factors (diet, smoking cessation, UV protection)
No risk factors:
- Food-first approach with leafy greens 4-5 times weekly
- Consider supplements if diet is inadequate
- Routine eye exams as recommended by your doctor
Bottom line: Genetics influences who benefits most from supplements. Strong family history of AMD warrants earlier and more aggressive supplementation. Genetic testing remains optional but might guide personalized approaches in the future.
👁️ Eye Health Supplement Selector Quiz
Answer 12 questions to get your personalized supplement protocol
7-Day Sample Meal Plan for Eye Health
Can you eat your way to 10mg lutein daily? Absolutely. Here’s how.
Day 1: The Kale Power Day
Breakfast: Spinach and mushroom omelet (2 eggs + 1 cup raw spinach)
- Lutein: 3.7mg | Zeaxanthin: 0.1mg
Lunch: Kale and white bean soup (1.5 cups cooked kale)
- Lutein: 17.8mg | Zeaxanthin: 0.4mg
Snack: Orange bell pepper strips with hummus (1 cup raw)
- Lutein: 0.3mg | Zeaxanthin: 2.8mg
Dinner: Grilled chicken with roasted Brussels sprouts (1 cup)
- Lutein: 1.9mg | Zeaxanthin: 0.1mg
Daily Total: Lutein: 23.7mg | Zeaxanthin: 3.4mg
Day 2: The Egg and Greens Day
Breakfast: Two-egg breakfast with sautéed collard greens (1 cup cooked)
- Lutein: 14.9mg | Zeaxanthin: 0.6mg
Lunch: Mixed green salad with romaine, spinach, and corn (2 cups greens + 0.5 cup corn)
- Lutein: 5.2mg | Zeaxanthin: 0.8mg
Snack: Hard-boiled eggs (2)
- Lutein: 0.3mg | Zeaxanthin: 0.2mg
Dinner: Baked salmon with Swiss chard (1 cup cooked)
- Lutein: 10.0mg | Zeaxanthin: 0.2mg
Daily Total: Lutein: 30.4mg | Zeaxanthin: 1.8mg
Day 3: The Squash and Greens Day
Breakfast: Scrambled eggs with zucchini (2 eggs + 1 cup cooked zucchini)
- Lutein: 2.8mg | Zeaxanthin: 0.5mg
Lunch: Butternut squash soup with side spinach salad (1 cup squash + 2 cups raw spinach)
- Lutein: 9.3mg | Zeaxanthin: 0.3mg
Snack: Corn on the cob (1 medium ear)
- Lutein: 1.4mg | Zeaxanthin: 1.0mg
Dinner: Stir-fried bok choy with tofu (2 cups bok choy)
- Lutein: 3.6mg | Zeaxanthin: 0.1mg
Daily Total: Lutein: 17.1mg | Zeaxanthin: 1.9mg
Day 4: The Turnip and Pepper Day
Breakfast: Vegetable frittata with peppers (2 eggs + 1 cup mixed peppers)
- Lutein: 0.6mg | Zeaxanthin: 2.5mg
Lunch: Turnip green salad with chickpeas (2 cups cooked turnip greens)
- Lutein: 24.4mg | Zeaxanthin: 0.4mg
Snack: Avocado with peas (0.5 avocado + 0.5 cup peas)
- Lutein: 2.1mg | Zeaxanthin: 0.1mg
Dinner: Grilled fish with asparagus (1 cup asparagus)
- Lutein: 2.5mg | Zeaxanthin: 0.1mg
Daily Total: Lutein: 29.6mg | Zeaxanthin: 3.1mg
Day 5: The Broccoli and Greens Day
Breakfast: Broccoli and cheese omelet (2 eggs + 1 cup broccoli)
- Lutein: 2.0mg | Zeaxanthin: 0.2mg
Lunch: Arugula and spinach salad with walnuts (3 cups mixed greens)
- Lutein: 7.5mg | Zeaxanthin: 0.2mg
Snack: Pistachios (1 ounce)
- Lutein: 0.3mg | Zeaxanthin: 0.05mg
Dinner: Pork chop with collard greens and sweet potato (1 cup collards + 1 medium sweet potato)
- Lutein: 15.7mg | Zeaxanthin: 0.5mg
Daily Total: Lutein: 25.5mg | Zeaxanthin: 0.95mg
Day 6: The Radicchio and Chard Day
Breakfast: Egg scramble with radicchio (2 eggs + 1 cup radicchio)
- Lutein: 0.7mg | Zeaxanthin: 0.3mg
Lunch: Swiss chard and lentil soup (2 cups cooked chard)
- Lutein: 20.0mg | Zeaxanthin: 0.4mg
Snack: Yellow corn tortilla chips with guacamole (1 ounce chips)
- Lutein: 0.5mg | Zeaxanthin: 0.6mg
Dinner: Grilled shrimp with green beans and yellow squash (1 cup each)
- Lutein: 2.3mg | Zeaxanthin: 0.4mg
Daily Total: Lutein: 23.5mg | Zeaxanthin: 1.7mg
Day 7: The Spinach Power Day
Breakfast: Spinach smoothie (2 cups raw spinach + banana + yogurt)
- Lutein: 7.0mg | Zeaxanthin: 0.2mg
Lunch: Spinach and artichoke stuffed chicken (1.5 cups cooked spinach)
- Lutein: 30.6mg | Zeaxanthin: 0.5mg
Snack: Orange slices with pistachios (1 orange + 1 ounce nuts)
- Lutein: 0.4mg | Zeaxanthin: 0.1mg
Dinner: Romaine lettuce wraps with ground turkey and corn salsa (2 cups romaine + 0.5 cup corn)
- Lutein: 3.9mg | Zeaxanthin: 0.8mg
Daily Total: Lutein: 41.9mg | Zeaxanthin: 1.6mg
Key Takeaways from the Meal Plan
Hitting the lutein target (10mg) through food is achievable with one serving of cooked leafy greens daily. Kale, spinach, collard greens, and turnip greens are your best sources.
Zeaxanthin is harder to get from food alone. Orange peppers, corn, and egg yolks help, but reaching 2mg daily requires deliberate food choices. This is where supplementation often makes practical sense.
Cooking increases bioavailability. Cooked greens provide more absorbable lutein than raw greens of equal weight. The cooking process breaks down cell walls, releasing carotenoids.
Add fat for absorption. Lutein and zeaxanthin are fat-soluble. Include olive oil, avocado, nuts, or eggs in meals with greens to maximize absorption.
Eggs punch above their weight. They contain relatively little lutein and zeaxanthin by amount, but the bioavailability is 3-4 times higher than from vegetables. Two eggs provide lutein equivalent to a much larger amount from plants.
Vegetarian Modifications
The meal plan already leans vegetarian. Simple swaps:
- Replace chicken or fish with tempeh, tofu, or legumes
- Ensure adequate fat sources (nuts, seeds, avocado, olive oil) with meals
- Consider algae-based omega-3 supplements for DHA
Omnivore Enhancements
Add more eggs and fatty fish:
- Wild salmon 2-3 times weekly (provides astaxanthin bonus)
- Egg-based breakfasts 4-5 times weekly (improves carotenoid absorption)
- Sardines or mackerel for omega-3s
When Supplements Make More Sense
Even with this meal plan, you might prefer supplements if you:
- Don’t enjoy leafy greens enough to eat them daily
- Have digestive issues (IBS, Crohn’s) limiting vegetable intake
- Travel frequently and can’t control food choices
- Want consistent, measurable daily doses
- Struggle with the zeaxanthin target (2mg is tough from food)
There’s no shame in choosing supplements. They provide reliable doses without requiring perfect dietary planning. Many people combine approach: eat greens when convenient, supplement on days they don’t.
Bottom line: You can absolutely get 10mg+ lutein daily from food with deliberate planning. Zeaxanthin is harder to achieve from food alone. Most people benefit from combining good dietary habits with targeted supplementation to ensure consistent intake.
Your Personalized Eye Health Protocol: Decision Tree
Different eyes need different supplements. Here’s how to find your protocol based on your specific situation.
| Your Situation | Recommended Supplements | Why These Work | Monthly Cost |
|---|---|---|---|
| Diagnosed intermediate/advanced AMD | AREDS2 formula | Only supplement proven to slow AMD progression in clinical trials | $20-35 |
| Healthy eyes, age 40-60, low vegetable intake | Lutein 10mg + Zeaxanthin 2mg | Builds macular pigment for long-term protection; 26% reduced late AMD risk in studies | $15-25 |
| Healthy eyes, excellent diet | Food-first approach; consider testing MPOD | You’re likely getting adequate lutein; supplement only if MPOD testing shows deficiency | $0-10 |
| Computer work 6+ hours daily | Astaxanthin 6-12mg + Lutein/Zeaxanthin | Astaxanthin supports ciliary muscle function; lutein protects retina from blue light | $35-55 |
| Dry, gritty eyes | Maqui berry 60mg standardized extract | Increases natural tear production in 30-60 days; outperforms omega-3s in recent studies | $25-40 |
| Dry eyes unresponsive to maqui berry | Omega-3 rTG form 2-3g EPA/DHA | Alternative mechanism for tear film improvement; try if maqui berry doesn’t help | $25-35 |
| Early AMD (small drusen) | Lutein 10mg + Zeaxanthin 2mg, consider adding Saffron 20-30mg | Lutein/zeaxanthin have strong prevention evidence; saffron experimental but promising | $45-75 |
| Type 1 or Type 2 diabetes | Alpha-lipoic acid 300-600mg + Lutein/Zeaxanthin | ALA shows specific benefits for diabetic retinopathy; lutein for general protection | $35-50 |
| Strong AMD family history (parent/sibling) | Start Lutein/Zeaxanthin by age 45 | Genetic risk 3-6x higher; earlier supplementation provides longer protection period | $15-25 |
| Smoker or former smoker | Lutein/Zeaxanthin ONLY (no beta-carotene) | Beta-carotene increases lung cancer risk 18%; modern AREDS2 formula safe for smokers | $15-25 |
| Light eye color + high sun exposure | Lutein/Zeaxanthin + strict UV protection | Light eyes have less melanin protection; supplement + sunglasses provide dual defense | $15-25 |
| Normal-tension glaucoma | Discuss with doctor; evidence for specific supplements weak/mixed | Ginkgo has inconsistent evidence; CoQ10 promising but needs more research; don’t self-treat | Varies |
How to Start Your Protocol
Step 1: Get a comprehensive dilated eye exam. Your eye doctor needs to check for:
- Early signs of AMD (drusen count and size)
- Diabetic retinopathy changes
- Glaucoma indicators
- Dry eye severity
- General retinal health
Don’t start supplements based on symptoms alone. Get objective measurements.
Step 2: Discuss supplement plans with your doctor. Bring this article or notes about which supplements you’re considering. Ask:
- Do I have early AMD that would benefit from AREDS2 or lutein/zeaxanthin?
- Are there drug interactions with my current medications?
- Should I get baseline MPOD testing?
- How often should I return for progress monitoring?
Step 3: Start with one supplement change at a time. Don’t start five new supplements simultaneously. If you develop side effects, you won’t know which one caused them.
Suggested order:
- Week 1-2: Start lutein/zeaxanthin (nearly everyone benefits)
- Week 3-4: Add astaxanthin if you have screen-related eye strain
- Week 5-6: Add maqui berry if you have dry eye symptoms
- Reassess after 90 days
Step 4: Track your symptoms and results. Create a simple log:
- Date started each supplement
- Symptoms you’re addressing
- Weekly check-ins on improvement (scale of 1-10)
- Any side effects
- Cost tracking
This helps you identify what’s working and what’s wasting money.
Step 5: Establish a long-term plan. Most eye supplements work through prevention and require indefinite continuation. After your initial trial period:
- Continue supplements showing clear benefit
- Discontinue those showing no benefit after adequate trial
- Schedule follow-up eye exams every 1-2 years to track objective changes
- Adjust protocol based on exam findings and new research
Special Considerations by Age
Ages 40-50: Focus on prevention. Lutein and zeaxanthin if family history or risk factors. Otherwise, food-first approach.
Ages 50-60: Start lutein/zeaxanthin supplementation even without symptoms. AMD risk increases significantly after 50. Add astaxanthin if heavy screen use.
Ages 60-70: Comprehensive eye exams every 1-2 years. If AMD develops, switch to AREDS2 formula immediately. Continue lutein/zeaxanthin if eyes remain healthy.
Ages 70+: AREDS2 if AMD present. Lutein/zeaxanthin for prevention if no AMD. Address dry eye aggressively—it worsens with age.
Supplement Timing and Absorption
Take with meals containing fat: Lutein, zeaxanthin, astaxanthin, and vitamins A, D, E, K all need dietary fat for absorption. Take them with breakfast or lunch that includes:
- Eggs
- Avocado
- Nuts or nut butter
- Olive oil
- Fatty fish
Morning vs. evening: Most eye supplements work equally well regardless of timing. Choose based on convenience and meal patterns. Consistency matters more than timing.
Spacing from other supplements: Zinc and calcium can interfere with each other’s absorption. If taking both, separate by 2-3 hours.
With or without food:
- AREDS formula: With food (reduces stomach upset from zinc)
- Lutein/Zeaxanthin: With fatty food (improves absorption)
- Astaxanthin: With fatty food (improves absorption)
- Omega-3s: With food (reduces fishy burps, improves absorption)
- Maqui berry: With or without food (water-soluble anthocyanins)
- Alpha-lipoic acid: Empty stomach or with food both work
What to Avoid Combining
Don’t combine:
- High-dose beta-carotene with lutein/zeaxanthin (competition for absorption)
- Ginkgo with blood thinners (bleeding risk)
- High-dose vitamin E (over 400 IU) without medical reason (mortality concerns)
- Multiple zinc sources totaling over 40mg daily (toxicity risk)
Safe combinations:
- Lutein + zeaxanthin + astaxanthin (different mechanisms, different targets)
- AREDS2 formula + maqui berry (no interactions)
- Omega-3s + lutein/zeaxanthin (may be synergistic)
- Alpha-lipoic acid + other antioxidants (regenerates them)
Supplement Myths We Need to Retire
Misinformation about supplements persists despite contrary evidence. Let’s address the most common myths.
Myth 1: “Natural is Always Safer”
The Reality: Natural doesn’t equal safe. Beta-carotene is natural but increases lung cancer risk in smokers. Arsenic is natural. Poison ivy is natural.
The AREDS study used natural beta-carotene, and it still caused problems. The solution was switching to lutein and zeaxanthin—also natural compounds, but safer ones.
What matters is evidence of safety and efficacy, not whether something comes from nature or a lab.
Myth 2: “More is Better”
The Reality: Nutrients have optimal dose ranges. Beyond these ranges, you get no additional benefit and might cause harm.
Examples:
- Zinc over 40mg daily can cause copper deficiency and immune suppression
- Vitamin E over 400 IU daily might increase mortality risk
- Vitamin A over 10,000 IU daily causes toxicity
The AREDS2 study specifically tested whether more zinc was better. It wasn’t. The 25mg dose worked just as well as 80mg with fewer side effects.
Take the dose supported by evidence, not the maximum your bottle allows.
Myth 3: “Supplements Can Reverse Damage”
The Reality: Supplements slow progression of existing disease or help prevent future disease. They don’t reverse damage already done.
The AREDS formula reduces AMD progression by 25%. It doesn’t restore vision you’ve already lost. Lutein and zeaxanthin build macular pigment for future protection—they don’t fix current problems.
Think of supplements like sunscreen. Sunscreen prevents future sun damage but doesn’t erase existing wrinkles or sunspots. Same principle.
Myth 4: “You Can Feel Them Working Immediately”
The Reality: Most eye supplements require weeks to months to show effects. The lack of immediate results doesn’t mean they’re not working.
Exception: astaxanthin for eye strain might show benefits in 4-12 weeks. But lutein, zeaxanthin, AREDS formula, and omega-3s take months to accumulate in tissues and produce measurable effects.
Impatience causes people to quit before supplements have a chance to work. Give them adequate time.
Myth 5: “Eye Vitamins Prevent Needing Glasses”
The Reality: Supplements address disease and dysfunction. They don’t fix refractive errors like nearsightedness, farsightedness, or astigmatism.
These conditions result from eyeball shape, not nutritional deficiency. No supplement changes the physical structure of your eye.
Glasses correct how light focuses. Supplements protect tissues from disease. Completely different issues.
Myth 6: “If It Works for AMD, It Works for Glaucoma and Cataracts”
The Reality: Different eye conditions have different causes and require different treatments. AMD involves retinal pigment epithelium and photoreceptor damage. Glaucoma involves optic nerve damage. Cataracts involve lens protein changes.
The AREDS formula works for AMD but shows no benefit for cataracts or glaucoma. Lutein might reduce cataract risk slightly, but evidence is weak. Astaxanthin doesn’t help AMD but does help eye strain.
Match the supplement to the condition backed by evidence.
Myth 7: “Expensive Supplements Are Better Quality”
The Reality: Price often reflects marketing and packaging, not quality. Many expensive brands are made in the same facilities as cheap store brands.
What matters:
- Ingredient amounts matching clinical studies
- Third-party testing verification
- Appropriate chemical forms (zinc oxide, rTG omega-3s)
- Proper storage and expiration dates
A $40 bottle of underdosed ingredients is worse than a $15 bottle of properly dosed generics.
Myth 8: “Taking Them Occasionally is Better Than Nothing”
The Reality: Eye supplements require consistent daily intake to build and maintain tissue levels. Taking lutein twice weekly won’t increase macular pigment density. Skipping the AREDS formula on weekends undermines its protective effects.
It’s like taking blood pressure medication occasionally and expecting your blood pressure to stay controlled. Doesn’t work that way.
If cost is an issue, take a lower-cost effective supplement daily rather than an expensive one inconsistently.
Myth 9: “If My Diet is Healthy, I Don’t Need Supplements”
The Reality: This depends on what “healthy” means. If you eat cooked leafy greens daily, fatty fish 2-3 times weekly, and colorful vegetables at every meal, you might get adequate eye nutrients from food.
But most people don’t. National surveys show:
- Average American eats greens less than once daily
- Most people get under 2mg lutein daily from food (need 10mg for benefits)
- Average zeaxanthin intake is under 0.5mg (need 2mg)
Unless your diet consistently includes the foods in our meal plan section, supplements fill real gaps.
Myth 10: “The Studies Are All Funded by Supplement Companies”
The Reality: The gold-standard studies—AREDS and AREDS2—were funded by the National Eye Institute, part of the National Institutes of Health. This is government-funded research, not industry-sponsored marketing.
The studies were designed to find truth, not sell products. When AREDS2 found that omega-3s provided no benefit, they published that finding. When they found that lower zinc doses worked as well as high doses, they reported it even though it meant people would buy less.
Industry-sponsored research exists and deserves scrutiny. But the foundational eye supplement research comes from independent, government-funded sources.
Questions to Ask Your Eye Doctor
Before starting any supplement regimen, have a conversation with your ophthalmologist or optometrist. Here are the questions that will help you make informed decisions:
About Your Current Eye Health
- Do I have any early signs of AMD, even small drusen? This determines whether you need AREDS2 or lutein/zeaxanthin.
- What’s my baseline macular pigment optical density (MPOD)? Only some practices measure this, but it provides objective data on your current protection level.
- Do I have any signs of diabetic retinopathy or other retinal changes? This affects which supplements make sense for your situation.
- How severe is my dry eye, if I have it? Mild vs. severe dry eye might respond differently to supplements.
- What are my biggest risk factors for vision loss based on my exam findings and family history? This helps prioritize which supplements address your actual risks.
About Supplement Choices
- Which supplements make sense for MY eyes specifically? Don’t rely on general recommendations—get personalized guidance.
- Are there any interactions with my current medications? Especially important if you take blood thinners, diabetes medications, or immunosuppressants.
- Should I take AREDS2 or just lutein and zeaxanthin? Make sure your doctor explains the difference and which you actually need.
- What about omega-3s—do you recommend them for my situation? Get their perspective on the mixed evidence.
- Are there any supplements I should avoid given my health conditions? Some supplements are contraindicated with certain medical conditions.
About Monitoring and Follow-Up
- How often should I return for follow-up exams while taking supplements? Typically every 1-2 years for prevention, more frequently for active disease.
- What specific measurements will you track to monitor if supplements are working? MPOD, drusen progression, visual acuity, etc.
- At what point would you recommend changing my supplement regimen? Establish criteria for adjustments.
- What symptoms should prompt me to call immediately rather than waiting for my next appointment? Know warning signs of urgent problems.
About Practical Considerations
- Do you recommend specific brands or formulations? Some doctors have experience with particular products.
- Can I buy generic versions or do I need name brands? Get guidance on when generic is fine vs. when specific brands matter.
- Will insurance cover any of these supplements or related testing? Usually no, but worth asking.
- If I can only afford one supplement, which should I prioritize? Real-world budget constraints matter.
Taking these questions to your appointment ensures you leave with actionable, personalized guidance rather than generic advice.
Your Personalized Action Plan: Start Here
Feeling overwhelmed? Here’s a simple, step-by-step approach to getting started.
Week 1: Assessment Phase
Day 1-2: Schedule a comprehensive dilated eye exam if you haven’t had one in the past year. Request specific assessment for:
- AMD signs (drusen count and size)
- Dry eye severity
- General retinal health
Day 3-4: Track your current symptoms for three days:
- Eye fatigue level at end of work day (1-10 scale)
- Dry eye discomfort (frequency and severity)
- Difficulty with night driving or glare
- Any vision changes you’ve noticed
Day 5-7: Review your current diet:
- How many times weekly do you eat leafy greens?
- How often do you eat fatty fish?
- Do you eat eggs regularly?
- Track one full day of eating to estimate lutein intake using the food table in this article
Week 2: Food-Based Approach
Before buying supplements, try improving your diet for one week.
Daily goal:
- One serving of cooked leafy greens (kale, spinach, collards)
- Two eggs prepared any way you like
- One serving of colorful vegetables (peppers, squash, corn)
Why start here: You might find you can meet your lutein needs through food, saving supplement costs. Even if you ultimately supplement, improving your diet provides additional nutrients beyond what pills offer.
Track results: Note any changes in energy, eye comfort, or overall well-being.
Week 3: Begin Supplement Protocol
Based on your eye exam results and risk factors, start the appropriate supplements:
If your doctor found early/intermediate AMD:
- Start AREDS2 formula at label-recommended dose
- Take with breakfast or lunch containing some fat
- Set phone reminder for daily consistency
If your eyes are healthy but you have risk factors:
- Start lutein (10mg) + zeaxanthin (2mg)
- Take with a meal containing fat
- Continue eating greens when possible
If you have significant eye strain from computer work:
- Add astaxanthin (6-12mg) to lutein/zeaxanthin
- Take with fatty breakfast or lunch
- Give it 4 weeks before assessing benefit
If you have dry, uncomfortable eyes:
- Start maqui berry extract (60mg standardized)
- Can take with or without food
- Track symptom severity weekly
Month 2: Assess and Adjust
Week 5-8: Continue your initial protocol consistently.
Track weekly:
- Symptom levels (same metrics from Week 1)
- Any side effects (stomach upset, skin changes, etc.)
- Compliance (did you remember to take it daily?)
- Cost (is this sustainable long-term?)
Look for early changes:
- Astaxanthin: Should show effects by week 8-12
- Maqui berry: Should show effects by week 6-8
- Lutein/zeaxanthin: Don’t expect noticeable changes yet
- AREDS: Don’t expect noticeable changes—this prevents future progression
Month 3: Establish Long-Term Plan
Week 9-12: Decide what’s working and what’s not.
Continue indefinitely:
- Supplements showing clear benefit
- AREDS2 if you have AMD (must continue for ongoing benefit)
- Lutein/zeaxanthin for prevention (long-term investment)
Reassess or discontinue:
- Supplements showing zero benefit after adequate trial
- Astaxanthin if eye strain hasn’t improved by week 12
- Maqui berry if dry eye unchanged by week 8
Schedule next eye exam:
- In 6-12 months if you have AMD or high risk factors
- In 1-2 years if using supplements for prevention
- Sooner if you notice any vision changes
Month 6-12: Monitor Progress
For lutein and zeaxanthin: Consider MPOD testing at 6-12 months if available. This provides objective confirmation that supplementation is increasing your macular pigment density.
For AREDS2: Your eye doctor will check for AMD progression at follow-up exams. Stable disease or slower progression than expected indicates the supplement is working.
For astaxanthin and maqui berry: Ongoing symptom relief indicates benefit. If symptoms return, ensure you haven’t skipped doses or switched to a lower-quality product.
Adjust as needed: If a supplement clearly isn’t working after adequate trial, stop it. Put that money toward higher-quality versions of supplements that are working, or toward more nutrient-dense foods.
Cost Management Strategies
If budget is tight, prioritize:
- Most important: Address diagnosed conditions (AREDS2 for AMD)
- High value: Lutein/zeaxanthin for prevention if you have risk factors
- Quality of life: Astaxanthin or maqui berry if symptoms significantly impact daily life
- Lower priority: Experimental supplements like saffron for early AMD
Money-saving tactics:
- Buy 3-6 month supplies when on sale (if formula is stable)
- Choose store brands that match proven formulas
- Split large bottles with family members who need the same supplements
- Use FSA/HSA funds if available (some accounts allow supplement purchases)
Tracking Progress: Simple Worksheet
Create a simple spreadsheet or notebook with these columns:
- Date
- Supplements taken (which ones, doses)
- Symptoms (scale 1-10)
- Side effects (if any)
- Monthly cost
- Notes (anything unusual)
Review monthly to identify patterns and make informed decisions.
Conclusion
The supplement aisle is full of promises. But only a handful of products have solid science behind them.
The proven winners:
- AREDS2 formula for slowing AMD progression in people with intermediate or advanced disease
- Lutein and zeaxanthin for building macular pigment and likely reducing AMD risk
- Astaxanthin for reducing digital eye strain and improving focusing ability
- Maqui berry for increasing natural tear production in dry eye
The emerging options with promise:
- Saffron for early AMD (small studies, consistent results, needs confirmation)
- Alpha-lipoic acid for diabetic eye disease (moderate evidence, low risk)
The disappointments:
- Bilberry (weak evidence despite decades of use)
- Isolated vitamin A (unnecessary and potentially dangerous)
- Ginkgo (inconsistent results, interaction risks)
- High-dose omega-3s for AMD (AREDS2 found no benefit)
The critical distinctions most articles miss:
- AREDS2 only works for existing AMD, not prevention
- Lutein and zeaxanthin work for prevention, not treatment
- Astaxanthin targets muscles, not retina
- Beta-carotene in old formulas increases cancer risk in smokers
The biggest mistakes people make:
- Taking AREDS formulas when they don’t have AMD
- Giving up on supplements after just a few weeks
- Choosing underdosed products based on marketing
- Ignoring food sources entirely
- Not getting baseline eye exams before starting
What to do right now:
- Schedule a comprehensive eye exam if you haven’t had one recently
- Start lutein (10mg) and zeaxanthin (2mg) if you have any AMD risk factors
- Add astaxanthin if computer work exhausts your eyes
- Try maqui berry if dry eyes bother you daily
- Focus on eating leafy greens 4-5 times weekly regardless of supplement choices
- Give supplements adequate time to work (3-12 months depending on type)
- Track costs and benefits to make informed long-term decisions
Most importantly: supplements complement healthy habits, they don’t replace them. Wear sunglasses outdoors to block UV. Take breaks from screens every 20 minutes (20-20-20 rule). Don’t smoke—it multiplies all eye disease risks. Control blood sugar and blood pressure. Get regular exercise.
Your eyes are remarkable organs. They convert photons into electrical signals your brain interprets as reality. They allow you to read these words, recognize loved ones’ faces, and witness sunsets. They deserve evidence-based care, not marketing-driven guesswork.
Now you know what actually works—and what’s just expensive wishful thinking. Use this information to make choices that protect your vision for decades to come.
FAQs
What is the number one supplement for eye health?
The answer depends on your specific situation. For people with intermediate or advanced AMD, the AREDS2 formula is the only supplement proven to slow vision loss. For everyone else, lutein (10mg) and zeaxanthin (2mg) have the strongest prevention evidence and broadest benefit. If you take just one supplement for general eye health, make it lutein and zeaxanthin.
Can supplements improve your eyesight?
Supplements can slow vision loss from conditions like AMD, but they don’t improve refractive errors (nearsightedness, farsightedness) or restore vision already lost to disease. Some supplements like astaxanthin improve functional vision (less fatigue, better focusing) rather than making your prescription better. Think of supplements as disease prevention and management tools, not vision correction.
What is the best vitamin for blurry vision?
This depends on what’s causing blurriness. For AMD-related blur, the AREDS2 formula slows progression. For strain-related blur after computer work, astaxanthin (6-12mg) improves focusing ability. For dry eye blur that improves with blinking, maqui berry increases tear production. Get an eye exam to identify the cause before choosing supplements.
Are eye vitamins worth taking?
For specific groups, absolutely yes. AREDS2 reduces AMD progression by 25%—that’s substantial. Lutein and zeaxanthin reduce late AMD risk by 26% in observational studies. For people with these conditions or high risk factors, supplements are definitely worth the modest cost. For young people with healthy eyes, excellent diets, and no risk factors, food-based approaches might suffice.
Can you take too much lutein?
No upper limit has been established because no toxicity has been observed even at high doses (20mg+ daily) taken for years. The only documented side effect is harmless yellowing of the skin (carotenodermia) that reverses when you stop. That said, studies show maximum benefit at 10-20mg daily, so taking mega-doses provides no additional benefit.
Do eye supplements really work?
Some do, some don’t. AREDS2 formula works for AMD—this is proven in large clinical trials. Lutein and zeaxanthin work for building macular pigment and likely reduce AMD risk. Astaxanthin works for eye strain. Maqui berry works for dry eye. But bilberry, ginkgo, and isolated vitamin A have weak or negative evidence. The key is matching supplements with strong evidence to your specific condition.
What foods are highest in lutein?
Cooked kale leads at 23.7mg per cup, followed by cooked spinach (20.4mg per cup), collard greens (14.6mg per cup), and turnip greens (12.2mg per cup). Among non-leafy vegetables, cooked zucchini provides 2.5mg per cup. Egg yolks contain only 0.15mg per yolk but in a highly bioavailable form that absorbs 3-4 times better than plant sources.
How long does it take for eye vitamins to work?
Astaxanthin for eye strain: 4-12 weeks. Maqui berry for dry eye: 30-60 days. Lutein and zeaxanthin for macular pigment: 6-12 months for full effect. AREDS formula for AMD: benefits accumulate over years of continuous use. Most supplements require consistent daily intake for months before showing measurable results. Patience is essential.
Can supplements prevent macular degeneration?
Evidence suggests lutein and zeaxanthin reduce risk of developing late-stage AMD by about 26%, but they don’t prevent AMD entirely. No supplement has been proven to prevent AMD from starting in people with healthy eyes. The AREDS2 formula slows progression of existing intermediate AMD but doesn’t prevent the condition from developing. Think of supplements as risk reduction tools, not guarantees.
Are expensive eye supplements better than cheap ones?
Not necessarily. What matters is ingredient amounts, chemical forms, and quality verification—not price. Many expensive brands are manufactured in the same facilities as store brands. A $15 generic with proper AREDS2 doses and USP verification is better than a $50 name brand with proprietary blends and underdosed ingredients. Compare labels, not prices.



