Most people assume cognitive decline is a problem for their 70s or 80s. By that logic, protecting your brain is something you’ll get around to later. That assumption is wrong, and it’s costing people decades of opportunity.
The damage doesn’t start in old age. It starts in middle age, quietly, while life feels completely normal. That’s the real story, and it changes everything about when you need to act.
The Midlife Wake-Up Call
A landmark study published in the British Medical Journal tracked roughly 7,400 adults from the Whitehall II cohort across three assessment points over 10 years. The findings were striking. Researchers led by Singh-Manoux and colleagues found that measurable cognitive decline begins as early as age 45. Not 65. Not 75. Forty-five.

That shifts the entire conversation. Midlife isn’t a waiting room before the real risk begins. It’s the most important window you have to protect your brain.
The brain isn’t a fixed machine that simply wears down. It retains what scientists call neuroplasticity, the ability to reshape itself throughout life. A review by Pascual-Leone and colleagues in the Annual Review of Neuroscience showed that the brain’s structural maps are continually shaped by experience and mental training across the lifespan. You can build a biological buffer right now.
The six habits below aren’t wellness tips. They’re some of the most consistent findings in brain health research, drawn from clinical trials, long-term cohort studies, and randomized controlled trials involving tens of thousands of people.
Habit 1: Feed Your Brain the Right Architecture
What the Research Shows
Diet may be the single most powerful tool you have. A 10-year cohort study published in the British Medical Journal by Jia and colleagues followed nearly 29,000 adults aged 60 and older across five assessment waves. Among the six lifestyle factors tracked, a healthy diet had the strongest independent effect on slowing memory decline.

What makes this finding especially important is who it helped. The protective effect held even for people carrying the APOE ε4 gene variant, which is considered a high-risk genetic marker for Alzheimer’s disease. In fact, adults who maintained the most favorable lifestyle scores had an 89 percent lower risk of progressing to mild cognitive impairment or dementia compared to those with the least favorable scores (hazard ratio 0.11). A separate meta-analysis in Ageing Research Reviews by Veronese and colleagues, pooling data from nine longitudinal cohort studies, found that higher adherence to the Mediterranean diet was consistently linked to better cognitive function and reduced risk of decline across multiple populations.
What to Do
Drop processed and ultra-processed foods. Adopt the core principles of a Mediterranean-style diet: olive oil, oily fish, leafy greens, legumes, berries, whole grains, and nuts. This isn’t a short-term protocol. Think of it as long-term fuel for the brain’s structural needs.
→ See how omega-3s support memory and cognitive function
Habit 2: Reverse the Atrophy Clock With Aerobic Exercise
What the Research Shows
“Stay active” is advice so vague it’s almost useless. The science gets far more specific. A randomized controlled trial published in the Proceedings of the National Academy of Sciences by Erickson and colleagues assigned 120 older adults to either an aerobic walking program or a stretching control group for one year.
The aerobic group saw hippocampal volume increase by roughly two percent. The hippocampus is the brain region most closely tied to memory. That two percent increase effectively reversed approximately one to two years of age-related brain atrophy. The stretching control group continued to show volume decline.

There’s an important nuance here. A separate analysis of the Whitehall II cohort by Kivimäki and colleagues, published in the BMJ, found no evidence of a neuroprotective effect from physical activity when cardiometabolic health was not accounted for. Exercise works best as part of a broader healthy lifestyle, not as a single fix. Your blood pressure, blood sugar, and cholesterol matter too.
What to Do
Commit to activities that genuinely raise your heart rate. Walking, cycling, swimming, and jogging all count. The goal is sustained aerobic output, not gentle movement. Think 150 minutes or more per week, paired with attention to your overall cardiovascular health.
Habit 3: Fix Your Sleep Quality, Not Just Your Hours
What the Research Shows
Eight hours of time in bed is not the same as eight hours of restorative sleep. This is where most sleep advice falls short.
A longitudinal study drawing from the Study of Osteoporotic Fractures cohort, cited in research published in Neurology, tracked over a thousand older women and examined not just how long they slept but how well. Women with sleep efficiency below 70 percent, meaning less than 70 percent of their time in bed was actually spent asleep, faced between 61 and 96 percent higher odds of cognitive impairment depending on the measure used, with risk nearly doubling on tests of processing speed and executive function. It was sleep fragmentation and disturbance, not simply short duration, that drove the risk.
What to Do
Focus on the quality of your sleep, not just the quantity. Reduce stimulants in the evening. Keep your bedroom cool and dark. Build a consistent wind-down routine that reduces the time it takes to fall asleep. If you wake frequently in the night, investigate why. Sleep apnea, for example, is a common and treatable cause of fragmented sleep that significantly raises cognitive risk.
Habit 4: Force Your Brain to Redraw Its Maps
What the Research Shows
The brain is efficient by design. It builds well-worn pathways for the things you do repeatedly and expends less energy over time on familiar tasks. That efficiency is useful in daily life, but it doesn’t build cognitive reserve. Reserve is what protects you when the brain faces stress or damage.
The foundational science for this comes from the theoretical review by Pascual-Leone and colleagues in the Annual Review of Neuroscience. Their work showed that the brain requires constant novel sensory input and mental challenges to maintain neural efficiency and structural plasticity. Familiar routines maintain the status quo. They don’t expand it.
What to Do
Stop relying on activities that feel easy. The brain adapts quickly and stops building when a task becomes routine. High-friction learning is what drives new cognitive scaffolding. Pick up a new language. Learn a musical instrument. Work through problems in a domain that’s completely new to you. The discomfort of being a beginner is the signal that your brain is actually building something.
Habit 5: Treat Social Connection as a Medical Necessity
What the Research Shows
Social isolation isn’t just bad for mood. It’s a measurable risk factor for cognitive decline. A long-term clinical-pathologic cohort study by Bennett and colleagues, published in JAMA Neurology, followed roughly 1,400 to 1,500 older adults from the Rush Memory and Aging Project and Religious Orders Study for up to 20 years. Higher cognitive and social engagement was linked to slower cognitive decline, and crucially, this effect held even after accounting for the underlying burden of Alzheimer’s pathology in the brain.
A parallel review published in The Lancet Neurology by Fratiglioni, Paillard-Borg, and Winblad brought together findings from multiple longitudinal studies, including the Kungsholmen Project. Social networks, mental activity, and physical activity all showed convergent protective effects against dementia. The proposed mechanisms include building cognitive reserve, improving vascular health, and reducing chronic stress, all of which support brain function over time.
What to Do
Schedule meaningful social interaction with the same commitment you’d give to a gym session. Depth matters more than breadth. Strong, consistent relationships with people who engage your mind appear to offer the greatest benefit. Don’t let social connection be what gets cancelled when life gets busy.
Habit 6: Stack the Habits Together
What the Research Shows
If there’s one finding that ties all of this together, it comes from the FINGER study, published in The Lancet by Kivipelto and colleagues. This was a randomized controlled trial involving 1,260 at-risk adults aged 60 to 77 in Finland, running for two years.
Participants in the intervention group received a combined program covering diet, aerobic exercise, cognitive training, and vascular health monitoring simultaneously. The result: the intervention group improved their composite cognitive performance score by 25 percent more than the control group. This was the first large-scale randomize trial to show that combining lifestyle changes can protect cognition in at-risk older adults.

This is the key insight that most advice gets wrong. The habits listed above aren’t interchangeable options on a menu. They work as a system. Each one addresses a different biological pathway, and together they create a compounded defence that no single habit can replicate alone.
The Jia study mentioned in Habit 1 reinforces this perfectly. Across nearly 29,000 older adults tracked for a decade, every lifestyle factor independently slowed memory decline. But the more habits a person adopted, the stronger the protective effect.
What to Do
Stop looking for one change that will solve everything. Layer these habits. Start with the ones that feel most accessible, and build from there. A Mediterranean-style diet plus regular aerobic exercise plus quality sleep plus a challenging mental activity plus consistent social connection plus ongoing health monitoring is not a perfect wellness ideal. It’s what the evidence points to, consistently, across decades of research and tens of thousands of participants.
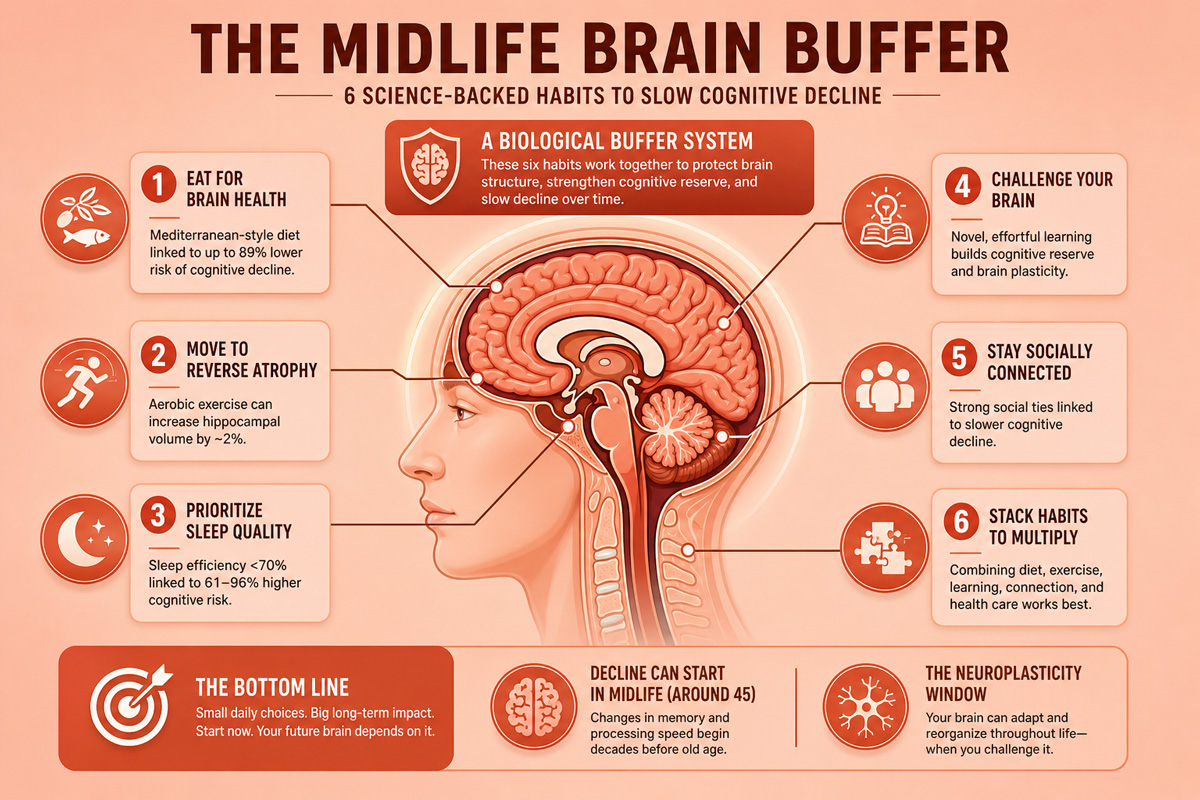
The Takeaway
Your brain is already changing. If you’re in your 40s or 50s, that process is underway. But the same research that reveals the timeline also reveals the solution.
These six habits appear in study after study because they address the actual biological mechanisms behind cognitive decline. They’re not soft wellness advice. They’re supported by randomized controlled trials, multi-decade cohort studies, and population-level data covering tens of thousands of people across multiple countries.
The question isn’t whether your brain will change with age. It will. The question is how much of that change you’re willing to influence.



